Posted by: Northwest Eye in Eye Symptoms and Their Causes on March 16, 2026
Introduction
Eye health is a crucial part of our overall well-being, and it’s understandable to feel uncertain about the possibilities that eye transplants can offer. With the remarkable advancements in medical technology, procedures like corneal transplants have the potential to restore vision for thousands each year. However, the complexities surrounding eye transplants can often lead to confusion and concern.
We understand that considering such life-changing surgeries can be daunting. What challenges might you face, and how can you navigate the intricate landscape of options available? It’s common to feel overwhelmed, but understanding the potential benefits and limitations of eye transplants is essential for anyone seeking clarity on this vital topic.
We are here to help you through this process, providing the support and information you need to make informed decisions about your eye health.
Define Eye Transplants and Transplantable Tissues
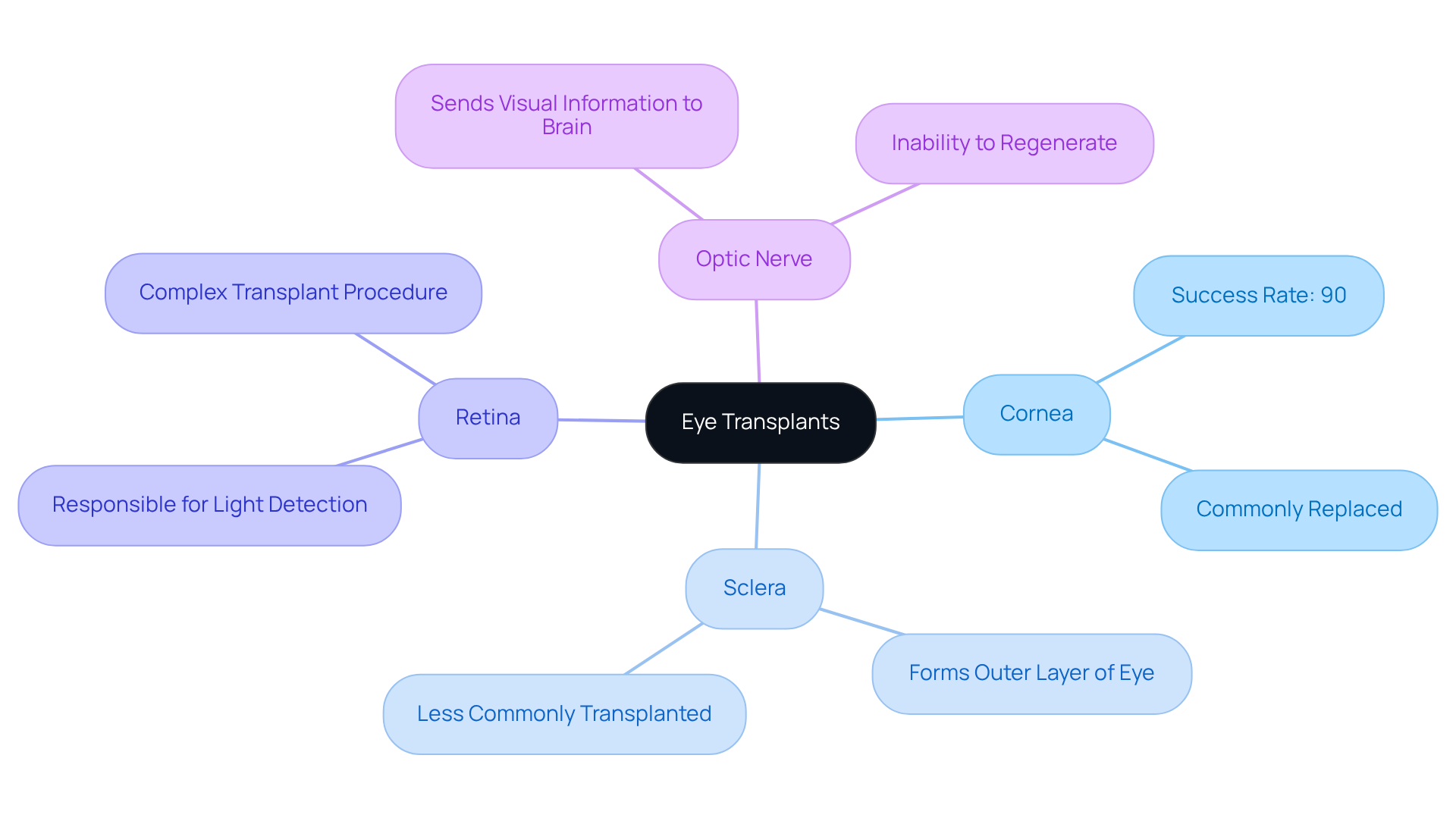
Eye transplants encompass surgical procedures designed to replace damaged or diseased eye tissues, aiming to restore vision. The cornea, the clear front part of the eye, is the most commonly replaced component, with over 85,000 corneal transplants performed each year in the United States alone. Other transplantable materials include:
- The sclera, which forms the outer layer of the eye
- The retina, responsible for detecting light
- The optic nerve, which sends visual information to the brain
It’s common to feel concerned about the success of these surgeries. Corneal transplants have a success rate of over 90% in low-risk situations, which is reassuring. However, procedures involving the sclera, retina, and optic nerve are less frequent and can be more complex. A significant challenge in restoring vision is the optic nerve’s inability to regenerate, given the complexities involved.
Moreover, the COVID-19 pandemic has greatly affected the availability of corneal tissue, leading to a notable decline in tissue distribution. We recognize that understanding these challenges is crucial for patients exploring their options for vision restoration. As advancements in surgical techniques and regenerative medicine continue to evolve, we are here to help you through this process, providing support and guidance every step of the way.
Explore Types of Eye Transplants: Corneal and Beyond
Eye transplants can be categorized into several types, each serving distinct purposes and addressing specific conditions. We understand that considering these options can feel overwhelming, but we’re here to help you through this process.
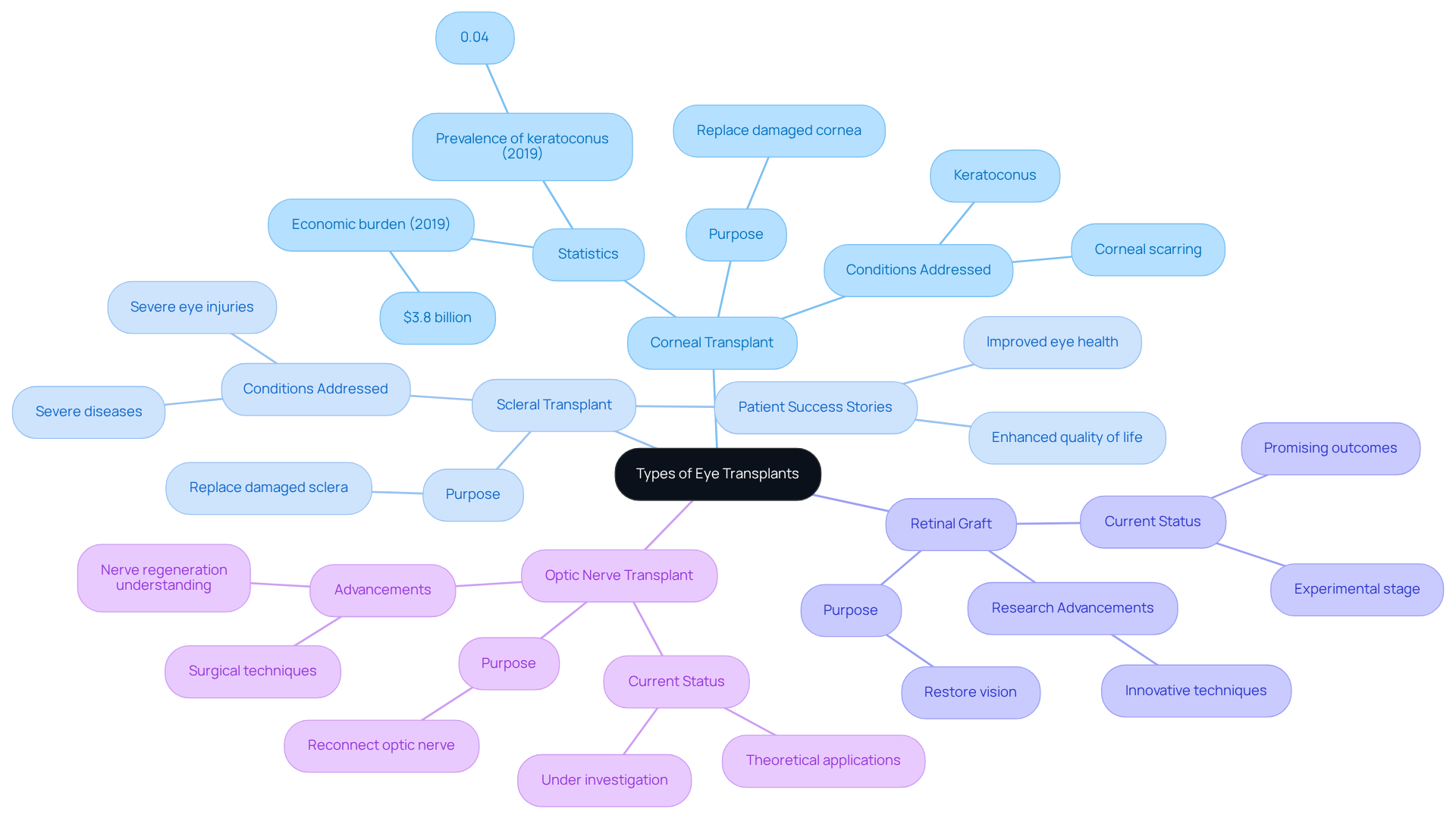
- Corneal Transplant: This is the most prevalent type, where a damaged cornea is replaced with healthy donor tissue. It’s often performed to address issues like keratoconus and corneal scarring, significantly enhancing visual acuity for many individuals. In fact, recent data shows that the national prevalence of keratoconus was 0.04% in 2019, highlighting the importance of this procedure for those affected.
- Scleral Transplant: This procedure involves replacing the sclera, the white outer layer of the eyeball, to address severe eye injuries or diseases. Scleral grafts can be vital for individuals with significant damage, providing an opportunity for improved eye health and function. Many patients have shared their success stories after undergoing scleral procedures, illustrating the potential for significant recovery and enhanced quality of life.
- Retinal Transplant: Currently in the experimental stage, retinal transplants aim to restore vision by replacing damaged retinal tissue. Recent advancements in research are exploring innovative techniques to improve the success rates of these procedures. Ongoing studies indicate promising outcomes, and experts like Lynda Seminara emphasize the need for continued research to enhance treatment options for retinal damage.
- Optic Nerve Transplant: Also under investigation, this procedure seeks to reconnect the optic nerve to restore vision in cases of severe damage. While still largely theoretical, advancements in surgical techniques and our understanding of nerve regeneration are paving the way for future applications.
Comprehending these types of eye procedures is essential for you to engage in informed discussions with your healthcare providers about potential options and outcomes. Remember, we’re here to support you every step of the way.
Understand Challenges and Limitations of Eye Transplants
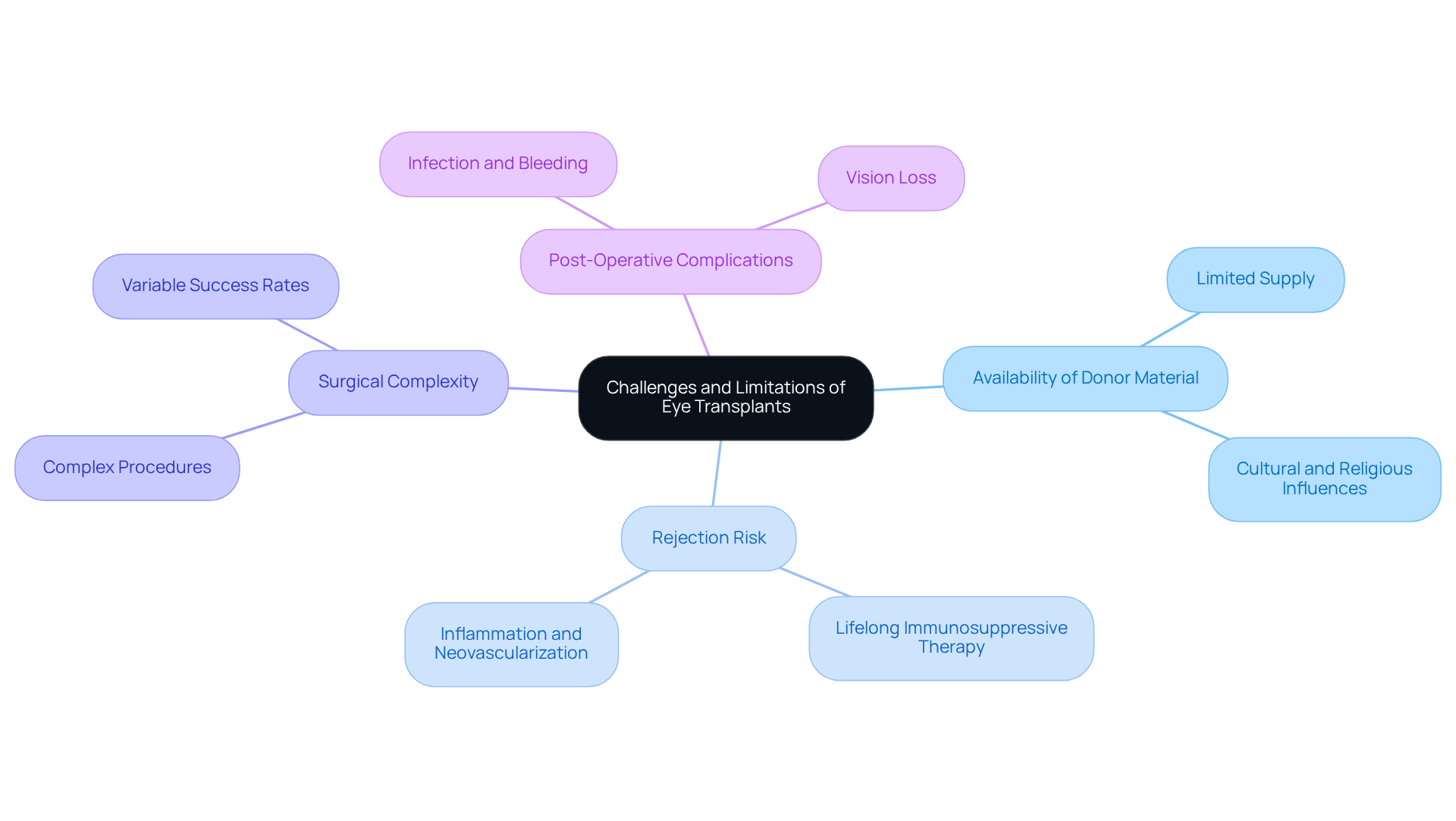
s hold great promise, but they also come with several challenges and limitations that we want you to be aware of:
- make informed decisions about your care We understand that the limited supply of suitable donor materials can be frustrating and may delay procedures.
- lifelong immunosuppressive therapy It’s important to know that the body may reject transplanted tissues, which means treatment might be necessary.
- Availability of Donor Material Procedures like retinal and optic nerve grafts are highly complex and still experimental, with success rates that can vary.
- Post-Operative Complications After surgery, patients may face complications such as infection, bleeding, or even vision loss. We recognize that support is essential for anyone contemplating eye procedures.
We are here to help you through this process, and it’s common to feel a mix of hope and concern. Understanding these challenges can empower you to navigate surgical complexity.
Navigate Post-Operative Care and Recovery After Transplant
Post-operative care is vital for the success of an eye transplant. We understand that this can be a challenging time, but adhering to these key steps can significantly enhance your recovery outcomes:
- Follow-Up Appointments: Please attend all scheduled follow-ups with your ophthalmologist. These appointments are crucial for monitoring your healing and identifying any complications early. Research shows that individuals who consistently attend follow-up visits experience better visual outcomes and lower rates of complications.
- Medication Compliance: It’s essential to take your prescribed medications, including anti-rejection drugs and antibiotics, exactly as directed. Studies indicate that medication adherence among eye transplant recipients greatly affects recovery success, with non-compliance linked to negative outcomes. We recognize that logistical challenges, like access to safe drinking water, can hinder adherence, so it’s important to seek support in managing these barriers.
- Protective Measures: Wearing an eye shield or glasses as recommended is important to protect your eye from injury and infection during the healing process.
- Activity Restrictions: Avoid strenuous activities and heavy lifting for a specified period to facilitate proper healing. Participating in high-impact activities too soon can jeopardize the success of your procedure.
- Monitor Symptoms: Be vigilant for signs of complications, such as increased redness, pain, or changes in vision. Reporting these symptoms to your doctor promptly can lead to timely interventions, improving your recovery prospects.
We also recognize that psychological and emotional stressors, including anxiety and paranoia, can impact adherence to post-operative care. Understanding these factors is vital for providing thorough support to you. By following these guidelines and addressing both logistical and emotional challenges, you can enhance your recovery experience and improve the likelihood of a successful outcome. Remember, we are here to help you through this process.
Conclusion
Exploring the realm of eye transplants can feel overwhelming, and it’s completely normal to have concerns. The idea of restoring vision through surgical procedures might seem daunting, but understanding the different types of eye transplants available – like corneal, scleral, retinal, and optic nerve transplants – can empower you to make informed decisions about your vision restoration options. The success rates associated with these procedures, especially corneal transplants, offer hope. However, it’s essential to recognize the limitations and risks involved.
Key insights from this exploration highlight the importance of:
- Donor material availability
- The potential for rejection
- The complexities of post-operative care
We understand that patients must be proactive in their recovery, adhering to follow-up appointments and medication regimens to maximize their outcomes. By navigating these challenges with the right support and knowledge, you can enhance your prospects for a successful recovery and improved quality of life.
Ultimately, the journey toward vision restoration through eye transplants is not just about the procedures themselves but also about understanding the broader implications of eye health and the ongoing advancements in medical science. As research progresses and new techniques emerge, staying informed and engaged in discussions with your healthcare provider is crucial. Embracing the possibilities while being aware of the challenges can lead to a more empowered and hopeful outlook for those considering eye transplant options. Remember, we are here to help you through this process.
Frequently Asked Questions
What are eye transplants and what tissues can be transplanted?
Eye transplants refer to surgeries that replace damaged or unhealthy parts of the eye. The most commonly replaced component is the cornea, but other transplantable tissues include the sclera, retina, and optic nerve.
How many corneal transplants are performed annually in the United States?
Over 85,000 corneal transplants are performed each year in the United States.
What is the success rate of corneal transplants?
Corneal transplants have a success rate of over 90% in low-risk situations.
Are there other types of eye transplants besides corneal transplants?
Yes, other types of eye transplants include procedures involving the sclera, retina, and optic nerve, although these are less frequent and more complex.
What is a significant challenge in restoring vision through eye transplants?
A significant challenge is the optic nerve’s inability to regenerate, which complicates efforts to restore vision.
How has the COVID-19 pandemic affected eye transplants?
The COVID-19 pandemic has greatly affected the availability of corneal tissue, leading to a notable decline in tissue distribution.
What support is available for patients considering eye transplants?
Patients can receive support and guidance throughout the process as advancements in surgical techniques and regenerative medicine continue to evolve.
List of Sources
- Define Eye Transplants and Transplantable Tissues
- Vision-restoring whole eye transplants may soon be a reality (https://med.stanford.edu/ophthalmology/news-and-media/news-archive/2024-stories/vision-restoring-whole-eye-transplants-may-soon-be-a-reality.html)
- Whole-eye transplantation: Current challenges and future perspectives – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11212585)
- Future of Corneal Donation and Transplantation: Insights From COVID-19 Pandemic – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC7473794)
- Organ, Eye and Tissue Donation Statistics (https://donatelife.net/donation/statistics)
- Eyes on the Prize: Easing the Burden on Corneal Transplant Patients | Medical College of Virginia Foundation (https://mcvfoundation.org/news/stories/eyes-prize-easing-burden-corneal-transplant-patients)
- Explore Types of Eye Transplants: Corneal and Beyond
- Keratoconus: An updated review (https://sciencedirect.com/science/article/pii/S1367048421002058)
- Prevalence and Economic Burden of Keratoconus in the United States – PubMed (https://pubmed.ncbi.nlm.nih.gov/37951332)
- Keratoconus: U.S. Prevalence and Economic Burden (https://aao.org/eyenet/article/keratoconus-prevalence-economic-burden)
- Corneal Transplantation Outcomes at a Teaching Hospital: Residents vs Experts (https://gavinpublishers.com/article/view/corneal-transplantation-outcomes-at-a-teaching-hospital-residents-vs-experts)
- Understand Challenges and Limitations of Eye Transplants
- Statistical Report – EBAA (https://restoresight.org/members/publications/statistical-report)
- Global Survey of Corneal Transplantation and Eye Banking (https://jamanetwork.com/journals/jamaophthalmology/fullarticle/2474372)
- Long-term outcomes of corneal transplantation: a review of 8,378 patients – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11756154)
- High-risk Corneal Transplantation: Recent Developments and… : Transplantation (https://journals.lww.com/transplantjournal/fulltext/2019/12000/high_risk_corneal_transplantation__recent.9.aspx)
- 2024 Eye Banking Statistical Report—Executive Summary : Eye Banking and Corneal Transplantation (https://journals.lww.com/ebctjournal/fulltext/2025/06000/2024_eye_banking_statistical_report_executive.5.aspx)
- Navigate Post-Operative Care and Recovery After Transplant
- Lost-to-follow-up: A study on corneal transplantation from Eastern India – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10391456)
- Predictors and associated outcomes of adherence to treatment in Russian patients undergoing corneal transplantation | Russian Open Medical Journal (https://romj.org/2024-0205)
- Factors Impacting the Medication “Adherence Landscape” for Transplant Patients – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10272095)
- Medication Adherence Among Patients with Corneal Diseases – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8418623)
- Treatment adherence after penetrating corneal transplant in a New Zealand population from 2000 to 2009 – PubMed (https://pubmed.ncbi.nlm.nih.gov/25393095)






