Posted by: Northwest Eye in Retinal Health and Diseases on April 9, 2026
Introduction
Retinal detachment isn’t just a medical condition; it can profoundly change the way you see the world and how you live your life. We understand that facing this challenge can be overwhelming, and that’s why it’s crucial to grasp the intricacies of recovery from this serious eye surgery. This article aims to guide you through the multifaceted journey of healing, comparing initial experiences, long-term outcomes, and the various surgical options available.
It’s common to feel anxious about what lies ahead after surgery. What challenges might arise during your recovery? How can you best navigate this process to maximize your vision restoration? We’re here to help you through this process, providing the support and information you need to feel reassured and empowered.
Understanding Retinal Detachment and Surgical Options
Retinal detachment can be a frightening experience. It occurs when the light-sensitive membrane, a delicate layer at the back of your eye, separates from the supportive tissue beneath it. If not treated promptly, this condition can lead to permanent vision loss. We understand that you may have many questions and concerns about what this means for you.
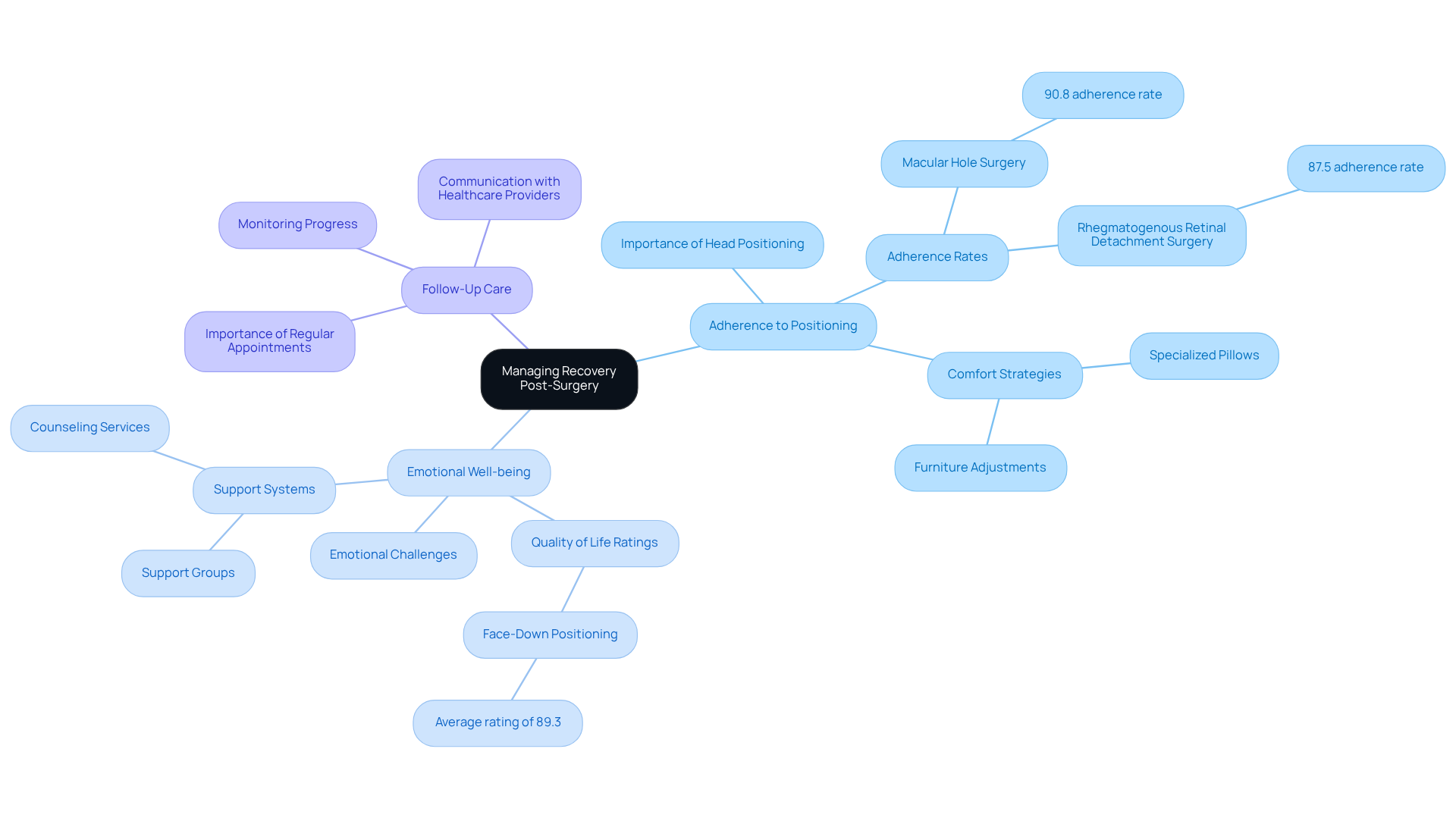
Fortunately, there are several surgical options available to repair a detached retina. Here are a few methods that your ophthalmic surgeon might discuss with you:
- Scleral Buckling: This procedure involves placing a silicone band around the eye. This band gently pushes the wall of the eye against the light-sensitive tissue, helping it to reattach.
- Vitrectomy: In this surgery, the vitreous gel that may be pulling on the light-sensitive layer is removed. This allows the retina to settle back into its proper position.
- Pneumatic Retinopexy: A gas bubble is injected into the eye to push the retina back into place. This is often followed by laser treatment to seal the retina securely.
Each of these methods has its own benefits and risks, which is why it’s essential to have a thorough discussion with a qualified ophthalmic surgeon. They can help you determine the best approach for your individual situation. Remember, you’re not alone in this journey; we are here to help you through the process.
Post-Operative Recovery: Initial Experiences After Surgery
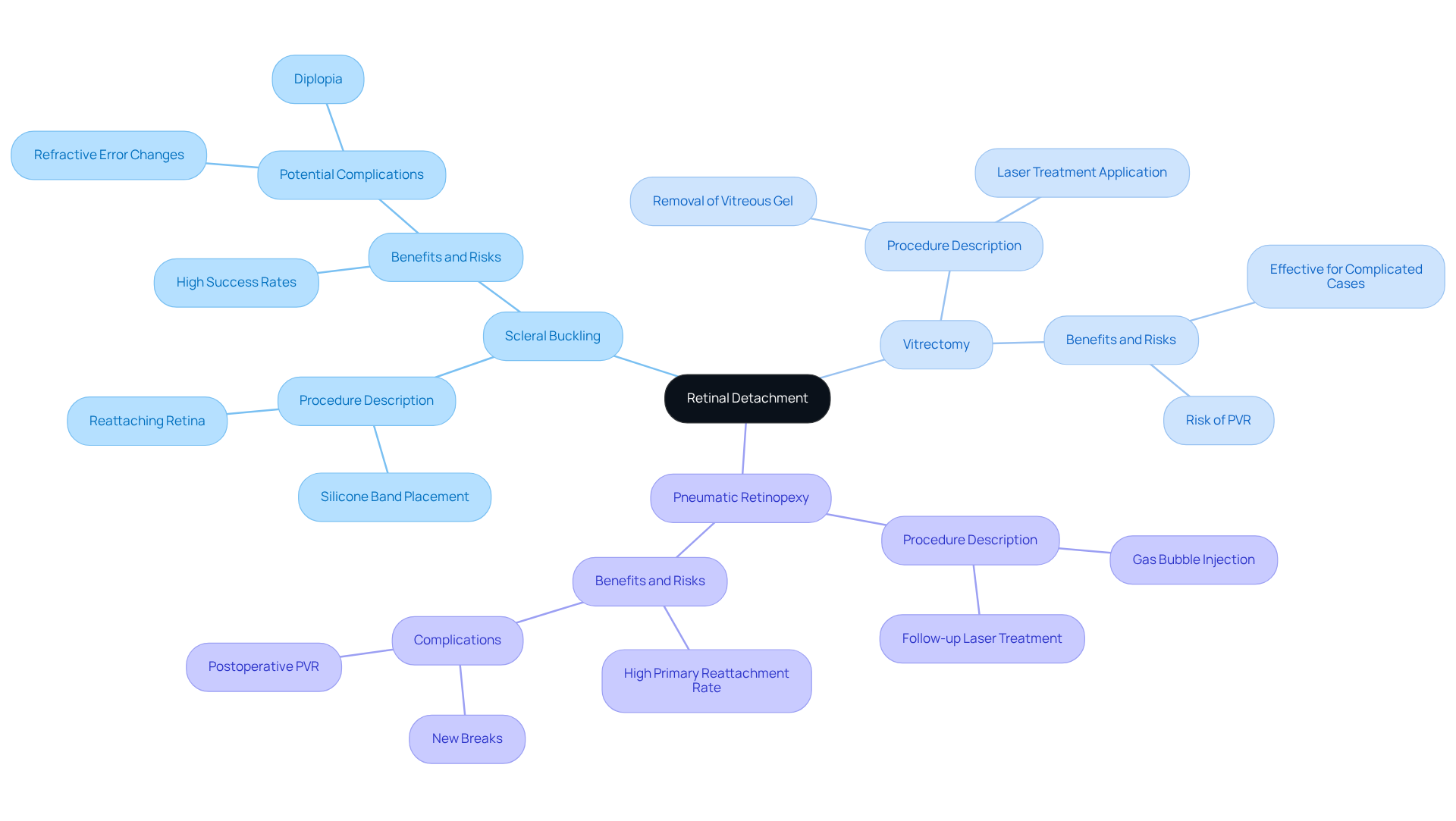
It’s completely normal to experience a variety of initial recovery symptoms before and after retinal detachment eye surgery that can impact your healing journey. We understand that this can be a challenging time, and we’re here to support you. Here are some common experiences you might encounter:
- Discomfort and Pain: While mild discomfort is often reported, severe pain is quite rare. Most individuals find relief through prescribed pain medications, helping to manage any discomfort effectively.
- Visual Changes: Blurred vision is a typical occurrence shortly after surgery, and it can be unsettling. It’s important to remember that fluctuations in your vision are common during this initial healing phase.
- Positioning Requirements: Depending on the surgical technique used, you may need to maintain specific head positions, such as face-down positioning, to encourage optimal healing. We know this can be tough, but following these guidelines is crucial for a successful recovery.
We encourage you to closely follow your surgeon’s post-operative instructions to maximize your chances of achieving the best possible outcomes. Regular follow-up visits are essential, as they allow for monitoring your progress and addressing any concerns that may arise. Remember, you’re not alone in this journey; we’re here to help you every step of the way.
Long-Term Recovery Outcomes: Comparing Patient Experiences
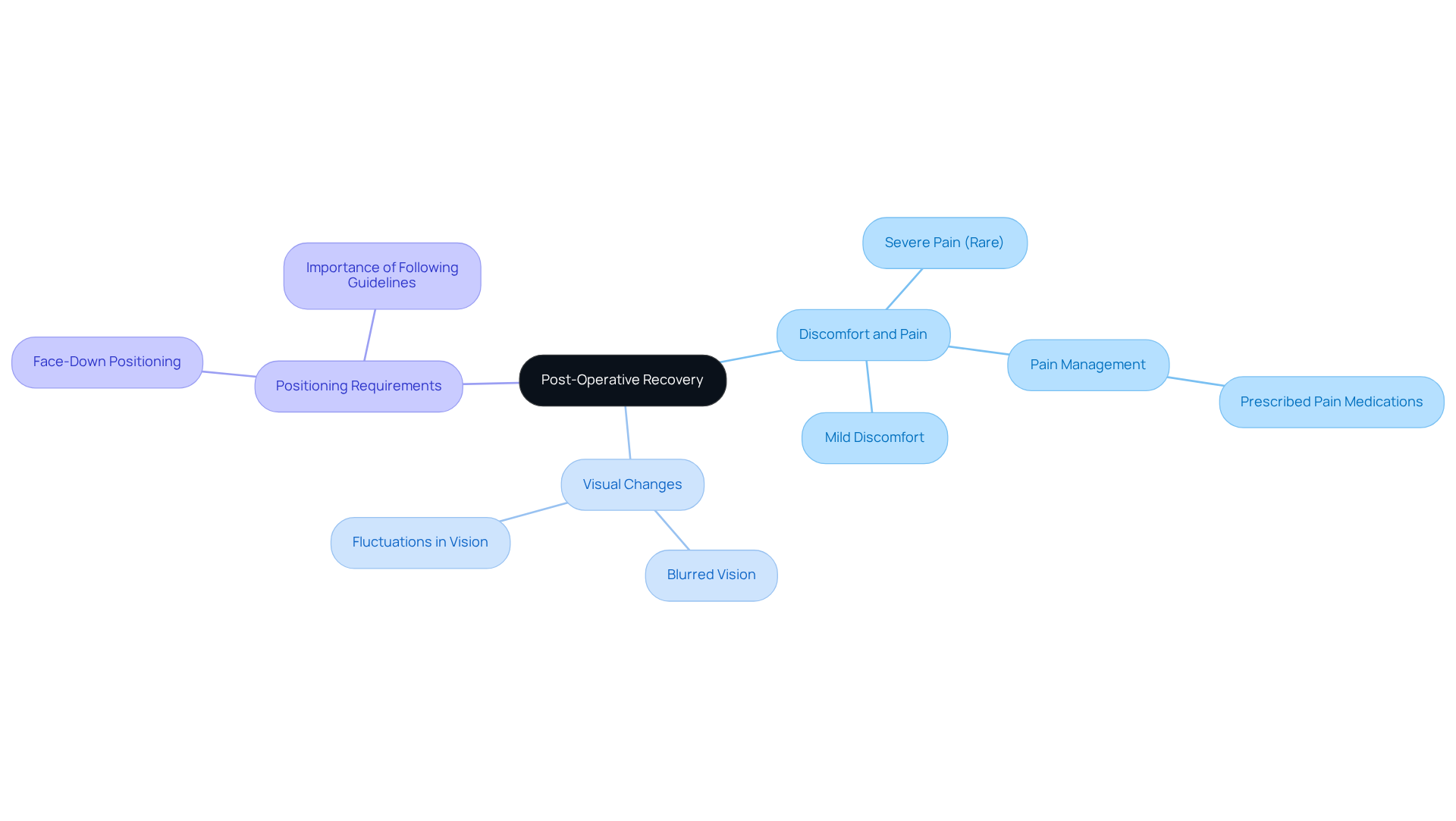
Long-term results before and after retinal detachment eye surgery can vary significantly from person to person. Factors such as the type of surgery, the timing of the intervention, and individual characteristics are all important before and after retinal detachment eye. We understand that this can be a concerning time, so let’s explore some key points together:
- Visual Acuity Improvement: Many patients notice substantial improvements in their vision within the first few months after surgery. Full recovery can take up to a year. Notably, those who undergo vitrectomy often report better long-term results compared to those treated with pneumatic retinopexy. For example, studies show that 93% of individuals with macula-on detachments achieved visual acuity suitable for UK driving standards after 10 years. In contrast, 65.2% of those with macula-off detachments reached similar standards. This highlights how the initial macular status before and after retinal detachment eye can impact recovery.
- Complications: It’s common to worry about complications like recurrent detachment and cataract formation, especially after vitrectomy. About 14% of individuals may experience redetachment within 10 years, which can lead to poorer visual outcomes. Understanding these risks is crucial for anyone considering surgery, especially before and after retinal detachment eye. It’s important to have timely discussions about potential future cataract surgery, as vitrectomy can speed up cataract formation.
- Quality of Life: Many patients report an improved quality of life after surgery, although some may still face challenges, such as reduced peripheral vision or difficulties with night vision. Patient testimonials often emphasize the importance of setting realistic expectations for healing. Visual function can continue to improve beyond the initial follow-up period. This underscores the need for ongoing monitoring and support to address any lingering issues and enhance results.
We are here to help you through this process, ensuring you feel supported every step of the way.
Managing Recovery: Challenges and Considerations Post-Surgery
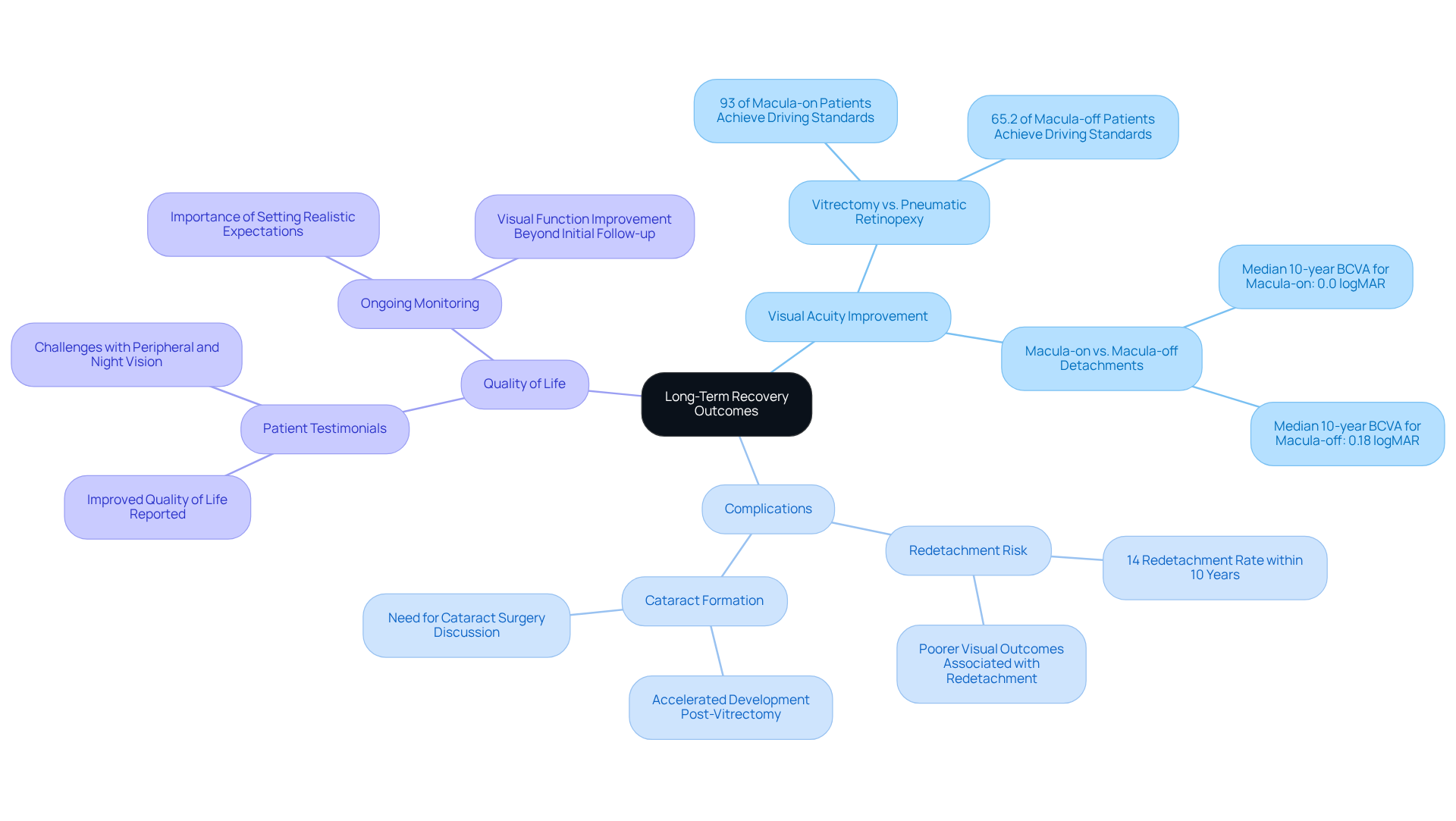
Healing from retinal detachment surgery can be a challenging journey, and it’s completely normal to feel a mix of emotions during this time. Here are some key aspects to consider that can help you navigate your recovery:
- Adherence to Positioning: We understand that maintaining the required head position is crucial for your recovery, but it can also be uncomfortable and inconvenient. Did you know that adherence rates after macular hole surgery can be as high as 90.8%? Using specialized pillows or furniture can make it easier for you to stick to your prescribed positioning, especially during those critical postoperative days when recommendations may vary.
- Emotional Well-being: The healing process can be emotionally taxing, particularly if you find that your vision improvement is slower than you hoped. Quality of life ratings for individuals following face-down positioning (FDP) average 89.3, which underscores the importance of emotional support during this time. Connecting with support groups or seeking counseling can provide essential comfort for anyone feeling anxious or down during their recovery.
- Follow-Up Care: Regular follow-up appointments are vital for monitoring your progress and catching any complications early. Typically, the advised head positioning lasts around 9.6 days, so it’s important to prioritize these appointments. Keep an open line of communication with your healthcare providers about any concerns that arise.
By proactively addressing these challenges, you can enhance your recovery experience and improve your overall outcomes. Remember, we are here to help you through this process, paving the way for a smoother transition back to your daily life.
Conclusion
Experiencing retinal detachment and undergoing surgery can feel overwhelming. We understand that knowing what to expect during recovery is crucial for regaining your vision and enhancing your quality of life. This article highlights the importance of being informed about the recovery process, the various surgical options available, and the significance of post-operative care.
There are different surgical methods, such as:
- Scleral buckling
- Vitrectomy
- Pneumatic retinopexy
Each comes with its own benefits and risks. The initial recovery phase may bring challenges like discomfort, visual changes, and specific positioning requirements. These factors are vital for optimal healing. Many patients report improved visual acuity and a better quality of life in the long run, although some may encounter complications that require ongoing support and monitoring.
Navigating the recovery journey from retinal detachment surgery requires patience and adherence to medical advice. It’s common to feel uncertain during this time, but emotional support can make a significant difference. Engaging with healthcare providers and support networks can enhance your recovery experience. By staying informed and proactive, you can better manage your recovery and pave the way for a successful return to everyday life.
Frequently Asked Questions
What is retinal detachment?
Retinal detachment occurs when the light-sensitive membrane at the back of the eye separates from the supportive tissue beneath it. If not treated promptly, it can lead to permanent vision loss.
What are the symptoms of retinal detachment?
The article does not specify symptoms, but common symptoms may include sudden flashes of light, floaters, or a shadow over the visual field.
What are the surgical options available for repairing a detached retina?
There are several surgical options, including Scleral Buckling, Vitrectomy, and Pneumatic Retinopexy.
How does Scleral Buckling work?
Scleral Buckling involves placing a silicone band around the eye to gently push the wall of the eye against the light-sensitive tissue, helping it to reattach.
What is Vitrectomy?
Vitrectomy is a surgical procedure that involves removing the vitreous gel that may be pulling on the light-sensitive layer, allowing the retina to settle back into its proper position.
What is Pneumatic Retinopexy?
Pneumatic Retinopexy is a procedure where a gas bubble is injected into the eye to push the retina back into place, often followed by laser treatment to seal the retina securely.
Why is it important to discuss surgical options with an ophthalmic surgeon?
Each surgical method has its own benefits and risks, making it essential to have a thorough discussion with a qualified ophthalmic surgeon to determine the best approach for your individual situation.
What support is available for individuals experiencing retinal detachment?
The article emphasizes that individuals are not alone in this journey and that support is available throughout the process.
List of Sources
- Understanding Retinal Detachment and Surgical Options
- Pediatric Retinal Detachments (https://aao.org/education/disease-review/pediatric-retinal-detachments)
- Retinal Detachment: Improving Outcomes with Technique and Technology – Advances for Medical Professionals | NewYork-Presbyterian (https://nyp.org/publications/professional-advances/ophthalmology/retinal-detachment-improving-outcomes-with-technique-and-technology)
- The Scottish RD survey 10 years on: the increasing incidence of retinal detachments – Eye (https://nature.com/articles/s41433-022-02123-1)
- Primary retinal detachment: A review of the development of techniques for repair in the past 80 years – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5525625)
- Post-Operative Recovery: Initial Experiences After Surgery
- Patient Stories
- Patients – The American Society of Retina Specialists (https://asrs.org/patients/patient-stories)
- 1-year outcomes after retinal detachment surgery among Medicare beneficiaries – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC2926163)
- Retinal Detachment Surgery Recovery Timeline (https://everett-hurite.com/blog/how-long-does-recovery-take-after-retinal-detachment-surgery-in-pittsburgh-pa)
- One Year Outcomes After Retinal Detachment Surgery (https://academia.edu/124386346/One_Year_Outcomes_After_Retinal_Detachment_Surgery)
- Retina Surgery Outcomes | Mass Eye and Ear (https://masseyeandear.org/ophthalmology-outcomes/retina-surgery)
- Long-Term Recovery Outcomes: Comparing Patient Experiences
- Early Post Retinal Detachment Surgery Acuity Predicts Long-Term Visual Outcomes (https://ophthalmologyadvisor.com/news/early-acuity-predicts-long-term-visual-outcomes-after-retinal-detachment-repair)
- Long-term Detachment Outcomes Studied (https://reviewofophthalmology.com/article/longterm-detachment-outcomes-studied)
- The Scottish Retinal Detachment Study: 10-year outcomes after retinal detachment repair – Eye (https://nature.com/articles/s41433-025-03613-8)
- 10-Year RRD Repair Outcomes Look Good, Study Finds (https://reviewofoptometry.com/article/10year-rrd-repair-outcomes-look-good-study-finds)
- Managing Recovery: Challenges and Considerations Post-Surgery
- Post-Surgery Recovery Wishes: 80 Message Ideas (https://bloomsybox.com/blog/posts/surgery-encouraging-message-ideas)
- Adherence to the face-down positioning after vitrectomy and gas tamponade: a time series analysis – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5819221)
- Head Positioning after RD Surgery: A Review – Retina Today (https://retinatoday.com/articles/2024-oct/head-positioning-after-rd-surgery-a-review)
- 110 Get well soon wishes after surgery: quotes, Funny & images for friend – Rise Blessings (https://riseblessings.com/get-well-soon-wishes-after-surgery)
- 38 Best Wishes for After Surgery: Message Ideas for a Good Recovery (https://spoonfulofcomfort.com/blog/38-best-wishes-for-surgery-message-ideas-for-a-good-recovery?srsltid=AfmBOorxdn-dp4a-ZwdmTkc8oB0-DFfVxuuJFssN1v-OlyLRPmsfZCD2)






