Posted by: Northwest Eye in General on September 17, 2025
Introduction
Understanding migraines can feel overwhelming, especially when they present as painful sensations behind the eye. This specific type of headache, often accompanied by visual disturbances, underscores a complex relationship between neurological health and eye discomfort.
We invite you to explore the causes, symptoms, and effective treatments for migraines behind the eye, gaining insights that may significantly enhance your quality of life. It’s common to feel uncertain, especially with numerous triggers and varying symptoms.
How can one effectively differentiate between a migraine and other types of eye pain? We are here to help you navigate this journey.
Define Migraine and Its Connection to Eye Pain
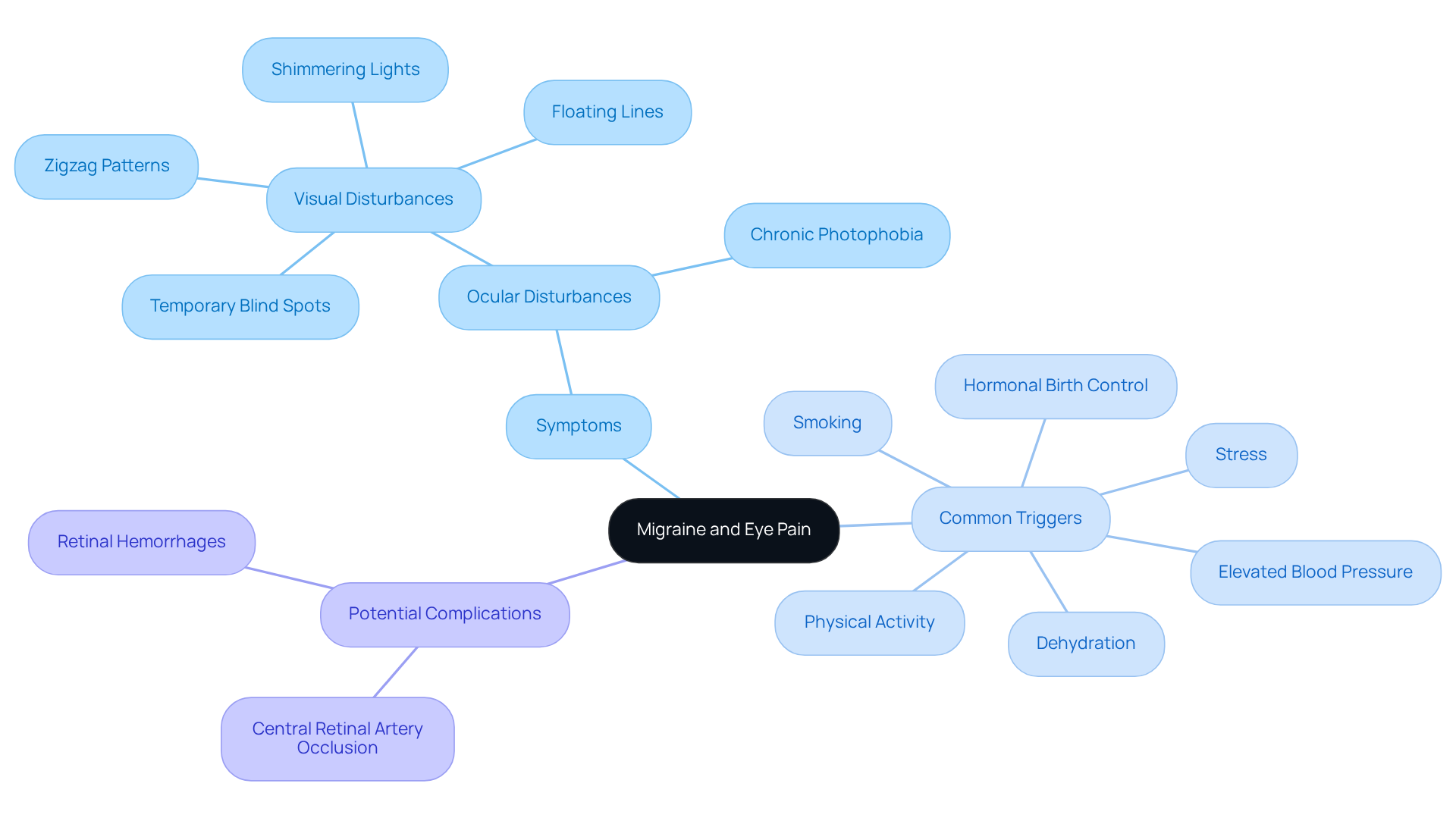
A severe headache is a neurological condition that many people experience, characterized by recurrent pain that can lead to intense throbbing discomfort, often on one side of the head. We understand that this can be distressing, especially when it also results in eye pain and migraine behind the eye, commonly known as a central retinal artery occlusion. These headaches may occur with visual disruptions, such as flashing lights or blind spots, and can be accompanied by a dull ache or pain around the eye. Recognizing this connection is crucial for those facing migraines, as it may indicate a condition that requires attention and management.
Visual disturbances, also known as retinal disturbances, specifically affect vision in one eye and can lead to temporary vision loss. It’s important to note that roughly 20% of individuals with severe headaches experience aura as a precursor to their pain, and about 50% of those who have migraines have a family history of headache disorders. Typically, these visual anomalies last between 10 to 20 minutes, but the visual issues usually resolve within an hour. This highlights the importance of identifying the signs related to headaches and eye health.
Neurologists emphasize the significance of recognizing discomfort indicators like photophobia, as they can greatly affect overall health. For instance, Dr. Kathleen Digre points out that photophobia is a common symptom among those who experience severe headaches, impacting up to 90% of individuals. Furthermore, Dr. Sean Gratton notes that ‘the eye can be essential in the headache mechanism,’ emphasizing the connection between eye pain and headaches. Understanding the multifactorial aspects of headaches, which include genetic, hormonal, and psychological elements, can aid in developing effective management strategies.
Common factors that can trigger a migraine behind the eye include:
- Stress
- Smoking
- Elevated blood pressure
- Hormonal birth control
- Physical activity
- Dehydration
By recognizing these causes and making lifestyle adjustments, individuals can reduce the occurrence and intensity of eye-related headaches, ultimately enhancing their quality of life. It is also essential to be aware of potential complications, such as glaucoma and retinal hemorrhages, which underscore the need for monitoring ocular disturbances.
Explore Causes of Migraine Behind the Eye
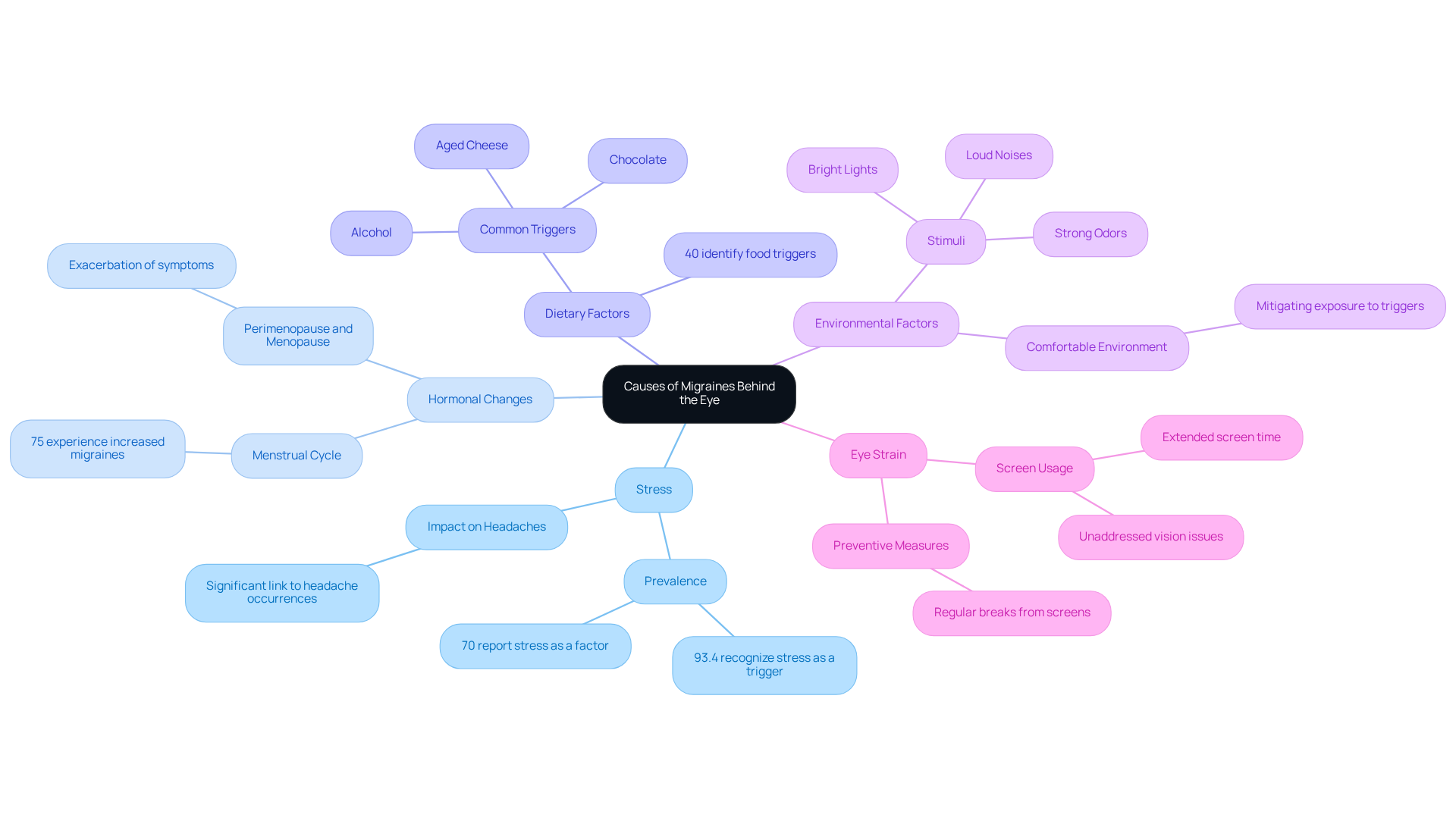
Migraines behind the eye can be triggered by a variety of factors, each contributing to the complexity of this condition. We understand how challenging it can be to navigate these triggers, and recognizing them is the first step toward managing your symptoms effectively. Key triggers include:
- Stress: Emotional and physical stress are significant contributors to tension headaches and migraines. It’s common to feel overwhelmed, and studies show that almost 70% of people suffering from headaches identify stress as a factor, with a significant link between daily stress levels and headache occurrences. Notably, 93.4% of individuals are aware of stress as a migraine trigger, highlighting its prevalence.
- Hormonal Changes: Fluctuations in hormones, especially in women, can trigger severe headaches. Many women experience increased migraine frequency around their menstrual cycle due to drops in estrogen levels; in fact, up to 75% report attacks during this time. Hormonal changes during perimenopause and menopause can also exacerbate symptoms, and it’s important to acknowledge how these changes can impact your well-being.
- Dietary Factors: Certain foods and beverages, such as aged cheeses, alcohol, and caffeine, are frequently mentioned as causes. We know that recognizing personal food triggers can be challenging, but maintaining a headache diary may assist you in tracking your dietary intake and its effects on migraine occurrences. Approximately 40% of patients identify common food causes such as aged cheese and chocolate, so being mindful of your diet can be beneficial.
- Environmental Factors: Bright lights, loud noises, and strong odors can act as environmental stimuli. For instance, exposure to flickering screens or bright lighting can result in migraines behind the eye, causing pain. Many studies identify bright lights and harsh visual contrasts as important factors, and it’s crucial to create a comfortable environment for yourself.
- Eye Strain: Prolonged screen time or uncorrected vision problems can lead to eye strain, which may cause headaches. Ensuring proper vision correction and taking regular breaks from screens can help mitigate this risk. We encourage you to be proactive about your eye health.
Comprehending these causes enables you to recognize patterns in your headaches and take proactive measures to manage your symptoms efficiently. As one headache expert observes, “Identifying individual triggers is essential for creating a customized strategy for headache management.” We are here to help you through this process, and together we can find ways to alleviate your discomfort.
Identify Symptoms of Migraine Behind the Eye
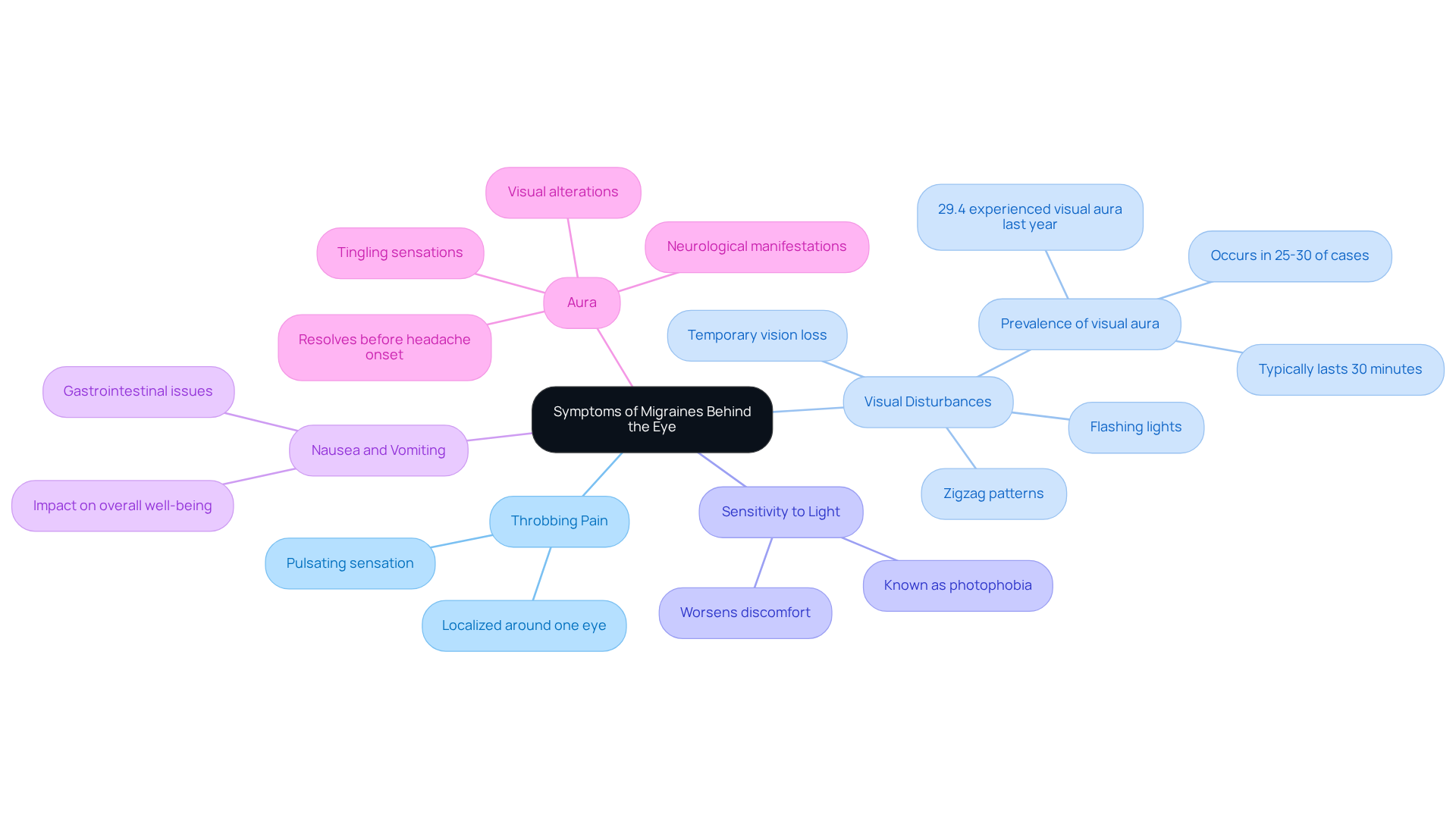
Symptoms of migraines that manifest as eye pain can vary significantly, often presenting as:
- identifying these symptoms is crucial for distinguishing specific headache types A pulsating sensation localized around one eye, which can be particularly intense.
- Migraine encompasses more manifestations than head pain It’s common to experience flashing lights, zigzag patterns, or even visual disturbances in one eye during a migraine behind eye. Studies show that visual aura appears in 25-30% of headache cases, with 29.4% of individuals with headaches experiencing visual aura over the past year, emphasizing its commonality among those affected.
- We are here to help you through this process Heightened sensitivity to light, known as photophobia, is a frequent sign during headache episodes, often worsening discomfort.
- Nausea and Vomiting: Gastrointestinal issues often accompany severe headaches, impacting overall well-being.
- Aura: visual disturbances, referred to as aura, may encompass visual alterations or tingling sensations, typically resolving prior to the onset of the headache.
We understand that migraines differ from others, such as tension or cluster headaches. For example, while tension headaches may show a dull, constant ache, migraines often involve more intense pain that can switch sides. Grasping these differences can assist in pursuing suitable care and managing headaches effectively. As Dr. Vernon Williams points out, ‘common symptoms include sound sensitivity, light sensitivity, and vision problems,’ highlighting the complexity of this condition.
Implement Treatment Strategies for Migraine Eye Pain
Managing pain can feel overwhelming; however, there are effective treatment strategies available. These can be categorized into acute and preventive measures, each designed to support you in your journey to relief.
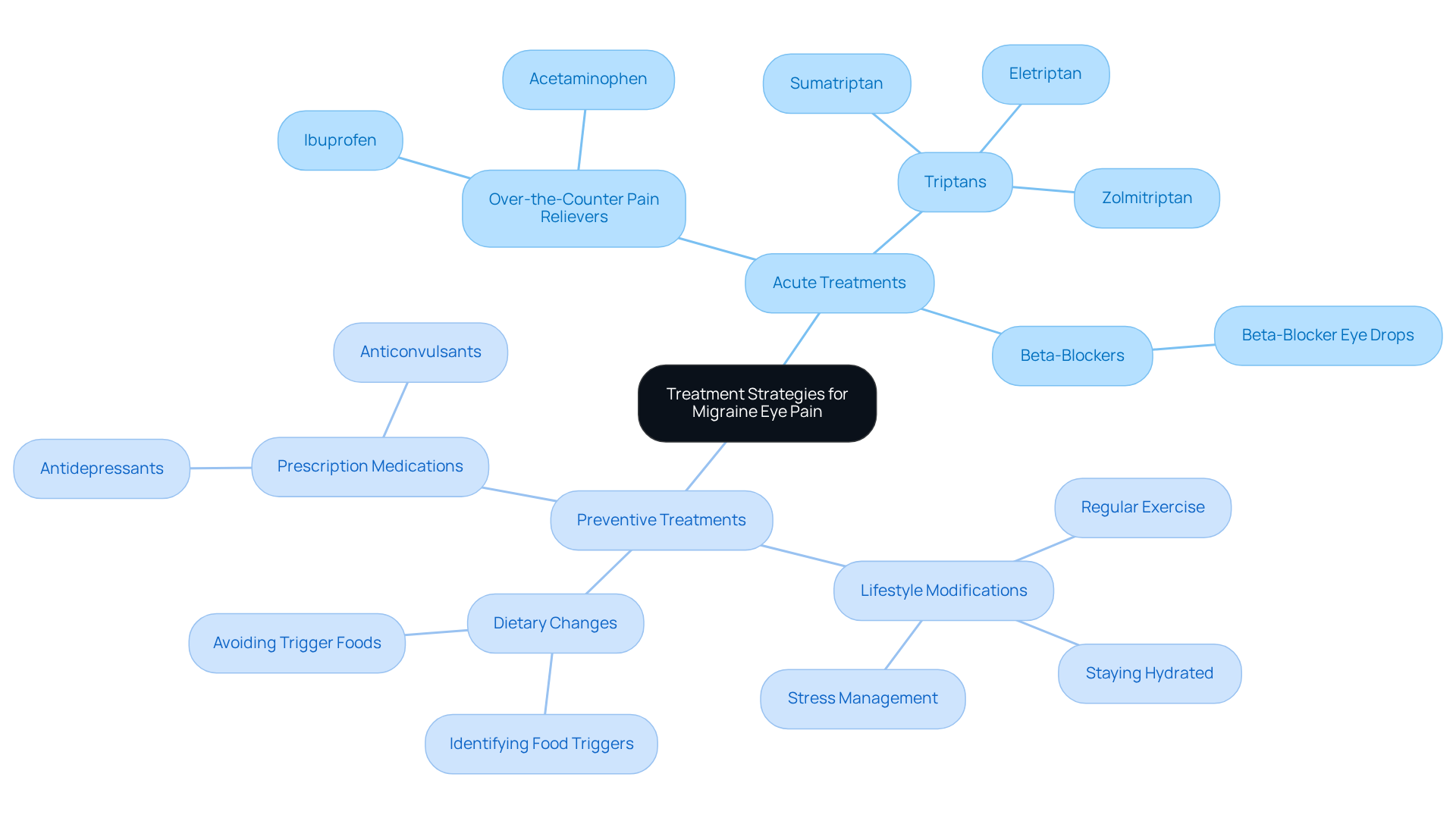
Acute Treatments: When a migraine strikes, immediate relief is essential. You might find comfort in:
- Over-the-Counter Pain Relievers: Medications like ibuprofen or acetaminophen can help alleviate pain.
- Triptans: Prescription medications specifically designed for severe headaches, such as sumatriptan, can be particularly effective.
- Beta-Blockers: Some studies suggest that beta-blocker eye drops may provide relief for acute headache symptoms.
Preventive Treatments: To reduce the frequency and severity of migraines, consider these effective treatment strategies:
- Lifestyle Modifications: Regular exercise, staying hydrated, and managing stress can make a significant difference.
- Dietary Changes: Identifying and avoiding food triggers can greatly reduce headache occurrences.
- Prescription Medications: Preventive medications, including certain antidepressants or anticonvulsants, may be recommended by your healthcare provider.
Implementing these strategies can empower you to manage your symptoms more effectively, ultimately enhancing your overall eye health. Remember, we are here to help you through this process, offering supportive measures every step of the way.
Conclusion
Migraine behind the eye is a complex condition that intertwines severe headaches with eye discomfort, affecting many individuals. We understand that experiencing these symptoms can be challenging, and recognizing this connection is vital for those affected. By understanding the various triggers and symptoms associated with migraines, you can take proactive steps toward alleviating your discomfort and improving your quality of life.
Key arguments explored throughout the article include the identification of common triggers such as:
- Stress
- Hormonal changes
- Eye strain
It’s common to feel overwhelmed by the diverse symptoms that can manifest, including:
- Throbbing pain
- Visual disturbances
Furthermore, treatment strategies, both acute and preventive, empower you to manage your symptoms effectively. By implementing lifestyle modifications and recognizing your personal triggers, you can significantly reduce the frequency and severity of your migraines.
The significance of understanding migraine behind eye pain cannot be overstated. By staying informed about potential causes and treatment options, you can take charge of your health and seek timely medical attention when necessary. Embracing a proactive approach to managing migraines will not only enhance your eye health but also improve your overall well-being. Remember, we are here to help you through this process and support you in finding relief.
Frequently Asked Questions
What is a migraine and how is it connected to eye pain?
A migraine is a severe neurological headache characterized by recurrent, intense throbbing pain, often on one side of the head. It can lead to eye discomfort, commonly referred to as a migraine behind the eye, which may include visual disruptions like flashing lights or blind spots.
What are ocular disturbances and how do they relate to migraines?
Ocular disturbances, or retinal disturbances, affect vision in one eye and can cause temporary vision loss. About 20% of individuals with severe headaches experience these disturbances as a precursor to their pain, and they usually last between 10 to 20 minutes but resolve within an hour.
What symptoms are associated with migraines behind the eye?
Common symptoms include severe headache pain, visual disruptions, and chronic photophobia, which affects up to 90% of individuals who experience migraines.
What factors can trigger a migraine behind the eye?
Common triggers include stress, smoking, elevated blood pressure, hormonal birth control, physical activity, and dehydration.
Why is it important to recognize the connection between eye health and migraines?
Recognizing the connection is crucial because eye discomfort may indicate a migraine that requires attention and management. Understanding the multifactorial aspects of headaches can help in developing effective management strategies.
What complications can arise from migraines related to eye pain?
Potential complications include central retinal artery occlusion and retinal hemorrhages, highlighting the need for timely medical attention for those experiencing eye-related headaches.
List of Sources
- Define Migraine and Its Connection to Eye Pain
- Ocular Migraine (https://my.clevelandclinic.org/health/diseases/24961-ocular-migraine)
- harboreyecare.com (https://harboreyecare.com/2024/05/29/what-to-know-about-ocular-migraine)
- aao.org (https://aao.org/eyenet/article/what-ophthalmologists-need-to-know-about-migraine)
- researchgate.net (https://researchgate.net/publication/380322486_Prevalence_and_burden_of_migraine_in_the_United_States_A_systematic_review)
- frontiersin.org (https://frontiersin.org/journals/neurology/articles/10.3389/fneur.2021.800605/full)
- Explore Causes of Migraine Behind the Eye
- americanmigrainefoundation.org (https://americanmigrainefoundation.org/resource-library/top-10-migraine-triggers)
- thejournalofheadacheandpain.biomedcentral.com (https://thejournalofheadacheandpain.biomedcentral.com/articles/10.1186/s10194-017-0780-8)
- pfizerforall.com (https://pfizerforall.com/migraine/education/common-migraine-triggers)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC8088284)
- thejournalofheadacheandpain.biomedcentral.com (https://thejournalofheadacheandpain.biomedcentral.com/articles/10.1186/s10194-025-02107-y)
- Identify Symptoms of Migraine Behind the Eye
- Migraine Visual Aura | North American Neuro-Ophthalmology Society (https://nanosweb.org/migraine)
- Healthline Quotes Dr. Williams: 6 Things People with Migraine Want You to Know (https://vernonwilliamsmd.com/blog/2022/march/healthline-quotes-dr-williams-6-things-people-wi)
- americanmigrainefoundation.org (https://americanmigrainefoundation.org/resource-library/visual-disturbances-migraine)
- nature.com (https://nature.com/articles/s41598-021-04250-3)
- bjgp.org (https://bjgp.org/content/70/691/88)
- Implement Treatment Strategies for Migraine Eye Pain
- ncbi.nlm.nih.gov (https://ncbi.nlm.nih.gov/books/NBK554507)
- thejournalofheadacheandpain.biomedcentral.com (https://thejournalofheadacheandpain.biomedcentral.com/articles/10.1186/s10194-025-02046-8)
- researchgate.net (https://researchgate.net/publication/387948429_The_use_of_triptans_as_an_effective_form_of_migraine_treatment_-_review)
- Checking your browser – reCAPTCHA (https://pmc.ncbi.nlm.nih.gov/articles/PMC11914668)
- health.harvard.edu (https://health.harvard.edu/pain/these-drugs-might-be-best-to-relieve-migraine-pain)






