Posted by: Northwest Eye in General on April 9, 2026
Introduction
Keratoconus is a progressive eye condition that affects millions of people, and we understand how daunting it can be. If left untreated, it can lead to significant vision impairment. But there’s hope. This article explores keratoconus cross-linking, a minimally invasive procedure that not only halts the disease’s progression but also offers a chance for improved visual stability.
Many patients face the overwhelming prospect of corneal transplants, and it’s common to feel anxious about what that means for your eye health and quality of life. How can cross-linking change this trajectory? Let’s delve into the details together, so you can feel more informed and empowered about your options.
Define Keratoconus: Understanding the Condition
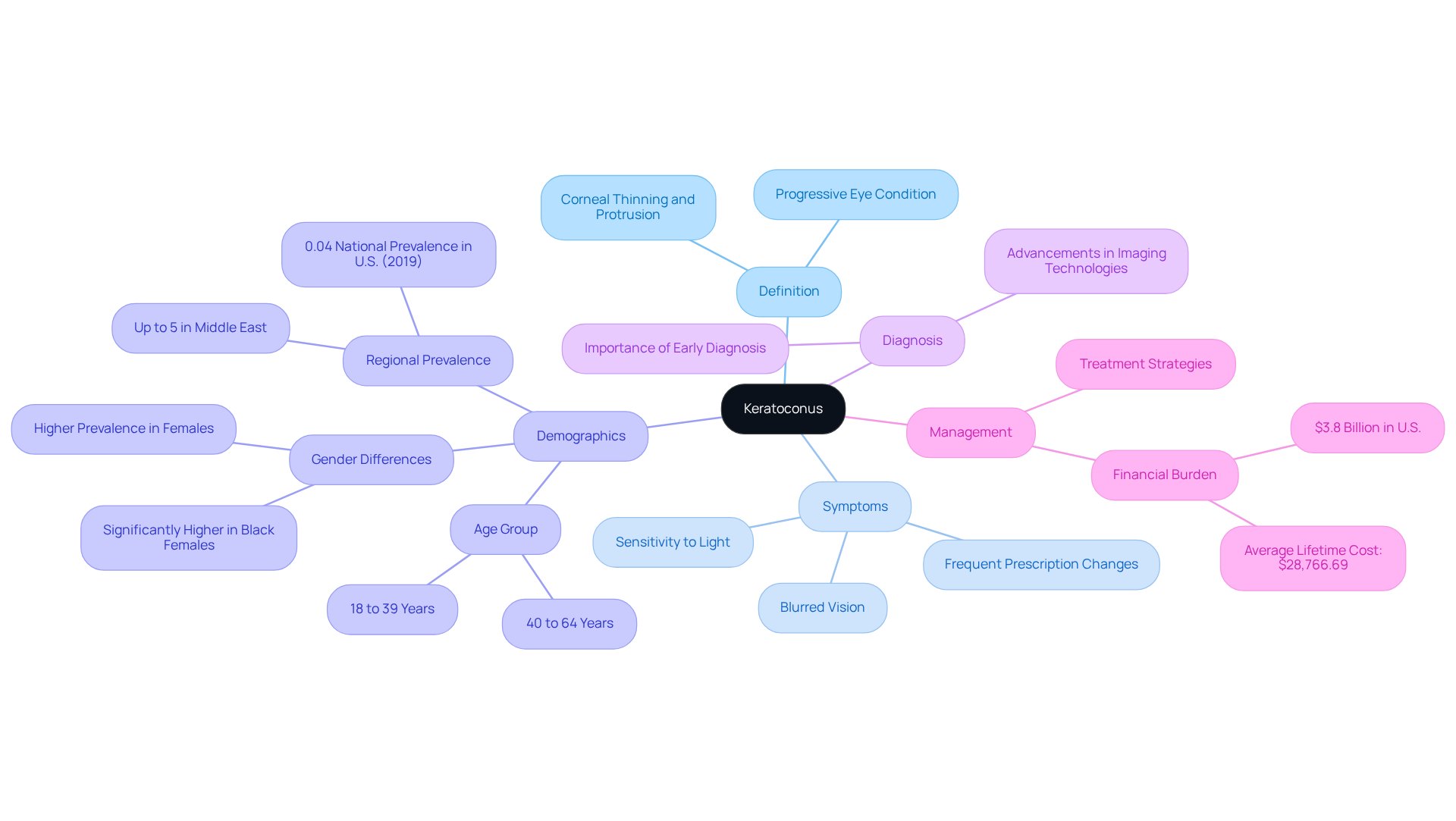
Keratoconus is a progressive eye condition that can be concerning. It’s characterized by the thinning and protrusion of the cornea, which leads to a cone-like shape that distorts your vision. This abnormal curvature can cause significant visual impairment, including blurred vision and increased sensitivity to light and glare. Many people first notice symptoms during their teenage years or early adulthood, often resulting in frequent changes in eyeglass prescriptions.
We understand that comprehending this eye condition is essential for effective management. Early diagnosis can significantly impact care outcomes and your overall quality of life. In certain regions, particularly in the Middle East, keratoconus affects up to 5% of the population. It’s been observed that young adults aged 18 to 39 years are particularly at risk. Notably, demographic studies indicate that Black females experience higher rates of this condition compared to their male counterparts, highlighting the need for targeted awareness and early intervention.
Recent advancements in imaging technologies have made it possible to diagnose keratoconus earlier, which is crucial for prompt care. Managing this eye condition can be financially burdensome, with the total strain in the U.S. approaching around $3.8 billion. This underscores its impact on both patients and the healthcare system. Eye care experts at Northwest Eye emphasize that identifying signs of corneal disease early, such as unclear sight, can lead to better management approaches and improved patient outcomes.
It’s also important to recognize that blurred vision can stem from other conditions like nearsightedness, farsightedness, and cataracts. Each of these may require different management strategies. Remember, we are here to help you through this process, and seeking care early can make a significant difference.
Explain Corneal Cross-Linking: The Treatment Process
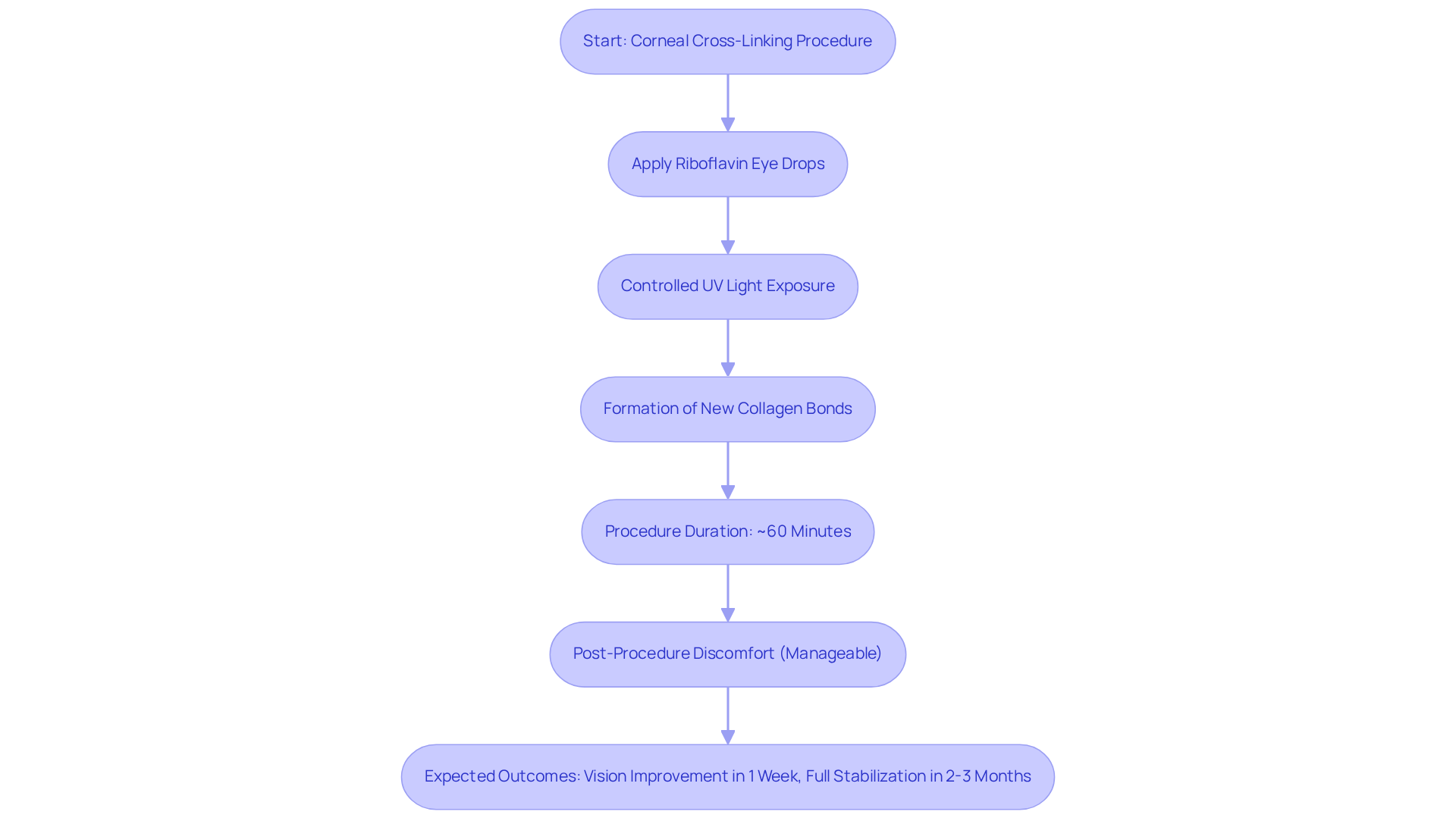
Keratoconus crosslinking is a minimally invasive procedure designed to strengthen the cornea and stop the progression of keratoconus. We understand that facing such a condition can be daunting, but this treatment offers hope. It starts with riboflavin (vitamin B2) eye drops applied to the cornea, followed by controlled exposure to ultraviolet (UV) light. This combination helps form new collagen bonds within the cornea, significantly enhancing its structural integrity.
Typically, the procedure lasts about 60 minutes and is performed under topical anesthesia, ensuring your comfort throughout. While some discomfort may occur during and after the procedure, most patients find it manageable. Many individuals report noticeable improvements in their vision within the first week, although full stabilization may take two to three months.
The success rate of keratoconus crosslinking is impressive, with over 90 percent of treated eyes showing halted progression of the condition. This underscores its importance as a treatment option. We encourage you to seek a prompt referral to a corneal specialist for the best outcomes, especially before the cornea becomes too thin. Remember, you’re not alone in this journey; we are here to help you through the process.
Highlight Benefits: Why Choose Cross-Linking for Keratoconus
Keratoconus crosslinking (CXL) provides several key benefits for individuals experiencing corneal ectasia. We understand that dealing with this condition can be challenging, and it’s common to feel concerned about your vision. Keratoconus crosslinking (CXL) effectively slows or even halts the progression of the disease, helping to prevent further deterioration of your sight.
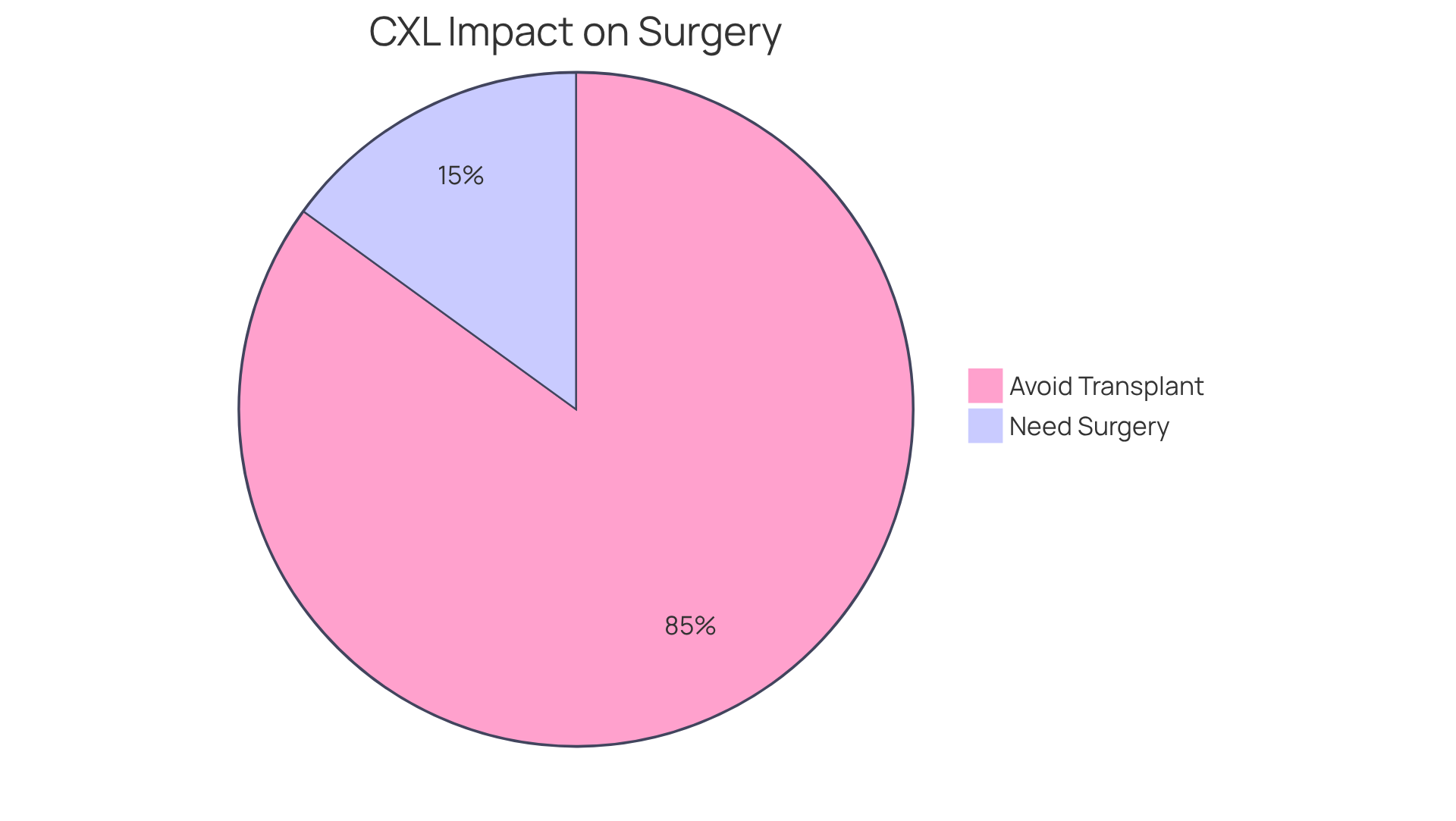
Recent studies show that around 80% to 90% of individuals with keratoconus can successfully avoid corneal transplants thanks to keratoconus crosslinking, who were once considered candidates for surgery. Many patients share their relief and joy at experiencing improved stability in their vision after the procedure, which significantly enhances their quality of life.
By reinforcing the cornea’s structure, CXL reduces the need for more invasive treatments, such as corneal transplants. This minimally invasive procedure, keratoconus crosslinking, is not just a treatment; it’s a vital step in managing keratoconus and preserving your long-term eye health. We are here to help you through this process, ensuring you feel supported every step of the way.
Outline Post-Operative Care: Ensuring a Smooth Recovery
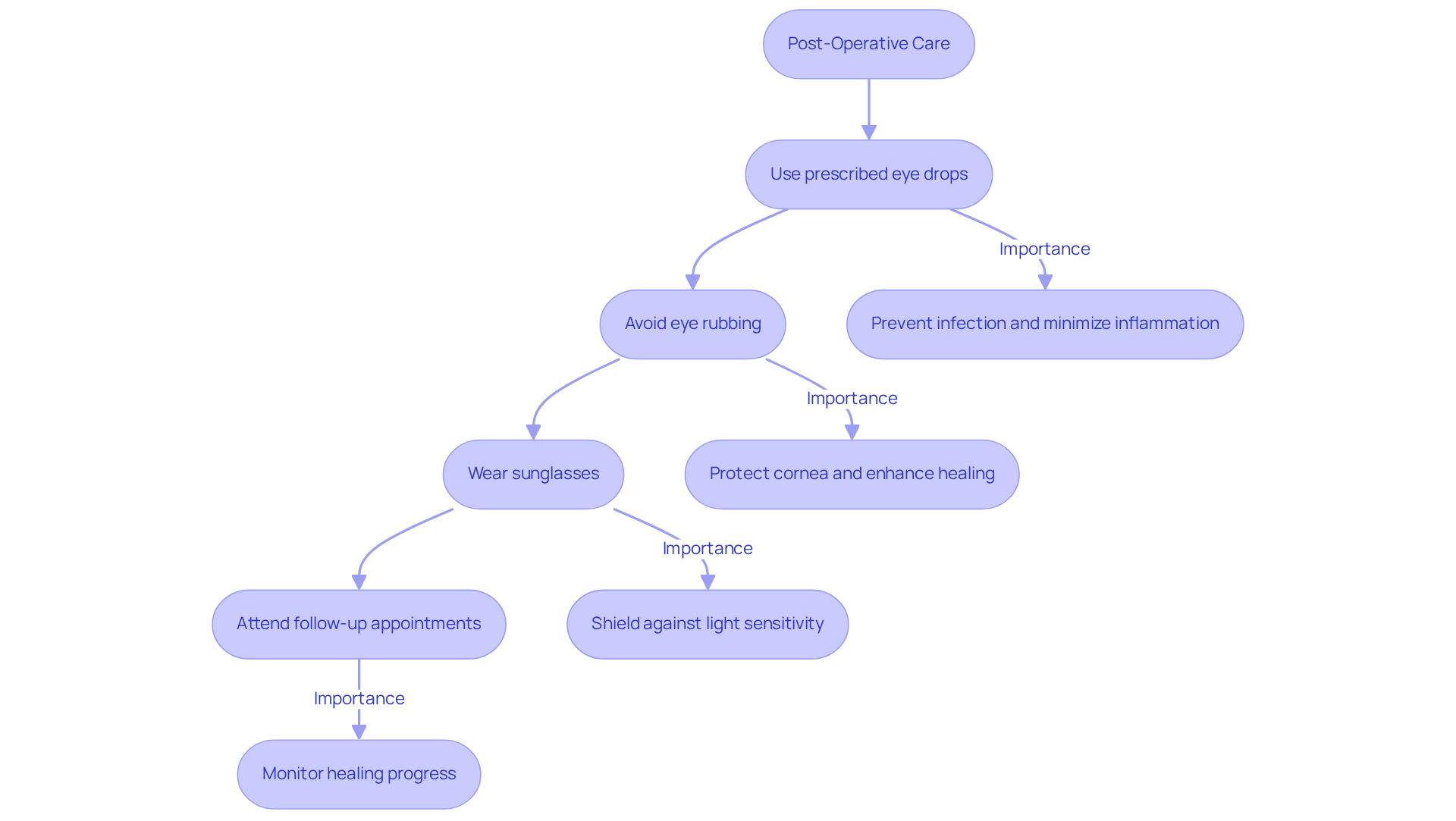
Post-operative care following corneal cross-linking is crucial for a smooth recovery. We understand that this can be a challenging time, and adhering to specific instructions can make all the difference. It’s important to use the prescribed antibiotic and anti-inflammatory eye drops to prevent infection and minimize inflammation. Avoiding eye rubbing is essential, and wearing sunglasses can help shield against light sensitivity, which many experience during the healing phase.
Follow-up appointments are vital for monitoring your healing progress and addressing any concerns that may arise. Most individuals can return to regular activities within a week, but complete visual stabilization typically takes around six months. During this time, it’s common for your sight to fluctuate; some may notice temporary blurriness or light halos. Many patients report that while initial discomfort eases within a few days, clearer vision often begins to emerge around the two to three-month mark.
We encourage you to adhere to your ophthalmologist’s recommendations and maintain regular follow-ups. This significantly enhances recovery outcomes and ensures that any complications are managed promptly. Remember, you’re not alone in this journey; we are here to help you through the process.
Conclusion
Keratoconus cross-linking shines as a beacon of hope for those facing this progressive eye condition. It effectively strengthens the cornea and halts vision deterioration, offering a crucial lifeline to those affected. We understand that early diagnosis and intervention are vital, playing a pivotal role in managing keratoconus and ensuring better outcomes for patients.
In this guide, we’ve shared key insights about keratoconus, its symptoms, and the importance of timely treatment. The corneal cross-linking procedure not only boasts impressive success rates but also significantly reduces the need for more invasive interventions, like corneal transplants. Post-operative care is equally important; following recovery protocols can enhance the likelihood of a smooth healing process and optimal visual stabilization.
Ultimately, raising awareness about keratoconus and its treatment options is essential for fostering better health outcomes. If you’re experiencing symptoms, we encourage you to seek prompt evaluation and care. Early intervention can lead to life-changing improvements in vision and quality of life. Embracing this proactive approach empowers you to take charge of your eye health and navigate your journey with confidence.
Frequently Asked Questions
What is keratoconus?
Keratoconus is a progressive eye condition characterized by the thinning and protrusion of the cornea, leading to a cone-like shape that distorts vision.
What are the symptoms of keratoconus?
Symptoms include blurred vision, increased sensitivity to light and glare, and frequent changes in eyeglass prescriptions.
At what age do people typically notice symptoms of keratoconus?
Many people first notice symptoms during their teenage years or early adulthood.
How prevalent is keratoconus in the population?
In certain regions, particularly in the Middle East, keratoconus affects up to 5% of the population, with young adults aged 18 to 39 years being particularly at risk.
Are there demographic differences in the prevalence of keratoconus?
Yes, demographic studies indicate that Black females experience higher rates of keratoconus compared to their male counterparts.
Why is early diagnosis of keratoconus important?
Early diagnosis can significantly impact care outcomes and improve overall quality of life.
How has technology improved the diagnosis of keratoconus?
Recent advancements in imaging technologies have made it possible to diagnose keratoconus earlier, which is crucial for prompt care.
What is the financial impact of keratoconus management in the U.S.?
The total financial strain of managing keratoconus in the U.S. approaches around $3.8 billion.
What should individuals with blurred vision consider?
Blurred vision can also stem from other conditions such as nearsightedness, farsightedness, and cataracts, each requiring different management strategies.
How can seeking care early affect keratoconus management?
Seeking care early can lead to better management approaches and improved patient outcomes.
List of Sources
- Define Keratoconus: Understanding the Condition
- Keratoconus: U.S. Prevalence and Economic Burden (https://aao.org/eyenet/article/keratoconus-prevalence-economic-burden)
- Prevalence and Economic Burden of Keratoconus in the United States | Department of Ophthalmology (https://eye.hms.harvard.edu/publications/prevalence-and-economic-burden-keratoconus-united-states)
- Keratoconus epidemiology: A review – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9375461)
- Prevalence of keratoconus estimated at more than 3% | 2 Minute Medicine (https://2minutemedicine.com/prevalence-of-keratoconus-estimated-at-more-than-3)
- Incidence and Prevalence of Keratoconus Rises Globally (https://reviewofoptometry.com/news/article/incidence-and-prevalence-of-keratoconus-rises-globally)
- Explain Corneal Cross-Linking: The Treatment Process
- What Is Corneal Cross-Linking and Is It Worth It? (https://my.clevelandclinic.org/health/procedures/corneal-cross-linking)
- How Many People Undergo Corneal Cross-Linking for Keratoconus? Treatment Statistics, Age Patterns, & Outcome Data | Glossary (https://lens.com/questions-answered/how-many-people-undergo-corneal-cross-linking-for-keratoconus?srsltid=AfmBOooPAxmGwhTPuyIWRqat4kWzfNH2vEtBC5ClWQJFxSw0qjmSV0oE)
- What is the success rate of corneal cross-linking? (https://oculase.com/treatments/keratoconus-treatment/answerpack/keratoconus/keratoconus-faqs/what-is-the-success-rate-of-corneal-cross-linking)
- Highlight Benefits: Why Choose Cross-Linking for Keratoconus
- Fewer Keratoplasties After CXL Adoption (https://aao.org/eyenet/article/fewer-keratoplasties-after-cxl-adoption)
- What Percentage of Keratoconus Patients Avoid Surgery Using Scleral Lenses? Progression Data, Visual Acuity, & Outcomes | Glossary (https://lens.com/questions-answered/keratoconus-surgery-avoidance-scleral-lenses?srsltid=AfmBOopx5HahAdEbmFykmBMjEo9Du3m6DcK_r1rXUOhxeiHEF15i4Xes)
- Understanding Keratoconus and the Benefits of Crosslinking (https://pacificeyemd.com/understanding-keratoconus-and-the-benefits-of-crosslinking-blog)
- Long-Term Outcomes in Crosslinking Therapy for Patients with Progressive Keratoconus (https://mdpi.com/2075-4418/15/5/626)
- The impact of cross-linking on corneal transplant rates | Ophthalmology Times – Clinical Insights for Eye Specialists (https://ophthalmologytimes.com/view/the-impact-of-cross-linking-on-corneal-transplant-rates)
- Outline Post-Operative Care: Ensuring a Smooth Recovery
- Evaluation of a Post-Operative Therapy Protocol after Epithelium-Off Corneal Cross-Linking in Patients Affected by Keratoconus – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9738184)
- Cross-linking Post-op Instructions | Palm Desert (https://modernicareoptometry.com/blog/post-op-instructions.html)
- Long-Term Outcomes in Crosslinking Therapy for Patients with Progressive Keratoconus (https://mdpi.com/2075-4418/15/5/626)
- How Long Does It Take for Corneal Cross-Linking to Heal? (https://eyecliniclondon.com/blog/corneal-crosslinking-healing-time)
- Rate of Corneal Collagen Crosslinking Redo in Private Practice: Risk Factors and Safety – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC4383466)






