Posted by: Northwest Eye in Glaucoma Awareness and Management on March 17, 2026
Introduction
Understanding eye drooping, or ptosis, is essential. We know that this condition often reflects more than just an aesthetic concern; it can signal underlying health issues that may require medical attention. It’s common to feel worried about changes in your appearance, especially when they might affect your well-being.
A significant portion of the population experiences some degree of eyelid droop. That’s why awareness of its causes, symptoms, and available treatments is crucial for maintaining both visual function and overall health. We understand that navigating these concerns can be overwhelming, but you’re not alone in this journey.
What happens when this common condition goes unaddressed? It’s important to recognize that ignoring ptosis can lead to complications. We encourage you to seek timely and effective care. Remember, taking action is the first step towards reassurance and recovery.
Define Eye Drooping: Medical Terminology and Importance
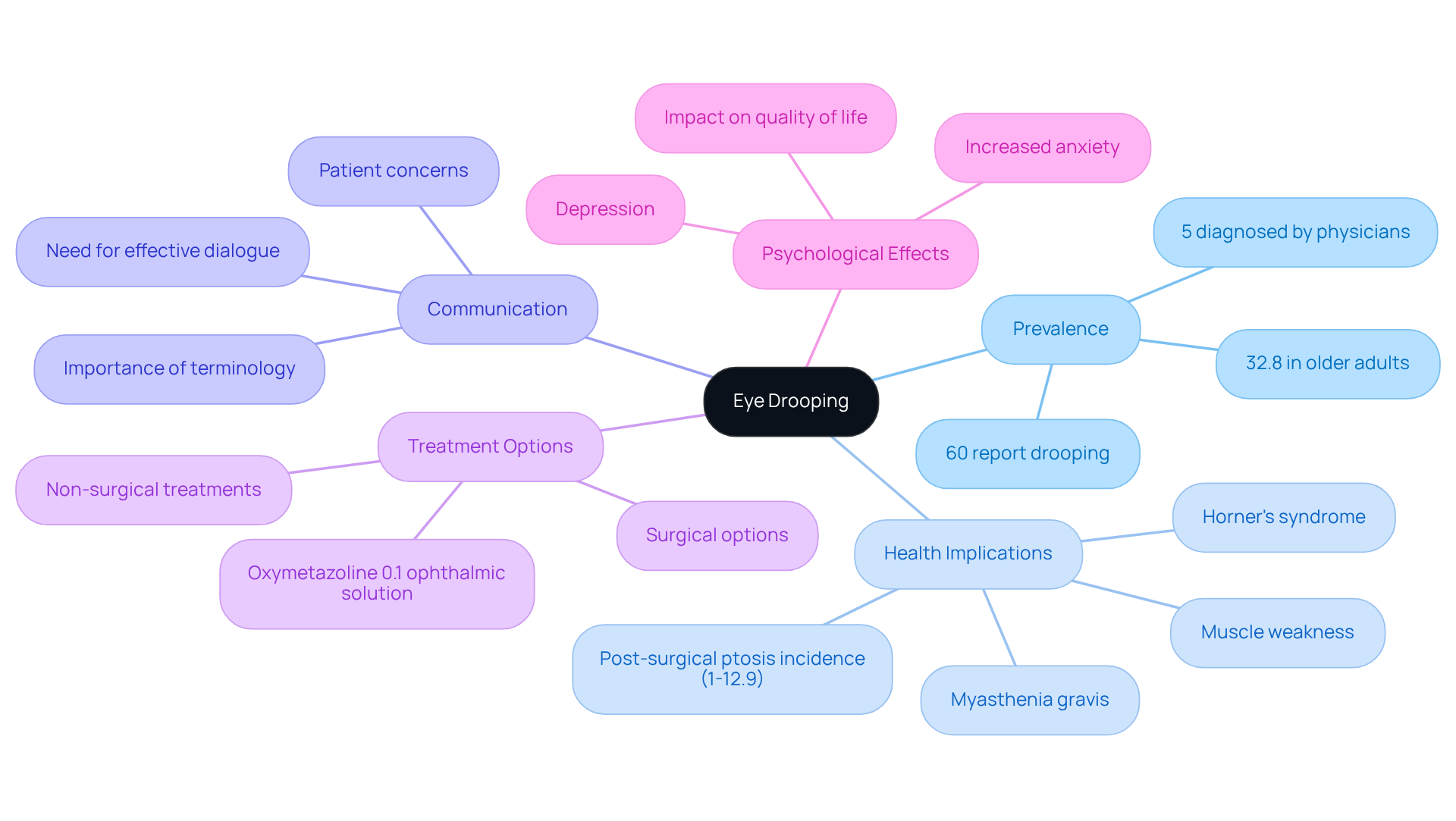
Eye drooping, often known as upper lid droop, can be a concern for many. It involves drooping of the upper eyelid, which may impact one or both eyes. This condition can range from mild drooping that’s barely noticeable to more severe cases that can obstruct vision. It’s important to know that around 60% of people report some level of drooping, yet only about 5% receive a formal diagnosis from a doctor. This gap highlights the need for awareness and proper assessment.
Understanding eye drooping is crucial, as it can sometimes signal underlying health issues, including neurological conditions like Bell’s palsy or myasthenia gravis, as well as other disorders. For instance, a systematic review found that the occurrence of complications after eye surgery can vary from 1% to 12.9%. This emphasizes the importance of careful monitoring for those undergoing surgery. Additionally, eye drooping is significantly more common among older adults, with studies showing rates of 32.8% in individuals aged 70 and older.
We understand that discussing eye conditions can be sensitive. Effective communication is key for individuals to express their concerns and seek appropriate treatment. Ophthalmologists emphasize that knowing the right terminology can help patients articulate their symptoms better. Symptoms like blurred vision, which may accompany eye drooping, can indicate serious conditions or diabetic retinopathy. This underscores the need for professional diagnosis.
Many individuals may not realize that drooping eyelids can be symptomatic of serious health issues, which can lead to delays in seeking help. Heightened awareness and regular assessments during routine eye exams, including visits with a Northwest Eye specialist, can facilitate earlier detection and action. This ultimately enhances your quality of life. Moreover, the serious conditions such as cataracts and the psychological effects of eyelid drooping, such as increased anxiety and depression, highlight the importance of addressing this condition comprehensively.
In summary, eye drooping is not just an aesthetic issue; it can significantly affect visual function and overall well-being. Understanding its implications and communicating effectively with healthcare providers are essential steps for anyone experiencing this condition. Remember, we are here to help you through this process.
Explore Causes of Eye Drooping: Neurological, Muscular, and Environmental Factors
Eye drooping, or ptosis, can arise from various factors, including:
- Neurological Causes: Conditions such as Horner’s syndrome and myasthenia gravis significantly impact eyelid movement. Myasthenia gravis, an autoimmune disorder, affects neuromuscular transmission, leading to muscle weakness, including the levator muscle responsible for lifting the eyelid. Studies indicate that over 50% of patients with myasthenia gravis initially present with ocular symptoms, including ptosis.
- Muscular Causes: Weakness in the levator muscle can result from aging, congenital issues, or conditions like myasthenia gravis. In a cohort study, it was found that 60.2% of patients undergoing ptosis surgery had aponeurotic ptosis, often linked to age-related muscle degeneration. Additionally, muscular causes can be exacerbated by environmental factors, leading to further weakening of eyelid muscles.
- Environmental Factors: Prolonged exposure to sunlight, trauma, or excessive eye strain can contribute to the deterioration of eyelid muscle function over time. These factors can lead to mechanical ptosis, where the eyelid droops due to structural changes rather than neurological or muscular weakness.
Understanding these causes is crucial for determining the most effective treatment options, which may include surgical interventions or medical management for underlying conditions like myasthenia gravis.
Review Treatment Options for Eye Drooping: Surgical and Non-Surgical Approaches
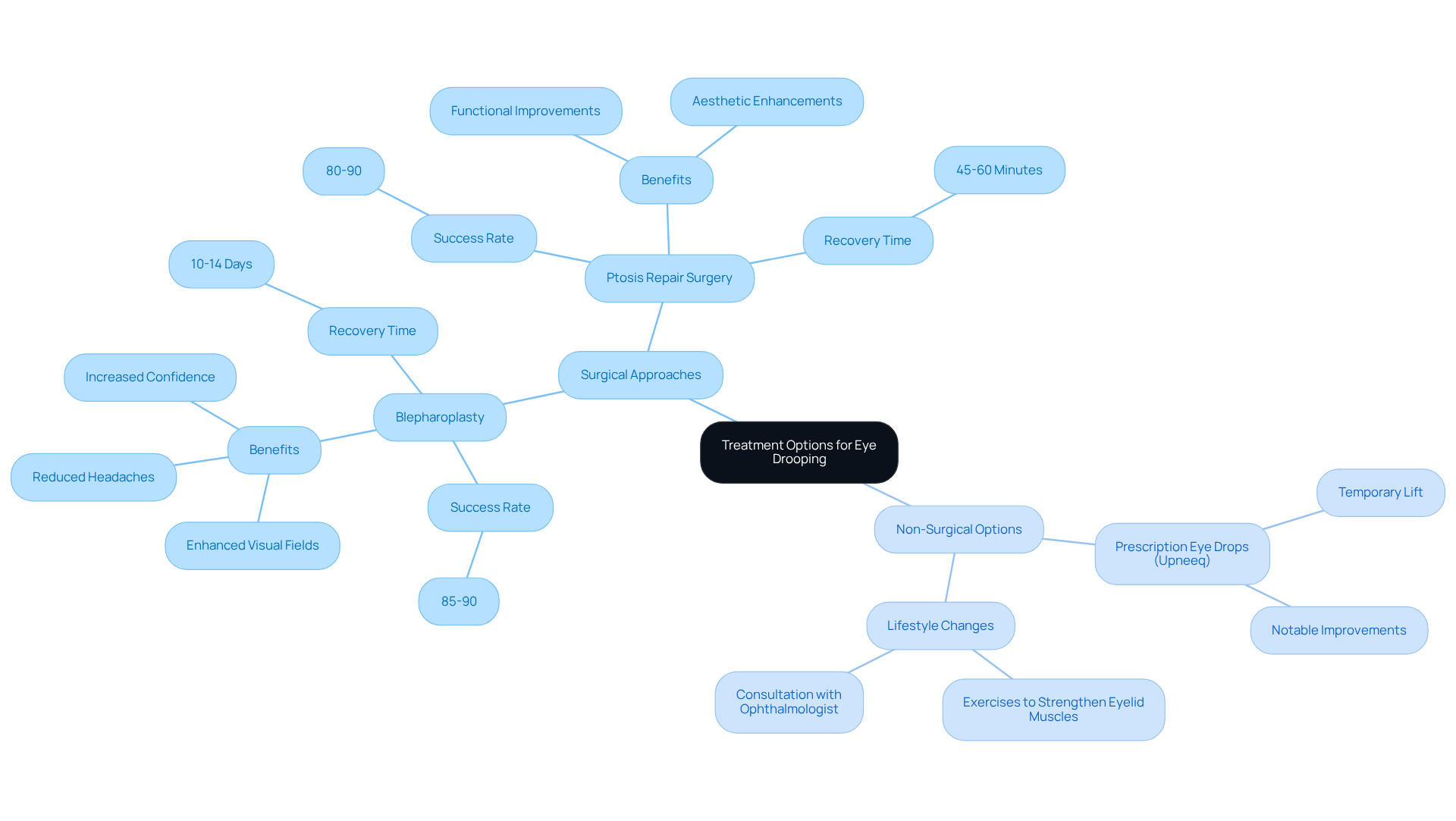
for eye drooping encompass both surgical and non-surgical options, and we recognize that navigating these choices can seem overwhelming.
- non-invasive treatments like prescription eye drops, such as Upneeq. Procedures like blepharoplasty can effectively address drooping by tightening the levator muscle or removing excess skin. With significant aesthetic and functional improvements, many individuals experience benefits. This includes enhanced visual fields and reduced headaches caused by sagging skin around the eyes. Most patients report feeling more confident and youthful after the procedure, which typically lasts 45 to 60 minutes. Recovery is often quick, with many feeling presentable within 10 to 14 days.
- blepharoplasty and ptosis repair surgery. For those with mild cases of ptosis, Upneeq can provide a temporary lift to the eyelid area. Research indicates that Upneeq can lead to notable improvements in the position of the upper eyelid, enhancing both appearance and visual function. Additionally, lifestyle changes and specific exercises may help strengthen eyelid muscles, offering extra support for mild sagging. It’s important to discuss these options with a healthcare provider to find the best course of action tailored to your needs and the severity of your condition.
In summary, there are both surgical and non-surgical therapies available for addressing eye drooping. We are here to help you through this process, ensuring that your choices align with your individual preferences and the severity of your condition.
Understand Post-Treatment Care: Recovery and Monitoring for Eye Drooping
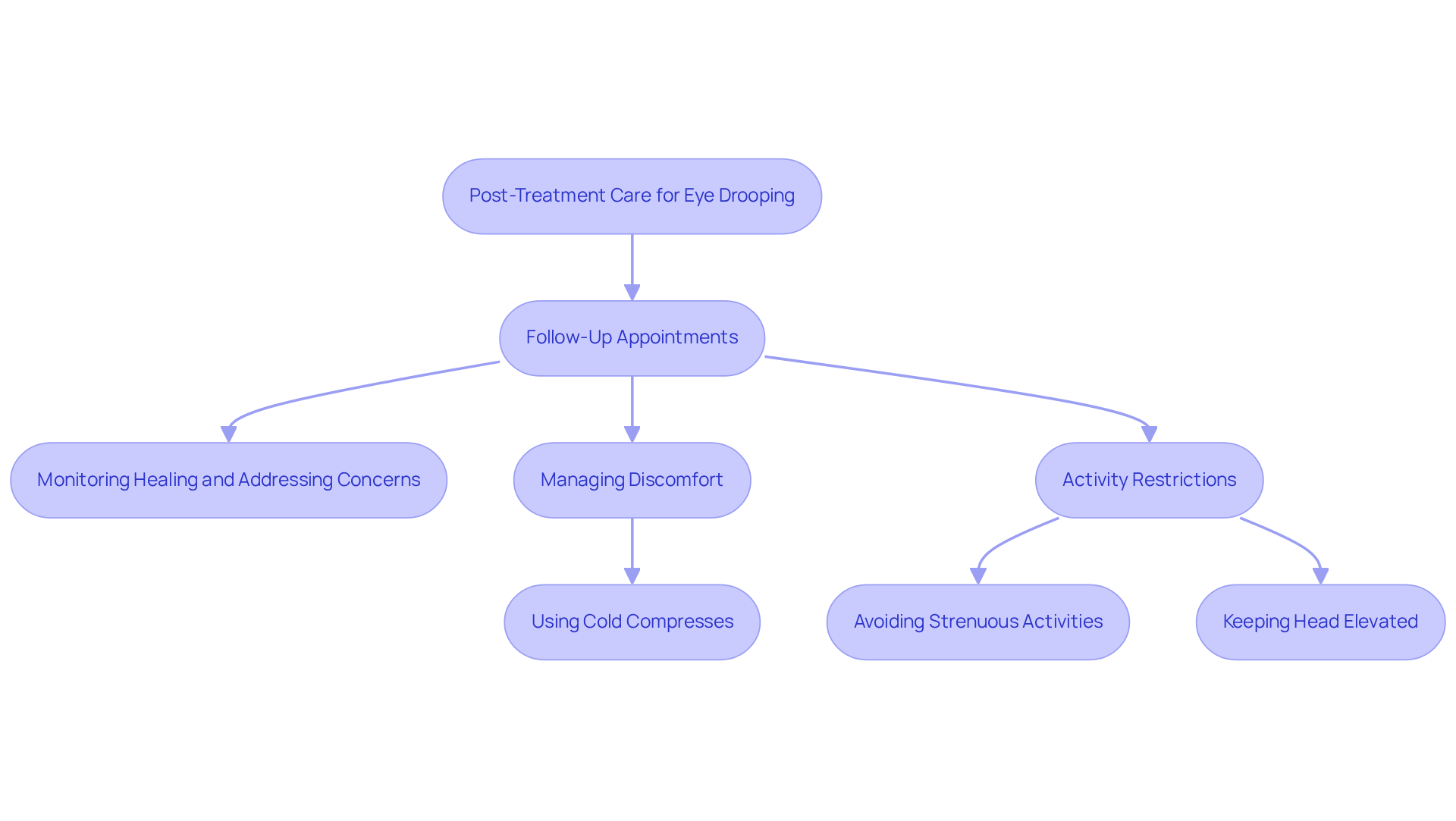
for eye drooping is crucial for ensuring a smooth recovery and achieving optimal results. We understand that this can be a challenging time, and regular check-ins with your ophthalmologist are crucial. These visits allow for monitoring and addressing any concerns that may arise. Prompt interventions can significantly improve outcomes, giving you peace of mind during your recovery.
Managing discomfort is another vital part of your follow-up appointments with your ophthalmologist. It’s common to feel some soreness, and patients are often advised to use cold compresses in the initial days to help reduce swelling and ease any pain. This simple measure can provide significant relief, making your recovery experience more comfortable.
Additionally, adhering to post-operative instructions is important. We recommend avoiding strenuous activities and keeping your head elevated to facilitate healing. Following these guidelines not only supports your recovery but also helps you achieve the best possible results from the procedure. By prioritizing these aspects of monitoring your healing process, you can navigate your recovery with greater confidence and support. Remember, we are here to help you through this process.
Conclusion
Understanding eye drooping, or ptosis, is essential not just for aesthetic reasons but also for its potential implications on your overall health and quality of life. We understand that noticing changes in your eyes can be concerning. This condition can indicate underlying neurological or muscular issues, and recognizing its significance can lead to timely diagnosis and appropriate treatment. It’s common to feel overwhelmed, but awareness of eye drooping is crucial, as many individuals may overlook symptoms that could signal serious health concerns.
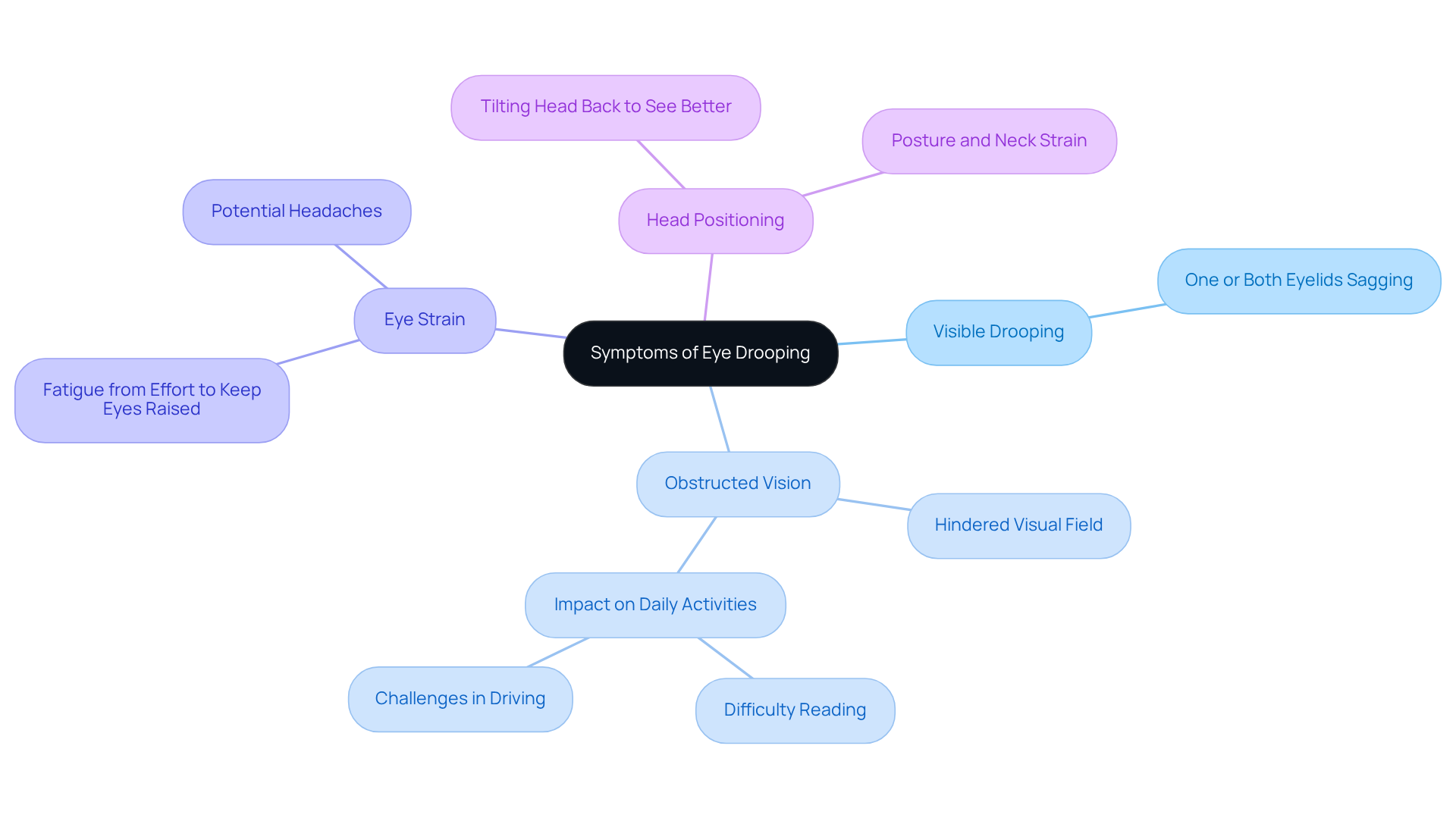
This article provides a comprehensive overview of the various causes of eye drooping, ranging from neurological disorders like myasthenia gravis to environmental factors that can weaken the muscles around your eyes. Recognizing symptoms such as obstructed vision and eye strain is vital, as these can significantly impact your daily activities. We want you to feel informed about the treatment options available, including both surgical and non-surgical approaches, so you can choose the best course of action for your specific circumstances.
Ultimately, addressing eye drooping is vital for enhancing not only your visual function but also your mental well-being. If you’re experiencing symptoms, we encourage you to seek professional evaluation and consider your treatment options seriously. By fostering awareness and understanding of eye drooping, you can take proactive steps toward improving your health and quality of life. Remember, we are here to help you through this process.
Frequently Asked Questions
What is eye drooping and why is it important to understand?
Eye drooping, or upper lid droop, involves the drooping of the upper eyelid, which can affect one or both eyes. It can range from mild to severe cases that obstruct vision. Understanding eye drooping is crucial as it can signal underlying health issues such as neurological conditions and muscle weakness.
How common is eye drooping among the population?
Approximately 60% of people report some level of eye drooping, but only about 5% receive a formal diagnosis from a doctor. This highlights the need for greater awareness and assessment of the condition.
What are some potential underlying health issues related to eye drooping?
Eye drooping can indicate serious underlying health issues, including neurological conditions like Horner’s syndrome and myasthenia gravis, as well as muscle weakness.
How does age affect the occurrence of eye drooping?
Eye drooping is significantly more common among older adults, with studies indicating that 32.8% of individuals aged 70 and older experience this condition.
What symptoms may accompany eye drooping?
Symptoms such as blurred vision may accompany eye drooping and can indicate serious conditions like cataracts or diabetic retinopathy, emphasizing the need for professional diagnosis.
Can eye drooping be treated non-surgically?
Yes, many individuals may not realize that eye drooping can be treated non-surgically, which can lead to delays in seeking help. Regular assessments during eye check-ups can facilitate earlier detection and treatment.
What psychological effects can eye drooping have on individuals?
The psychological effects of eyelid drooping can include increased anxiety and depression, highlighting the importance of addressing this condition comprehensively.
What are the neurological causes of eye drooping?
Neurological causes of eye drooping include conditions like Horner’s syndrome and myasthenia gravis, which can significantly impact eyelid movement.
What are the muscular causes of eye drooping?
Muscular causes can stem from aging, congenital issues, or conditions like myasthenia gravis. A study found that 60.2% of patients undergoing ptosis surgery had aponeurotic ptosis, often linked to age-related muscle degeneration.
What environmental factors can contribute to eye drooping?
Prolonged exposure to sunlight, trauma, or excessive eye strain can lead to the deterioration of muscle function around the eyes, contributing to eye drooping.
Why is recognizing the causes of eye drooping important?
Recognizing the causes of eye drooping is crucial for determining the best treatment options, whether surgical interventions or medical management for underlying conditions.
List of Sources
- Define Eye Drooping: Medical Terminology and Importance
- Ptosis Prevalence in the General Population (https://ascrs.confex.com/ascrs/22am/meetingapp.cgi/Paper/82070)
- A review of acquired blepharoptosis: prevalence, diagnosis, and current treatment options – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8376882)
- The Prevalence and Severity of Acquired Blepharoptosis in US Eye Care Clinic Patients and Their Receptivity to Treatment – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10788066)
- researchgate.net (https://researchgate.net/publication/377294696_The_Prevalence_and_Severity_of_Acquired_Blepharoptosis_in_US_Eye_Care_Clinic_Patients_and_Their_Receptivity_to_Treatment)
- The Ultimate Guide to Assessing Eyelid Ptosis (https://eyesoneyecare.com/resources/the-ultimate-guide-to-assessing-eyelid-ptosis)
- Explore Causes of Eye Drooping: Neurological, Muscular, and Environmental Factors
- Incidence, Epidemiology, and Transformation of Ocular Myasthenia Gravis: A Population Based Study – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC6744973)
- Eyelid Ptosis Causes – Possible Neurological Causes | Dr. Prasad (https://prasadcosmeticsurgery.com/eyelid-ptosis-causes-possible-neurological-causes)
- A review of acquired blepharoptosis: prevalence, diagnosis, and current treatment options – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8376882)
- Myasthenia Gravis Presenting as Persistent Unilateral Ptosis with Facial Droop – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC4476909)
- Identify Symptoms of Eye Drooping: Recognizing Key Indicators
- Surgical quotes for Ophthalmologists. – Eye Centers (https://ecotn.com/ophthalmology-procedure-quotes)
- What Impact Can Droopy Eyelids Have on Vision? (https://seebetterflorida.com/blog/what-impact-can-droopy-eyelids-have-on-vision)
- 15 Inspiring Fred Hollows Quotes | The Fred Hollows Foundation AU | The Fred Hollows Foundation AU (https://hollows.org/latest-news/15-of-fred-hollows-most-inspiring-quotes)
- | OPTH | Dove Medical Press (https://dovepress.com/the-prevalence-and-severity-of-acquired-blepharoptosis-in-us-eye-care–peer-reviewed-fulltext-article-OPTH)
- The psychological well-being and appearance concerns of patients presenting with ptosis – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC3965808)
- Review Treatment Options for Eye Drooping: Surgical and Non-Surgical Approaches
- Nonsurgical Option for Eyelid Lift | Dermatology Times (https://dermatologytimes.com/view/nonsurgical-option-for-eyelid-lift)
- Blepharoplasty Success Rates: 27 Statistics About Eyelid Surgery Outcomes – drmmacdonald.com (https://drmmacdonald.com/blog/blepharoplasty-success-rates-27-statistics-about-eyelid-surgery-outcomes)
- Congenital ptosis repair—surgical, cosmetic, and functional outcome: a report of 162 cases (https://sciencedirect.com/science/article/abs/pii/S0008418212004565)
- Outcomes for severe aponeurotic ptosis using posterior approach white-line advancement ptosis surgery – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5770698)
- Frontiers | Long term risk of recurrence of ptosis repair: implications for surgical counseling and follow-up (https://frontiersin.org/journals/ophthalmology/articles/10.3389/fopht.2025.1689010/full)
- Understand Post-Treatment Care: Recovery and Monitoring for Eye Drooping
- Predictors of patient compliance with follow-up visits after cataract surgery | Request PDF (https://researchgate.net/publication/333627191_Predictors_of_patient_compliance_with_follow-up_visits_after_cataract_surgery)
- Following Up After Cataract Surgery (https://crstoday.com/articles/2020-jan/following-up-after-cataract-surgery)
- Follow-Up After Cataract Surgery – Comparison of the Practice in Two Institutions with the Aim of Optimize the Routine – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC7335894)
- Post-operative Day Zero Versus Day One Follow-Up for Uncomplicated Cataract Surgery – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9578331)
- 2023 MIPS Measure #304: Cataracts: Patient Satisfaction within 90 Days Following Cataract Surgery | MDinteractive (https://mdinteractive.com/mips_quality_measure/2023-mips-quality-measure-304)






