Posted by: Northwest Eye in Cataracts on March 3, 2026
Introduction
Low eye pressure, or hypotony, is a condition that can deeply affect your visual health, and it often goes unnoticed until complications arise. We understand that this can be concerning. That’s why it’s so important to maintain appropriate intraocular pressure (IOP), as it plays a vital role in preserving the structure and function of your eyes.
What steps can you take to effectively manage low eye pressure and protect your vision? In this article, we’ll explore practical strategies for:
- Monitoring your eye pressure
- Identifying underlying causes
- Making lifestyle changes that can enhance your overall eye health
Remember, you’re not alone in this journey, and we are here to help you through the process.
Understand Low Eye Pressure: Definition and Importance
hypotony, clinically known as hypotony, can be concerning. It occurs when eye pressure falls below the normal range of 12 to 22 mm Hg, highlighting the importance of careful monitoring and management of your ocular tension. We understand that maintaining appropriate intraocular pressure is vital for your overall eye health, as it helps preserve the eye’s shape and ensures essential nutrients reach ocular tissues.
When eye pressure falls too low, it can lead to symptoms such as pain and discomfort. In severe cases, low eye pressure can lead to structural damage to the eye, potentially resulting in irreversible vision loss. Recent studies indicate that routine eye assessments, known as eye exams, can arise from various factors, including surgical complications and inflammation. This highlights the risk of hypotony maculopathy.
For instance, complications like retinal detachment can develop when low eye pressure causes the scleral wall to collapse, leading to chronic hypotony. We want you to know that understanding these risks is crucial. Regular check-ups can help identify issues early, allowing for timely action that can significantly reduce the likelihood of serious eye health problems. Remember, we are here to help you through this process.
Identify Causes of Low Eye Pressure: Key Factors to Consider
Several factors can contribute to low eye pressure, including:
- Post-surgical complications: Eye surgeries, especially those involving the retina or cataracts, can lead to hypotony if there are leaks at the surgical site. Robert Weinberg, MD, notes that hypotony after cataract surgery is rare, but it can occur and may result in irreversible structural changes, such as corneal edema and macular edema, significantly affecting vision. A case study emphasizes the importance of recognizing and managing postoperative hypotony to prevent long-term damage.
- Chronic inflammation: Conditions like uveitis can disrupt the production and drainage of aqueous humor, leading to lower intraocular pressure (IOP). Chronic inflammation is prevalent in various eye conditions, and its management is crucial for maintaining healthy eye pressure. For instance, uveitis can lead to significant fluctuations in IOP, necessitating careful monitoring and treatment. Recent findings indicate that chronic inflammation can significantly affect eye pressure, highlighting the need for awareness among patients.
- Retinal detachment: This serious condition can disrupt normal fluid dynamics in the eye, potentially resulting in low IOP. Early detection and intervention are vital to prevent complications associated with retinal detachment.
- Medications: Certain medications, particularly those prescribed for glaucoma, can inadvertently lower eye pressure. Understanding the side effects of these medications is essential for patients to manage their eye health effectively. Notably, cataract surgery has been shown to reduce the mean number of ocular hypotensive medications needed by half up to 6 years postoperatively, providing valuable context for managing low eye pressure post-surgery.
Recognizing these causes is crucial for individuals at risk, particularly those with a history of eye surgery or chronic eye conditions. Awareness and timely intervention can help mitigate the risks associated with low eye pressure.
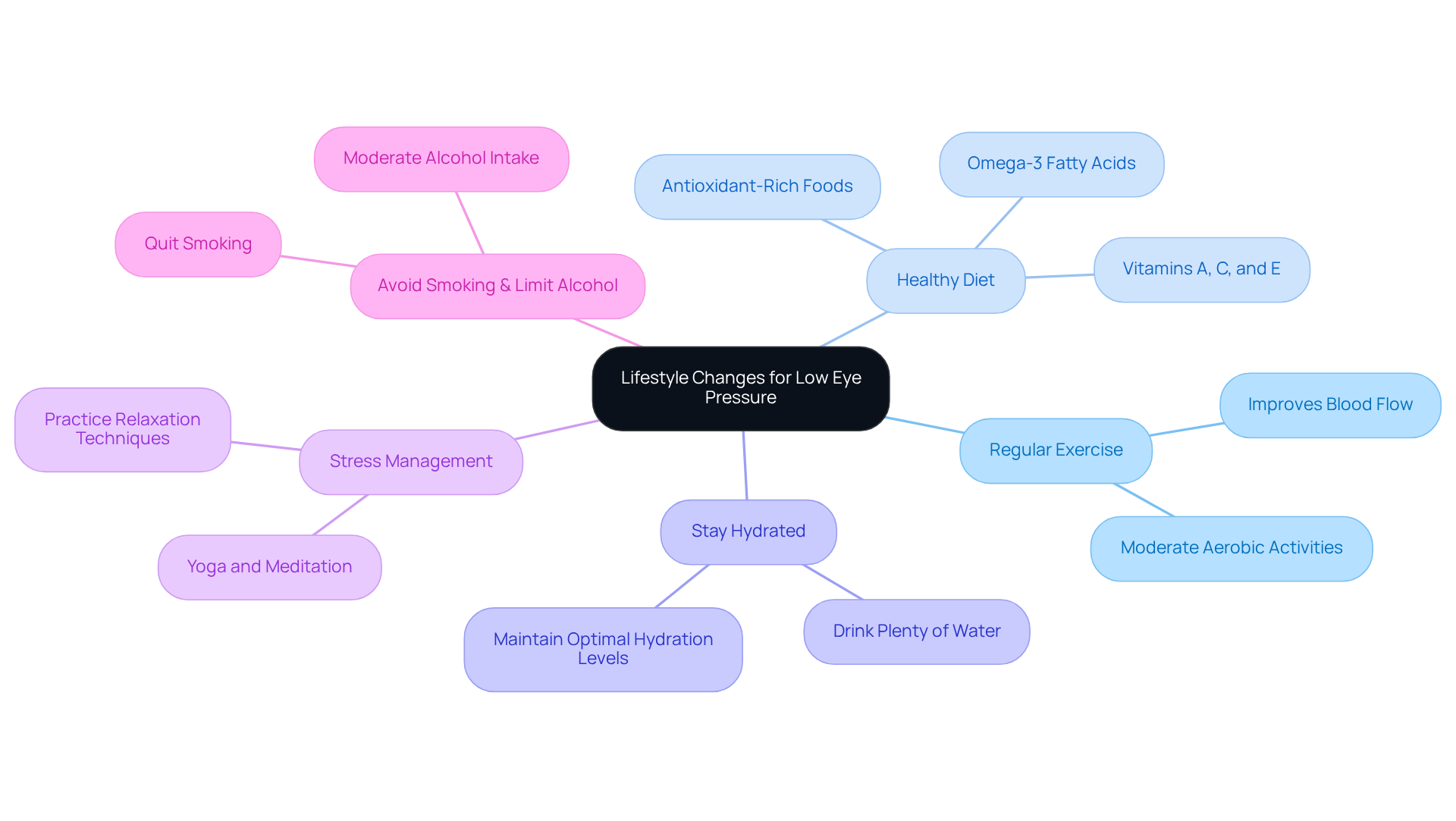
Implement Lifestyle Changes: Tips for Managing Low Eye Pressure
To manage low eye pressure effectively, consider the following lifestyle changes:
- Regular Exercise: Engage in moderate aerobic activities like walking, swimming, or cycling, which can help improve blood flow and potentially lower IOP.
- Healthy Diet: Incorporate foods rich in antioxidants, omega-3 fatty acids, and vitamins A, C, and E. Leafy greens, fish, nuts, and fruits are excellent choices.
- [Stay Hydrated](https://nweyeclinic.com/how-to-relieve-an-irritated-eye-that-feels-like-something-is-in-it/): Drink plenty of water throughout the day to maintain optimal hydration levels, which can support overall eye health.
- Stress Management: Practice relaxation techniques such as yoga or meditation to reduce stress, which can positively influence eye pressure.
- Avoid Smoking and Limit Alcohol: Both smoking and excessive alcohol consumption can negatively affect eye health. Quitting smoking and moderating alcohol intake can be beneficial.
Consult Healthcare Professionals: Seeking Expert Guidance
If you suspect low eye pressure or experience concerning symptoms, consulting a healthcare professional is essential. Follow these steps to ensure a productive visit:
- Schedule an Appointment: Reach out to your ophthalmologist to discuss your symptoms and concerns. Early intervention can significantly impact your eye health.
- Prepare for Your Visit: Bring a log of your eye pressure readings and notes on any symptoms you’ve experienced. This information will help your doctor assess your situation more effectively.
- Ask Questions: Engage in a dialogue with your doctor about potential causes of low eye pressure, available treatment options, and lifestyle changes that may assist in managing your condition. Effective communication is key to understanding your health.
- Follow Recommendations: Adhere to your healthcare provider’s advice regarding monitoring, medications, and lifestyle adjustments. Consistent follow-up and compliance with recommendations are crucial for achieving optimal outcomes in your eye health.






