Posted by: Northwest Eye in General on August 28, 2025
Overview
Intraocular melanoma is a type of cancer that arises from melanocytes in the uvea of the eye. We understand that learning about this condition can be overwhelming. Symptoms may include:
- Blurred vision
- Dark spots on the iris
- Flashes of light, which can understandably cause concern.
It’s essential to recognize the importance of early detection. Comprehensive diagnostic methods, such as:
- Dilated eye exams
- Advanced imaging techniques
play a crucial role in improving treatment outcomes and enhancing patient care. We are here to help you through this process, ensuring you receive the support and information you need.
By prioritizing early detection, we can work together towards better health outcomes. Remember, you are not alone in this journey, and seeking care is a vital step in addressing your concerns.
Introduction
Intraocular melanoma, the most common primary eye tumor in adults, poses significant health risks that often go unnoticed until advanced stages. We understand that this can be a daunting reality for many. Recognizing the symptoms, diagnostic methods, and treatment options is crucial for early detection and effective management of this condition.
It’s common to feel overwhelmed by the complexity of medical information. However, understanding these elements can empower you to take proactive steps in your health journey. How can individuals recognize the subtle signs of this disease and navigate the often-daunting medical landscape? We are here to help you through this process.
Define Intraocular Melanoma: Risk Factors and Symptoms
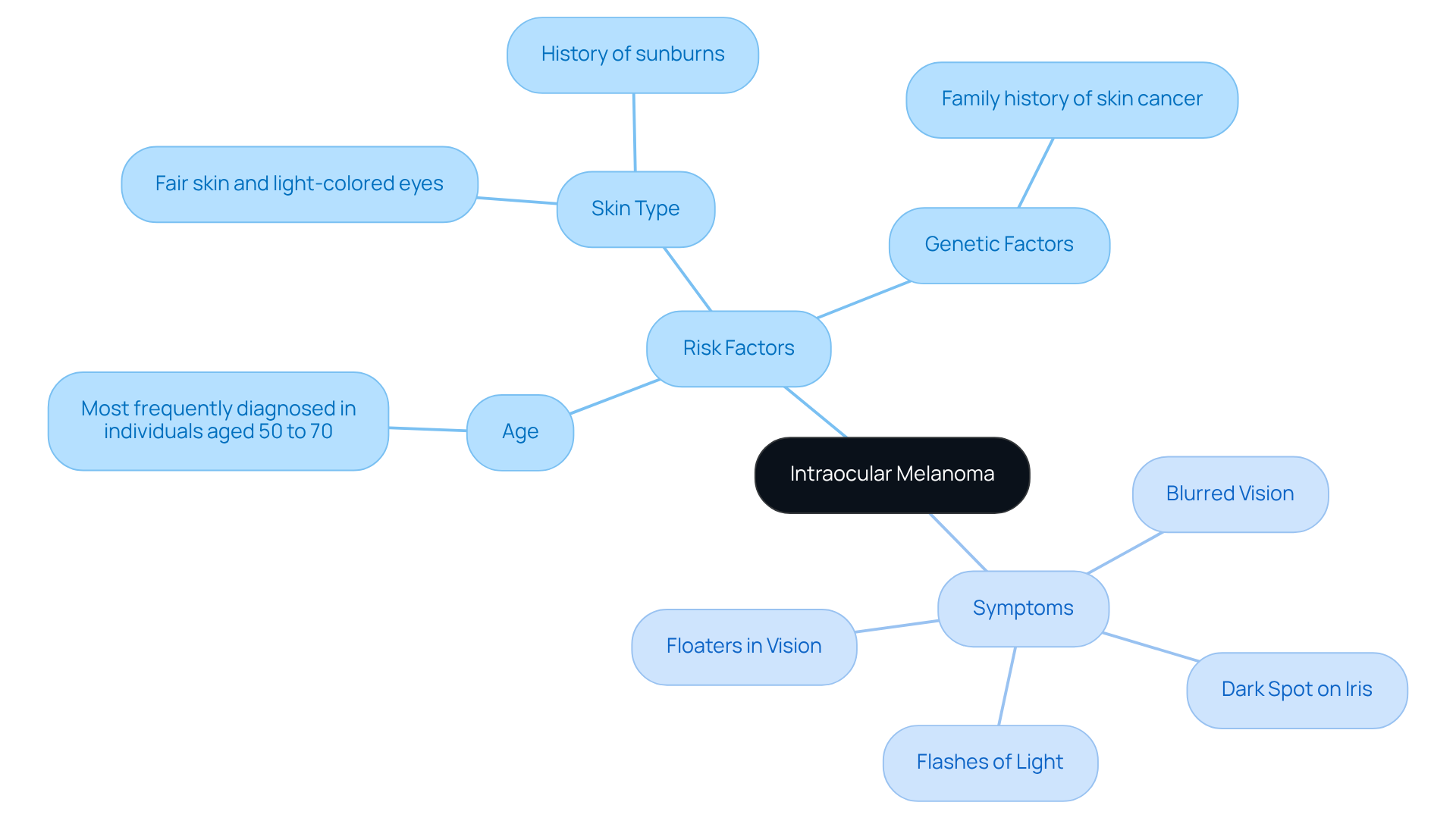
Intraocular cancer, especially uveal cancer, is the most prevalent primary eye tumor in adults. It originates from melanocytes within the uvea, which includes the iris, ciliary body, and choroid. We understand that learning about this condition can be overwhelming, so it’s important to recognize the key risk factors:
- Age: This condition is most frequently diagnosed in individuals aged 50 to 70.
- Skin Type: Those with fair skin, light-colored eyes, and a history of sunburns are at a heightened risk.
- Genetic Factors: A family history of skin cancer can significantly increase susceptibility.
Symptoms of cancer in the intraocular region can often be subtle, yet they are critical for early detection. Common indicators include:
- Blurred vision or sudden vision loss.
- A noticeable dark spot on the iris or alterations in pupil shape.
- Flashes of light or the presence of floaters in vision.
We understand that it’s common to feel anxious about these symptoms. Early recognition is vital, as it facilitates prompt medical evaluation and intervention, ultimately improving treatment outcomes. Remember, we are here to help you through this process.
Diagnose Intraocular Melanoma: Tests and Procedures
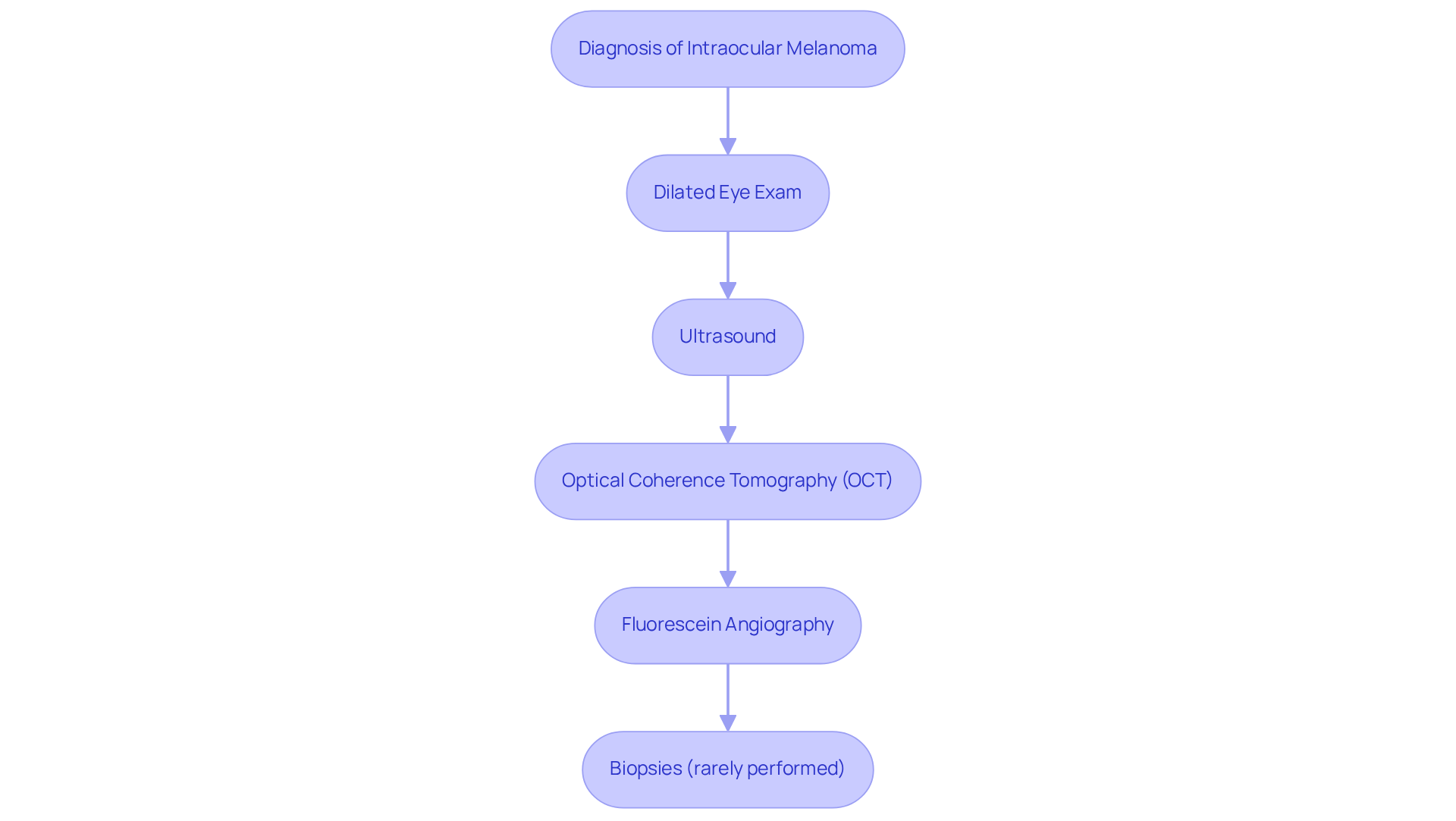
Diagnosing intraocular melanoma requires a comprehensive approach that integrates clinical examination with advanced imaging techniques, and we recognize that this process can be daunting.
- Dilated Eye Exam: An ophthalmologist uses specialized lenses to thoroughly examine the eye for tumors, making this a critical first step in diagnosis. Approximately 73 percent of cases of intraocular melanoma are detected during routine dilated eye exams, underscoring their importance. According to the American Society of Clinical Oncology (ASCO), about 73 percent of patients are diagnosed at an early stage, which significantly impacts treatment outcomes. Knowing this can provide some reassurance that early detection is possible.
- Ultrasound: This technique employs high-frequency sound waves to generate detailed images of the eye, allowing for precise evaluation of mass size and location.
- Optical Coherence Tomography (OCT): OCT provides cross-sectional images of the retina, revealing intricate structural details that can indicate the presence of tumors.
- Fluorescein Angiography: This involves injecting a dye into the bloodstream to visualize blood flow in the eye, helping to detect any irregularities related to intraocular conditions.
While biopsies can , they are seldom conducted for intraocular tumors because of the associated risks, including possible complications from the procedure. We want you to know that the combination of these diagnostic methods is essential for early detection and effective management of this serious condition. Remember, you are not alone in this journey; we are here to help you through this process.
Explore Treatment Options for Intraocular Melanoma
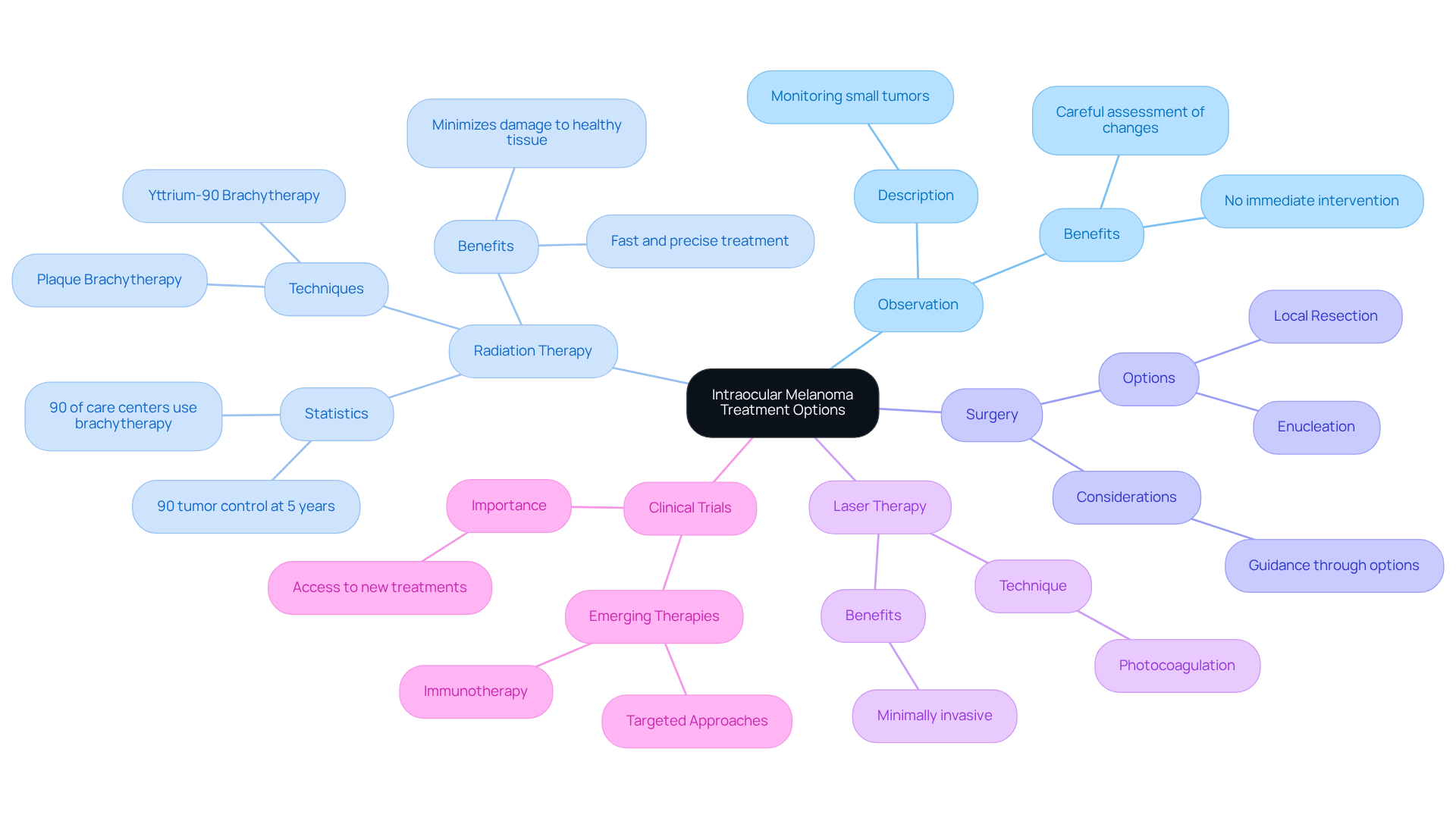
Treatment for melanoma is tailored with great care, considering the tumor’s size and location within the intraocular region. We understand that this can be a challenging time, and several effective options are available to you:
- Observation: For small tumors, we may choose to monitor your condition closely without immediate intervention. This allows us to assess any changes carefully and ensure you feel supported throughout the process.
- Radiation Therapy: Techniques like plaque brachytherapy deliver targeted radiation directly to the tumor, effectively controlling its growth while minimizing damage to surrounding healthy tissue. This method has shown promising outcomes, with studies indicating that 90% of patients maintain five years post-treatment. It’s reassuring to know that around 90% of care centers generally utilize brachytherapy for uveal melanoma, highlighting its commonality and acceptance in clinical practice. Recent advancements, particularly the introduction of yttrium-90 brachytherapy, have revolutionized care, providing rapid, precise treatment that can often be completed in just minutes.
- Surgery: For larger growths, local resection may be performed to remove the mass, or in more severe cases, enucleation (removal of the eye) may be necessary. We are here to guide you through these options and ensure you feel informed and supported.
- Laser Therapy: Photocoagulation uses laser light to destroy tumor cells, offering a minimally invasive option for certain patients. This can be a comforting choice for those seeking less invasive treatment.
Clinical trials may provide you with access to emerging therapies, including immunotherapy and targeted approaches, which are currently being evaluated for their effectiveness in managing intraocular melanoma. We encourage you to explore these options as they may provide new hope.
Each care option carries its own benefits and risks, which is why a multidisciplinary approach is essential in developing the most suitable plan for you. It’s important to be aware that common side effects of radiation therapy can include radiation retinopathy and radiation optic neuropathy, potentially leading to blurred vision and other complications. Regular dilated eye exams and prompt evaluation of any vision changes are crucial for early detection of ocular cancers.
As Dr. Louis Potters describes, the yttrium-90 technology is a ‘game-changer’ for ocular cancer care, significantly enhancing patient outcomes. We are here to help you through this process, ensuring you feel supported and informed every step of the way.
Understand Follow-Up Care and Monitoring After Treatment
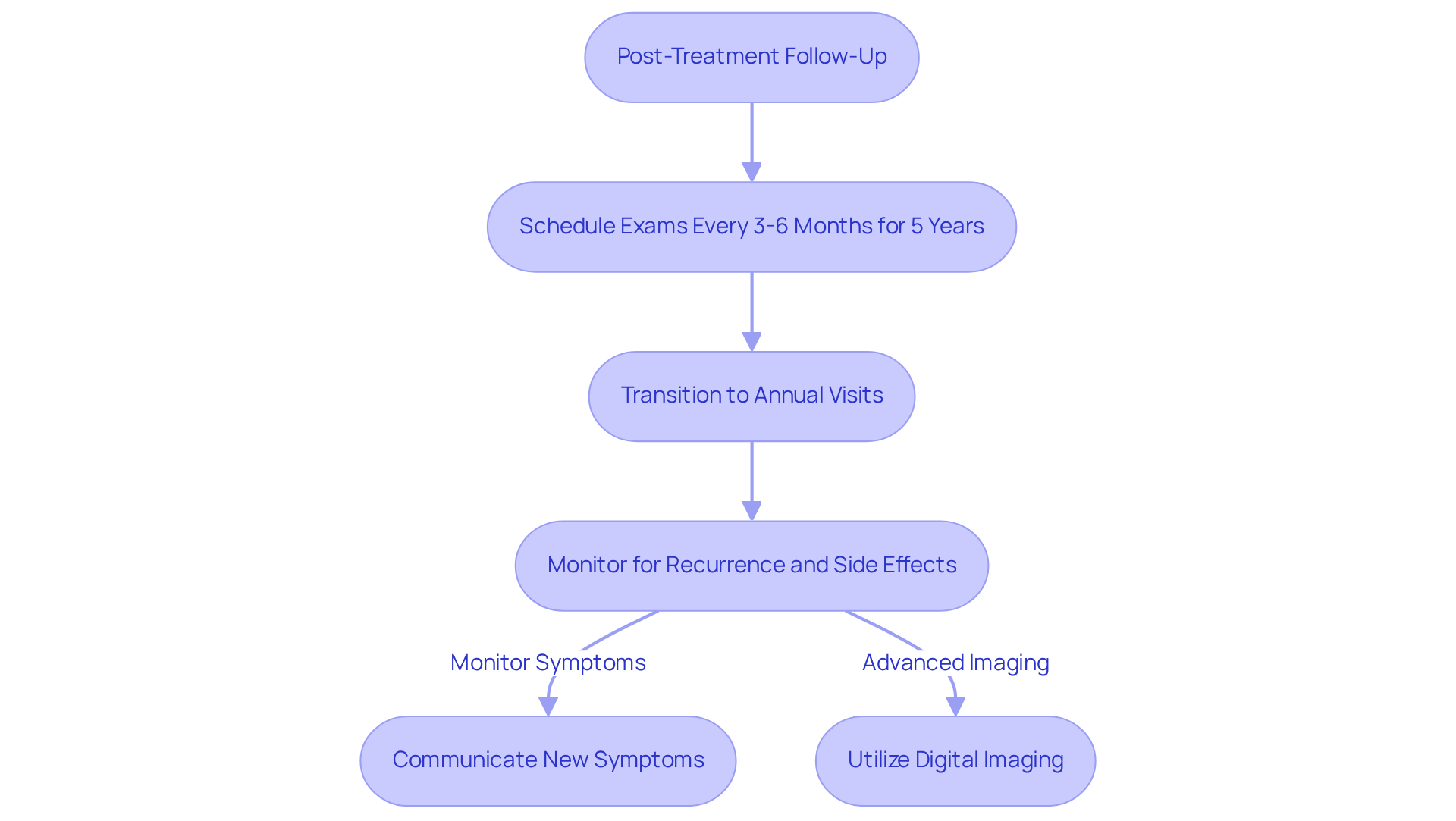
Post-treatment follow-up for ensuring optimal patient outcomes is essential for intraocular tumors. We understand that navigating this journey can be challenging, and patients are generally advised to schedule follow-up exams every 3 to 6 months during the first five years after treatment, transitioning to annual visits thereafter. These appointments are vital for monitoring potential recurrence or metastasis through comprehensive eye exams and advanced imaging tests. Research indicates that digital imaging systems have revolutionized fundus imaging, enhancing the accuracy of monitoring eye conditions.
In addition to surveillance for cancer recurrence, follow-up care plays a crucial role in managing any treatment-related side effects, such as changes in vision or discomfort. It’s common to feel uncertain about new symptoms, and patients are encouraged to maintain open lines of communication with their healthcare team, promptly reporting any new concerns. As noted by Wrobleski et al., the automatic classification of perimetry data may be useful for glaucoma screening, which can be relevant in the context of monitoring for recurrence. This proactive engagement can significantly enhance long-term outcomes and improve overall quality of life, highlighting the importance of in the management of intraocular conditions such as melanoma.
Furthermore, we recognize the challenges associated with data management and storage in follow-up care. The need for substantial storage capacity for imaging data highlights the complexities involved in monitoring eye cancer patients. We are here to help you through this process, ensuring that you receive the support and care you deserve.
Conclusion
Intraocular melanoma is a significant health concern, particularly as it stands as the most common primary eye tumor in adults. We understand that learning about this condition can be overwhelming, which is why understanding the risk factors, symptoms, and available treatment options is crucial for early detection and effective management. Recognizing symptoms such as blurred vision or changes in the iris can empower individuals to seek timely medical evaluation, essential for improving outcomes.
This article outlines a comprehensive approach to diagnosing and treating intraocular melanoma. Key diagnostic methods include:
- Dilated eye exams
- Ultrasound
- Advanced imaging techniques
These collectively enhance the chances of early detection. Treatment options vary, from careful observation for small tumors to advanced therapies like radiation and laser treatment for larger growths. We emphasize the importance of a tailored approach, considering each patient’s unique circumstances and the potential for emerging therapies through clinical trials.
Ultimately, we want to highlight that proactive engagement in follow-up care is vital for monitoring recurrence and managing any treatment-related side effects. Regular check-ups and open communication with healthcare professionals can significantly improve long-term outcomes and quality of life for patients. By staying informed about the latest research and treatment options for intraocular melanoma, individuals can empower themselves and their loved ones to navigate this challenging journey with confidence and support.
Frequently Asked Questions
What is intraocular melanoma?
Intraocular melanoma is the most prevalent primary eye tumor in adults, originating from melanocytes within the uvea, which includes the iris, ciliary body, and choroid.
What are the main risk factors for developing intraocular melanoma?
The main risk factors include age (most frequently diagnosed in individuals aged 50 to 70), skin type (higher risk for those with fair skin, light-colored eyes, and a history of sunburns), and genetic factors (family history of skin cancer).
What are the common symptoms of intraocular melanoma?
Common symptoms include blurred vision or sudden vision loss, a noticeable dark spot on the iris or changes in pupil shape, and flashes of light or floaters in vision.
Why is early detection of intraocular melanoma important?
Early recognition of symptoms is vital as it facilitates prompt medical evaluation and intervention, ultimately improving treatment outcomes.






