Posted by: Northwest Eye in Eye Symptoms and Their Causes on April 26, 2026
Introduction
We understand that dealing with eye health issues can be overwhelming, especially when it comes to conditions like ocular cellulitis. Ocular cellulitis can show up in two ways:
- Orbital cellulitis, which can seriously affect your vision,
- Periorbital cellulitis, which, while less severe, still needs quick medical care.
It’s important to recognize the symptoms and know your treatment options for ocular cellulitis, as ignoring it can lead to complications. So, how can you tell the difference between these two types and make sure you get the care you need when you need it?
Define Ocular Cellulitis: Orbital vs. Periorbital
We understand that dealing with ocular cellulitis can be concerning, especially regarding your vision and overall eye health. Ocular inflammation involves swelling and irritation of the tissues around your eye, and it can be categorized into two main types:
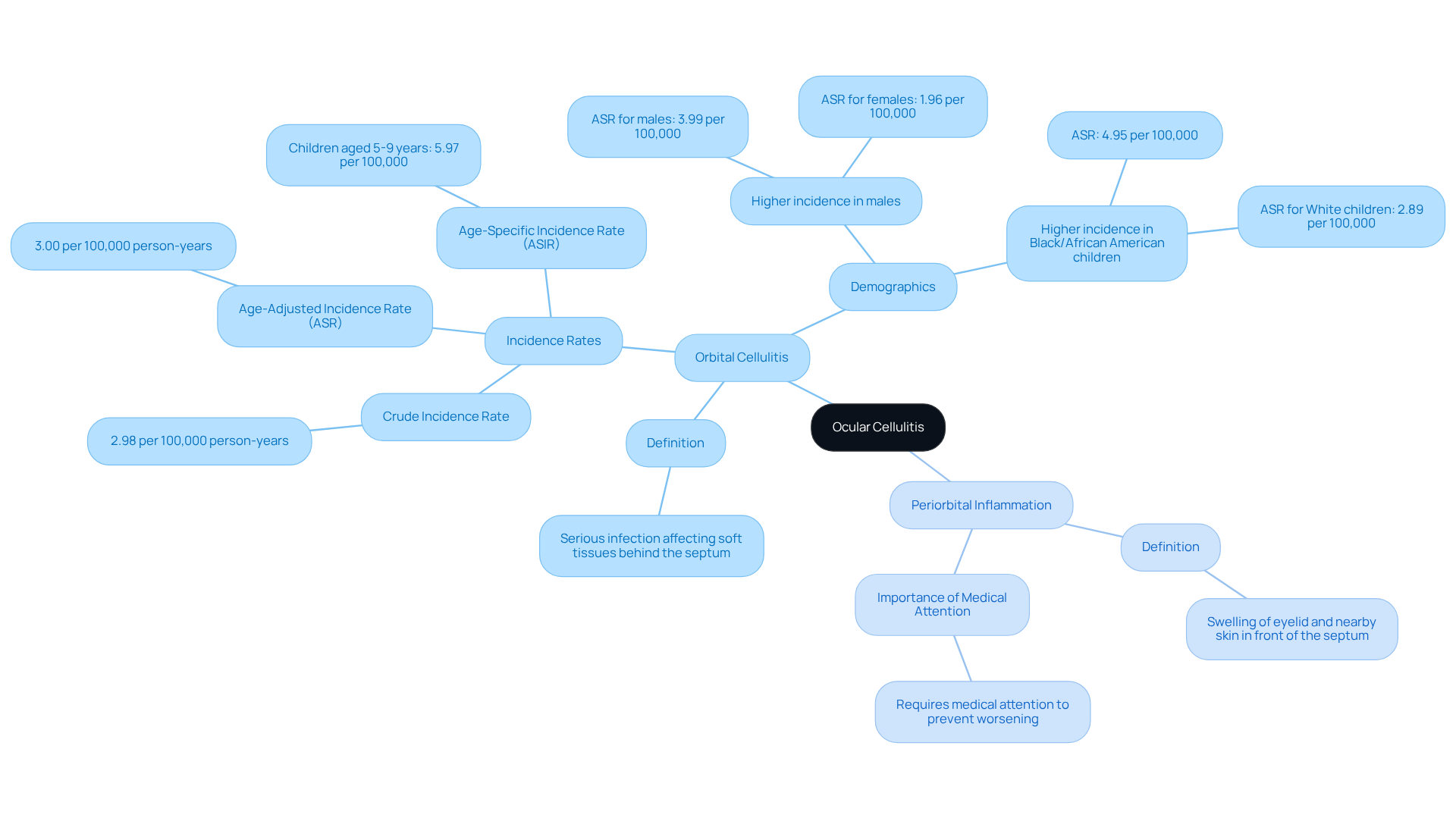
- Ocular cellulitis is a serious infection that affects the soft tissues behind the septum, which separates the eyelid from the deeper structures of the eye socket. If not treated promptly, it can lead to severe complications, including vision loss. It’s important to note that the age-adjusted incidence rate (ASR) of eye socket infections is approximately 3.00 per 100,000 person-years, with a crude incidence rate of 2.98 per 100,000 person-years. Children aged 5-9 years are particularly vulnerable, exhibiting the highest age-specific incidence rate (ASIR) of 5.97 per 100,000.
- Periorbital Inflammation: Also known as preseptal inflammation, this condition involves swelling of the eyelid and nearby skin in front of the septum separating the eye socket. While ocular cellulitis is typically less serious than an eye socket infection, it still requires medical attention to prevent worsening.
It’s common to feel overwhelmed by these distinctions, but understanding them is crucial for seeking the right care. Recent studies indicate that males are affected by eye socket infections nearly twice as often as females, with an ASR of 3.99 per 100,000 for males compared to 1.96 per 100,000 for females. Additionally, the occurrence of orbital inflammation is significantly higher in Black/African American children compared to their White peers, with rates of 4.95 per 100,000 against 2.89 per 100,000, respectively. Recognizing these demographic differences is crucial for effective diagnosis and treatment. By understanding these distinctions, you can take proactive steps towards seeking the right care for your eyes.
Identify Symptoms of Ocular Cellulitis
We understand that noticing symptoms of ocular cellulitis can be concerning, and it’s important to recognize them early for the best possible care. Common symptoms include:
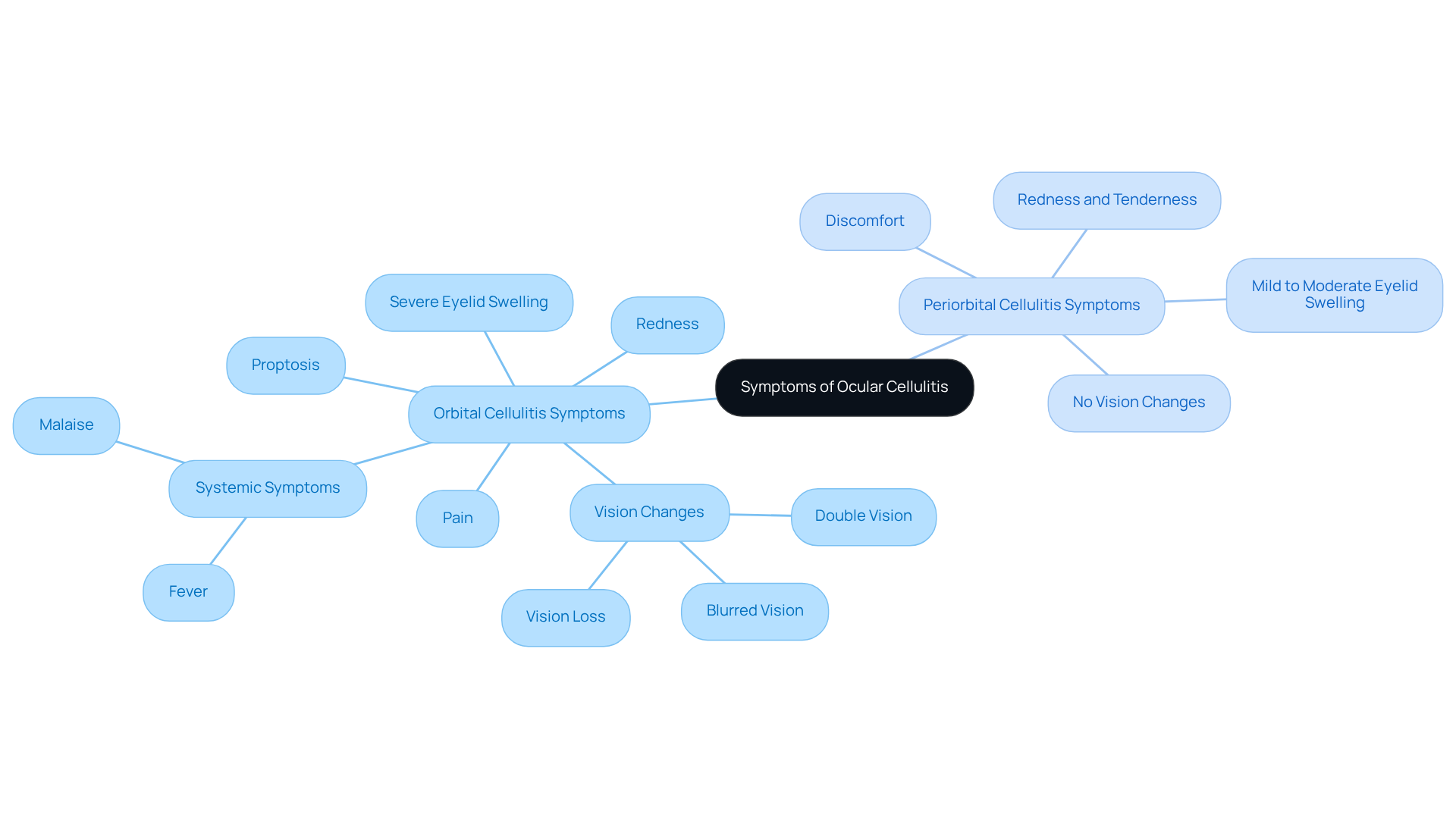
Orbital Cellulitis Symptoms:
- Severe eyelid swelling: Often unilateral, with significant edema.
- Redness: Noticeable erythema around the eye.
- Pain: Intense pain, especially with eye movement.
- Proptosis: Bulging of the eye due to swelling.
- Vision changes: Blurred or double vision, which can also indicate other serious conditions such as cataracts or diabetic retinopathy, frequently treated at Northwest Eye. In severe cases, vision loss may occur.
- Systemic symptoms: Fever and malaise may be present.
Periorbital Cellulitis Symptoms:
- Mild to moderate eyelid swelling: Less severe than orbital cellulitis.
- Redness and tenderness: Localized to the eyelid and surrounding skin.
- Discomfort: Generally less severe than in eye infections.
- No vision changes: Visual acuity is typically preserved.
Recognizing the symptoms of ocular cellulitis quickly can help you feel more in control and lead to timely medical intervention, reducing the risk of complications. Significantly, eye socket infection can result in severe complications, including loss of vision, which may happen in up to 11% of instances, even with treatment. The occurrence of orbital infection is significantly greater in children, especially those between 7 to 12 years old, emphasizing the necessity for attentiveness among caregivers and healthcare professionals. If you are experiencing any of these symptoms, taking action now can help ensure your vision remains protected and your health is prioritized.
Explore Causes of Ocular Cellulitis
We understand that learning about ocular cellulitis can feel overwhelming, particularly when taking its potential complications into account. Various sources can lead to ocular cellulitis, which is often associated with illnesses or trauma. Here are some key causes:
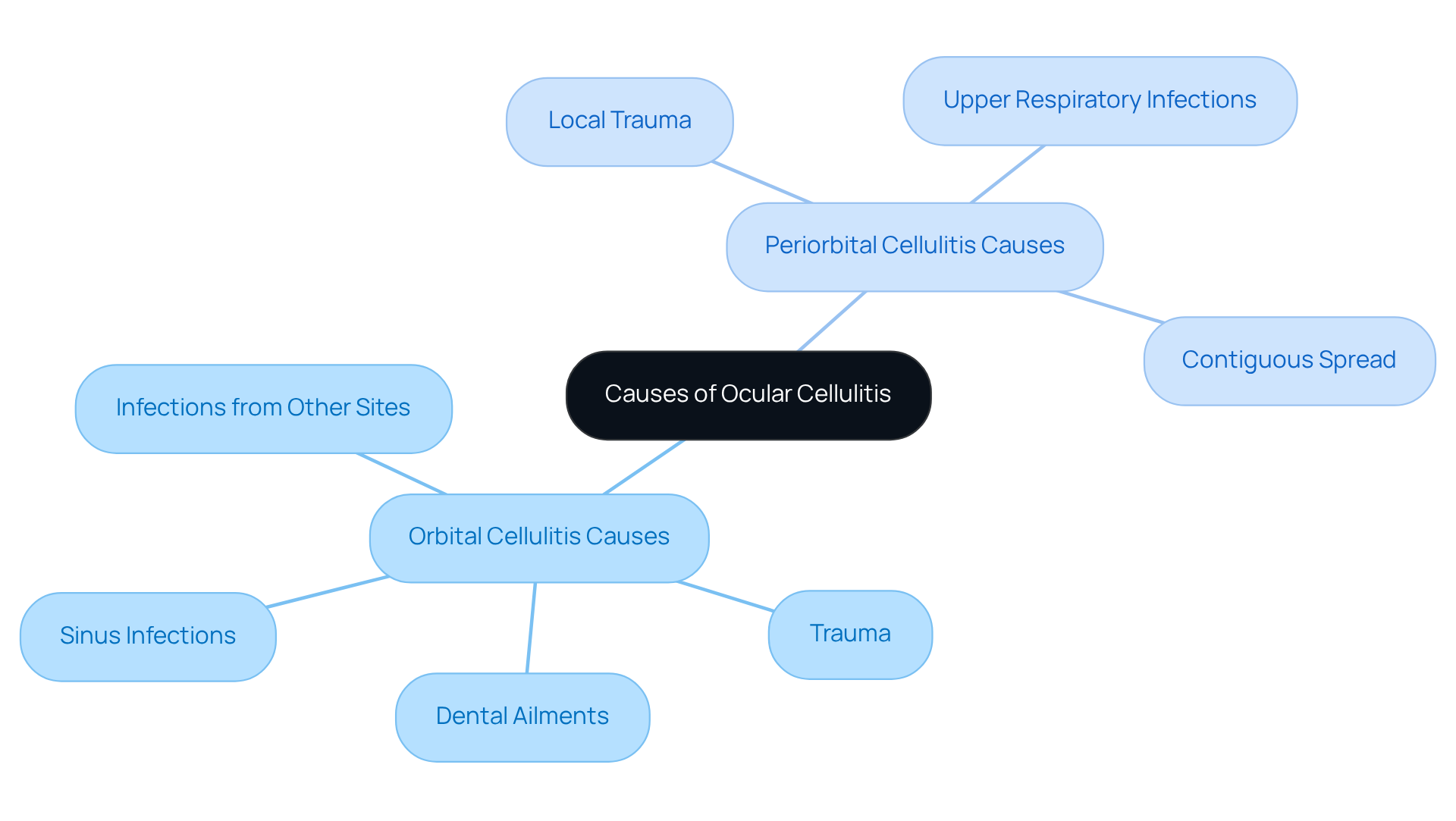
Orbital Cellulitis Causes:
- Sinus infections: The most common precursor, particularly from the ethmoid or frontal sinuses, accounting for over 90% of cases.
- Trauma: Direct injury to the eye or surrounding areas can introduce bacteria, with studies indicating that trauma was the inciting cause in 17.46% of cases.
- Dental ailments: Issues from teeth can extend to the orbit, contributing to the formation of inflammation.
- Infections from other sites: Such as skin conditions or systemic issues, which can lead to orbital involvement.
Periorbital Cellulitis Causes:
- Local trauma: Cuts, insect bites, or scratches on the eyelid can precipitate periorbital cellulitis, often seen in conjunction with upper respiratory infections.
- Upper respiratory infections: These infections often precede periorbital inflammation, particularly in children, underscoring the interconnectedness of respiratory and ocular health.
- Contiguous spread: Infections from nearby areas, such as conjunctivitis or hordeolum (stye), can lead to periorbital inflammation.
We want you to know that understanding these causes helps us provide the best care and support for you. It’s important to seek help right away, as these infections can lead to serious complications, including vision loss and other health risks. Recognizing the signs early can make a significant difference in your recovery and overall eye health.
Understand Diagnosis of Ocular Cellulitis
We understand that dealing with eye issues can be worrying, and knowing how ocular cellulitis is diagnosed can help alleviate your concerns. Diagnosing ocular cellulitis involves a systematic approach that includes:
-
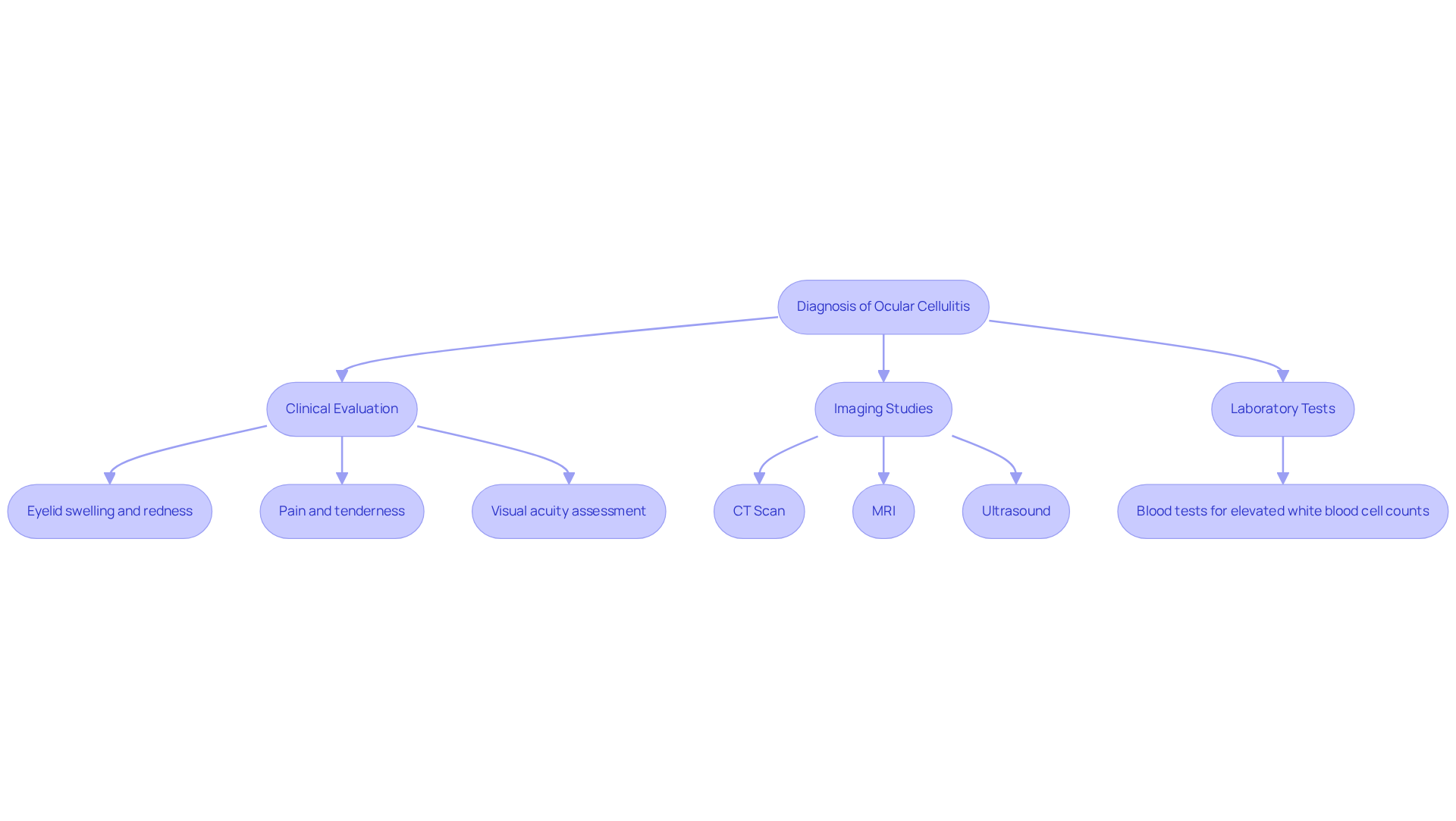
Clinical Evaluation: A thorough history and physical examination are essential. Key indicators include:
- Eyelid swelling and redness.
- Pain and tenderness around the eye may be symptoms of ocular cellulitis.
- Visual acuity assessment.
-
Imaging Studies: If there’s a suspicion of an eye socket infection, imaging is crucial to evaluate the severity. Common modalities include:
- CT Scan: This is the gold standard for evaluating orbital cellulitis, providing detailed images of the orbit and surrounding structures.
- MRI: This can be beneficial in certain situations, especially when soft tissue involvement is suspected.
- Ultrasound: Emerging as a valuable tool, ultrasound can diagnose eye socket infections in many cases without radiation exposure. Studies indicate that ultrasound demonstrated high accuracy, with findings often aligning with those from CT scans.
-
Laboratory Tests: Blood tests may be conducted to check for signs of illness, such as elevated white blood cell counts.
Getting the right diagnosis means you can receive the care you need to feel better.
Review Treatment Options for Ocular Cellulitis
We understand that dealing with a diagnosis of ocular cellulitis can be overwhelming and concerning for you and your loved ones. Treatment for ocular cellulitis depends on the type and severity of the condition, and we’re here to guide you through it.
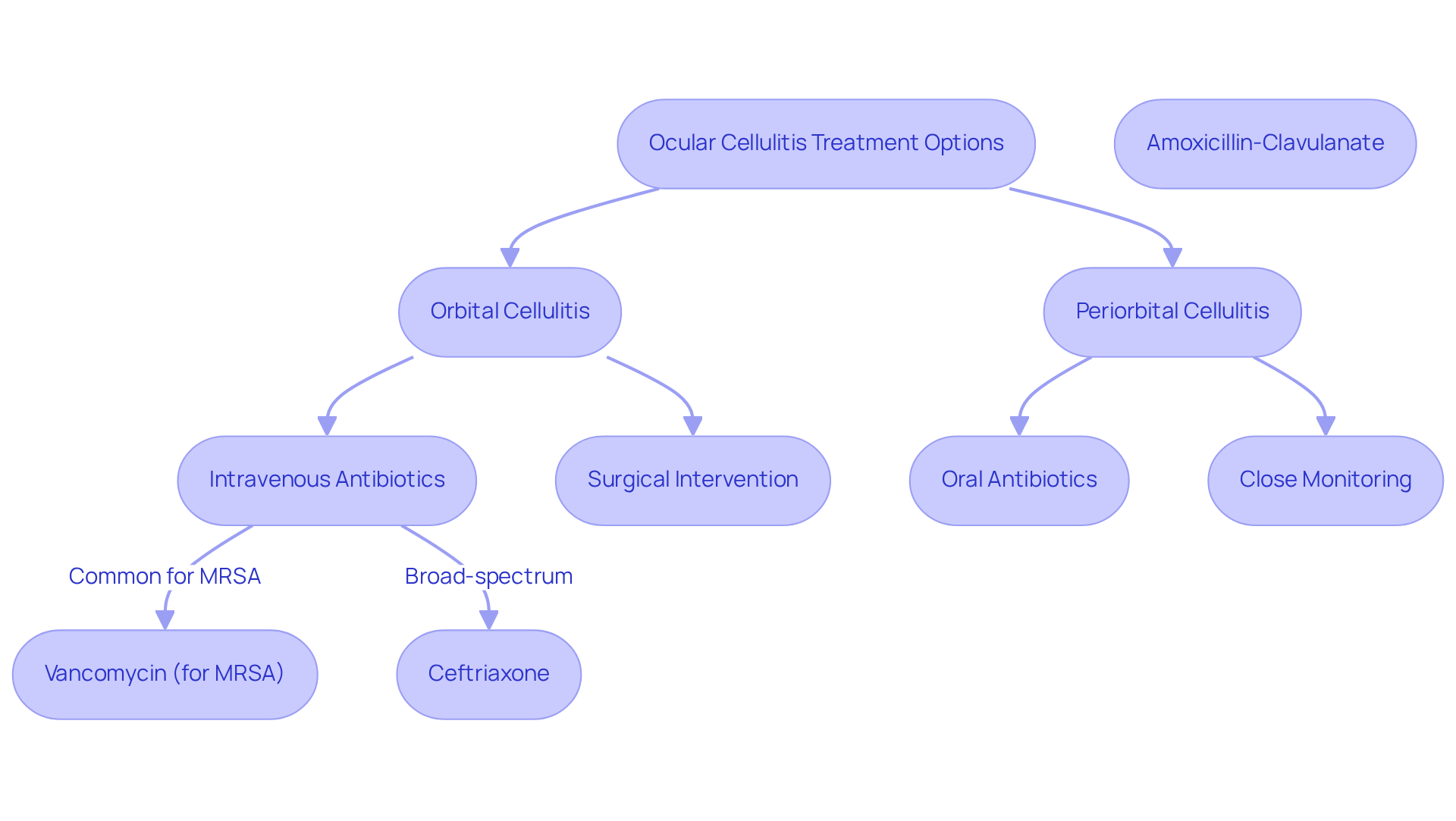
Orbital Cellulitis Treatment:
- Intravenous Antibiotics: We want you to know that starting broad-spectrum antibiotics right away is vital in fighting this infection. Common choices include:
- Vancomycin: Effective against methicillin-resistant Staphylococcus aureus (MRSA).
- Ceftriaxone: Provides coverage for a wide range of bacteria.
- Surgical Intervention: In some cases, if there’s an abscess or severe symptoms, surgical drainage may be necessary. This helps relieve pressure and remove infected tissue, which is important to prevent complications like vision loss. Research highlights that “Prompt and effective antibiotic therapy is essential to prevent life-threatening complications and significant visual impairment in pediatric periorbital infections, particularly in cases involving the eye socket.”
Periorbital Cellulitis Treatment:
- Oral Antibiotics: For mild cases, oral antibiotics like amoxicillin-clavulanate are often sufficient to manage the infection.
- Close Monitoring: We understand that it’s common to feel anxious about your condition. Patients should be closely observed for any signs of progression to an eye infection, which requires immediate medical attention. Studies indicate that “full recovery from orbital cellulitis is expected in most cases with timely treatment,” underscoring the urgency of seeking medical care.
We encourage you to seek timely treatment, as it’s key to avoiding complications and ensuring you recover fully.
Conclusion
We understand that dealing with ocular cellulitis can be overwhelming, especially when it comes to your vision and eye health. Recognizing the differences between orbital and periorbital cellulitis can make a real difference in how quickly you receive the care you need. We’ve shared how these conditions differ, and we want to stress how important it is to recognize symptoms early and reach out for help when you need it.
Key points highlighted include:
- The symptoms associated with each type of cellulitis
- The common causes
- The diagnostic procedures necessary for effective treatment
Orbital cellulitis, a more severe form, often requires aggressive intervention with intravenous antibiotics, while periorbital cellulitis may be managed with oral medications and careful monitoring. It’s common to feel anxious about these treatments, but remember that prompt action can significantly improve outcomes, especially for vulnerable populations like children.
By staying informed about ocular cellulitis, you can take steps that lead to better health outcomes for yourself and your loved ones. It is essential to prioritize eye health and consult healthcare professionals when symptoms arise, ensuring that timely and effective care is received. By staying proactive, you can safeguard your vision and ensure your eye health remains a priority.
Frequently Asked Questions
What is ocular cellulitis?
Ocular cellulitis is a serious infection that causes swelling and irritation of the tissues around the eye, specifically affecting the soft tissues behind the septum that separates the eyelid from the deeper structures of the eye socket.
What are the two main types of ocular cellulitis?
The two main types are orbital cellulitis, which affects the deeper tissues behind the septum, and periorbital inflammation (or preseptal inflammation), which involves swelling of the eyelid and nearby skin in front of the septum.
What are the symptoms of orbital cellulitis?
Symptoms of orbital cellulitis include severe eyelid swelling, redness around the eye, intense pain (especially with eye movement), proptosis (bulging of the eye), vision changes (such as blurred or double vision), and systemic symptoms like fever and malaise.
What are the symptoms of periorbital cellulitis?
Symptoms of periorbital cellulitis include mild to moderate eyelid swelling, localized redness and tenderness, discomfort that is generally less severe than in eye infections, and typically no changes in visual acuity.
Why is it important to recognize the symptoms of ocular cellulitis early?
Early recognition of symptoms is crucial as it allows for timely medical intervention, which can help reduce the risk of complications, including vision loss, which can occur in up to 11% of cases even with treatment.
Who is most at risk for developing ocular cellulitis?
Children aged 5-9 years are particularly vulnerable, with the highest age-specific incidence rate. Additionally, males are affected nearly twice as often as females, and the occurrence of orbital inflammation is higher in Black/African American children compared to White peers.
What are the incidence rates of ocular cellulitis?
The age-adjusted incidence rate (ASR) of eye socket infections is approximately 3.00 per 100,000 person-years, with a crude incidence rate of 2.98 per 100,000 person-years. For males, the ASR is 3.99 per 100,000, and for females, it is 1.96 per 100,000.
List of Sources
- Define Ocular Cellulitis: Orbital vs. Periorbital
- Preseptal Cellulitis Incidence Increasing, Orbital Cellulitis Routinely Discharged from ED (https://reviewofoptometry.com/article/preseptal-cellulitis-incidence-increasing-orbital-cellulitis-routinely-discharged-from-ed)
- Incidence of orbital cellulitis in children: a population-based study (https://jaapos.org/article/S1091-8531(25)00112-0/fulltext)
- Identify Symptoms of Ocular Cellulitis
- Orbital Cellulitis: Background, Etiology, Epidemiology (https://emedicine.medscape.com/article/1217858-overview)
- Epidemiology of Orbital and Preseptal Cellulitis in the United States: A 13-Year Analysis (https://pure.johnshopkins.edu/en/publications/epidemiology-of-orbital-and-preseptal-cellulitis-in-the-united-st)
- Incidence of orbital cellulitis in children: a population-based study (https://jaapos.org/article/S1091-8531(25)00112-0/fulltext)
- The prevalence of patients admitted for orbital and preseptal… (https://researchgate.net/figure/The-prevalence-of-patients-admitted-for-orbital-and-preseptal-cellulitis-A-Age-and-B_fig2_385679469)
- Explore Causes of Ocular Cellulitis
- Orbital Cellulitis: Background, Etiology, Epidemiology (https://emedicine.medscape.com/article/1217858-overview)
- Epidemiology of Orbital and Preseptal Cellulitis in the United States: A 13-Year Analysis (https://pure.johnshopkins.edu/en/publications/epidemiology-of-orbital-and-preseptal-cellulitis-in-the-united-st)
- Characteristics of Patients Treated for Orbital Infections: A Retrospective Study at a Tertiary Care Hospital (https://cureus.com/articles/339639-characteristics-of-patients-treated-for-orbital-infections-a-retrospective-study-at-a-tertiary-care-hospital)
- Incidence of orbital cellulitis in children: a population-based study (https://jaapos.org/article/S1091-8531(25)00112-0/fulltext)
- Understand Diagnosis of Ocular Cellulitis
- Diagnostic test accuracy of ultrasound for orbital cellulitis: A systematic review – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10325084)
- Orbital Cellulitis Workup: Laboratory Studies, Imaging Studies, Procedures (https://emedicine.medscape.com/article/1217858-workup)
- Diagnostic test accuracy of ultrasound for orbital cellulitis: A systematic review (https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0288011)
- Review Treatment Options for Ocular Cellulitis
- How To Recognize Orbital Cellulitis (https://my.clevelandclinic.org/health/diseases/24499-orbital-cellulitis)
- Clinical Practice Guidelines : Periorbital and orbital cellulitis (https://rch.org.au/clinicalguide/guideline_index/Periorbital_and_orbital_cellulitis)
- Antibiotic Choices for Pediatric Periorbital Cellulitis—A 20-Year Retrospective Study from Taiwan (https://mdpi.com/2079-6382/11/10/1288)
- Orbital Cellulitis Treatment & Management: Approach Considerations, Inpatient Care, Pharmacologic Therapy (https://emedicine.medscape.com/article/1217858-treatment)






