Posted by: Northwest Eye in General on January 19, 2026
Introduction
Scleral buckle surgery offers a glimmer of hope for those dealing with retinal detachment, a condition that can deeply impact vision and overall quality of life. This procedure is designed not just to restore sight but also to prevent further complications, highlighting its vital role in modern ophthalmology.
We understand that you may have questions:
- What does the surgery involve?
- What can you expect in terms of preparation, recovery, and potential risks?
It’s completely normal to feel uncertain about these aspects. This article aims to provide a comprehensive guide to help you navigate the journey from surgery to recovery, ensuring you feel informed and supported every step of the way.
Define Scleral Buckle Surgery and Its Purpose
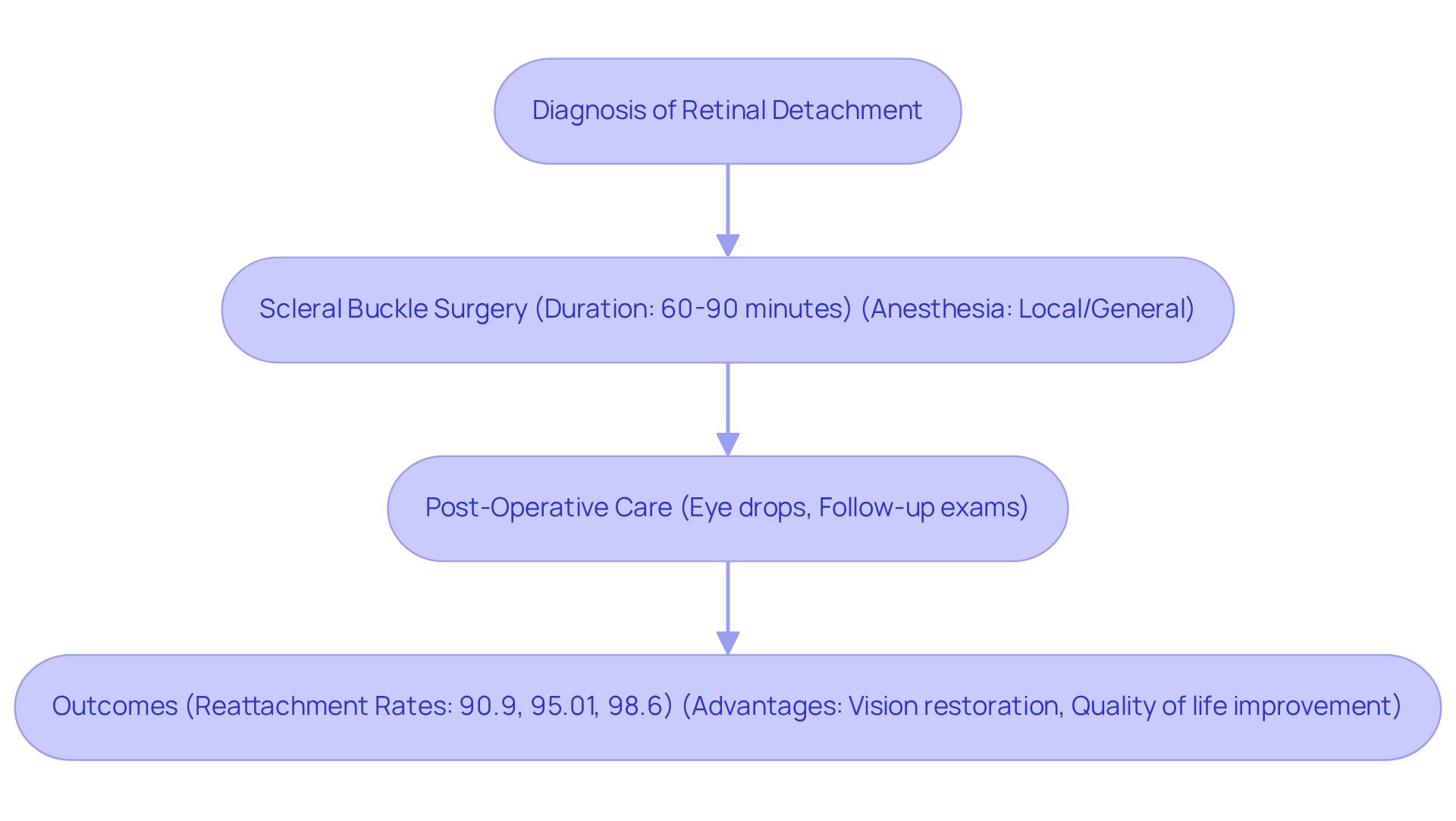
Scleral buckle surgery is a specialized eye procedure designed to help with retinal detachment, a serious condition where the light-sensitive layer of the eye separates from the underlying tissue. We understand that facing such a diagnosis can be overwhelming, but this operation aims to reconnect the retina by placing a silicone band around the eye. This band gently indents the sclera, relieving tension on the retina. Not only does this technique assist in restoring vision, but it also helps prevent further complications related to scleral support procedures.
Ophthalmologists have found scleral buckle surgery to be highly effective, with a reattachment rate of about 90.9% for a single procedure. For primary rhegmatogenous retinal detachments (RRD), the reattachment rate is even higher at 95.01%. When combined with scleral buckle operations, this rate reaches an impressive 98.6%. In 2023, the Retina Service performed 1,679 procedures, with 833 specifically addressing retinal detachments. This highlights how common and vital this procedure is in clinical practice. Real-life stories, like that of Michael, a 55-year-old patient who regained significant vision after his scleral buckle surgery combined with vitrectomy, truly showcase the positive impact of this treatment.
Recent advancements in surgical techniques and materials have further refined the scleral buckle surgery, contributing to its high success rates. Typically performed as an outpatient operation, the procedure lasts between 60 to 90 minutes and can be done under local or general anesthesia. After the surgery, patients are usually prescribed eye drops to prevent infection and are encouraged to attend regular follow-up exams to monitor their healing progress.
The key advantages of scleral buckle surgery include:
- Minimally invasive characteristics
- Capacity to restore vision
- Significant enhancement in quality of life
Many individuals report substantial improvements in their vision, allowing them to return to their regular activities and hobbies. As a cornerstone in the treatment of retinal detachment, scleral buckle surgery continues to be an essential option for both preserving and restoring vision. We are here to help you through this process, ensuring you receive the care and support you need.
Identify Conditions Requiring Scleral Buckling
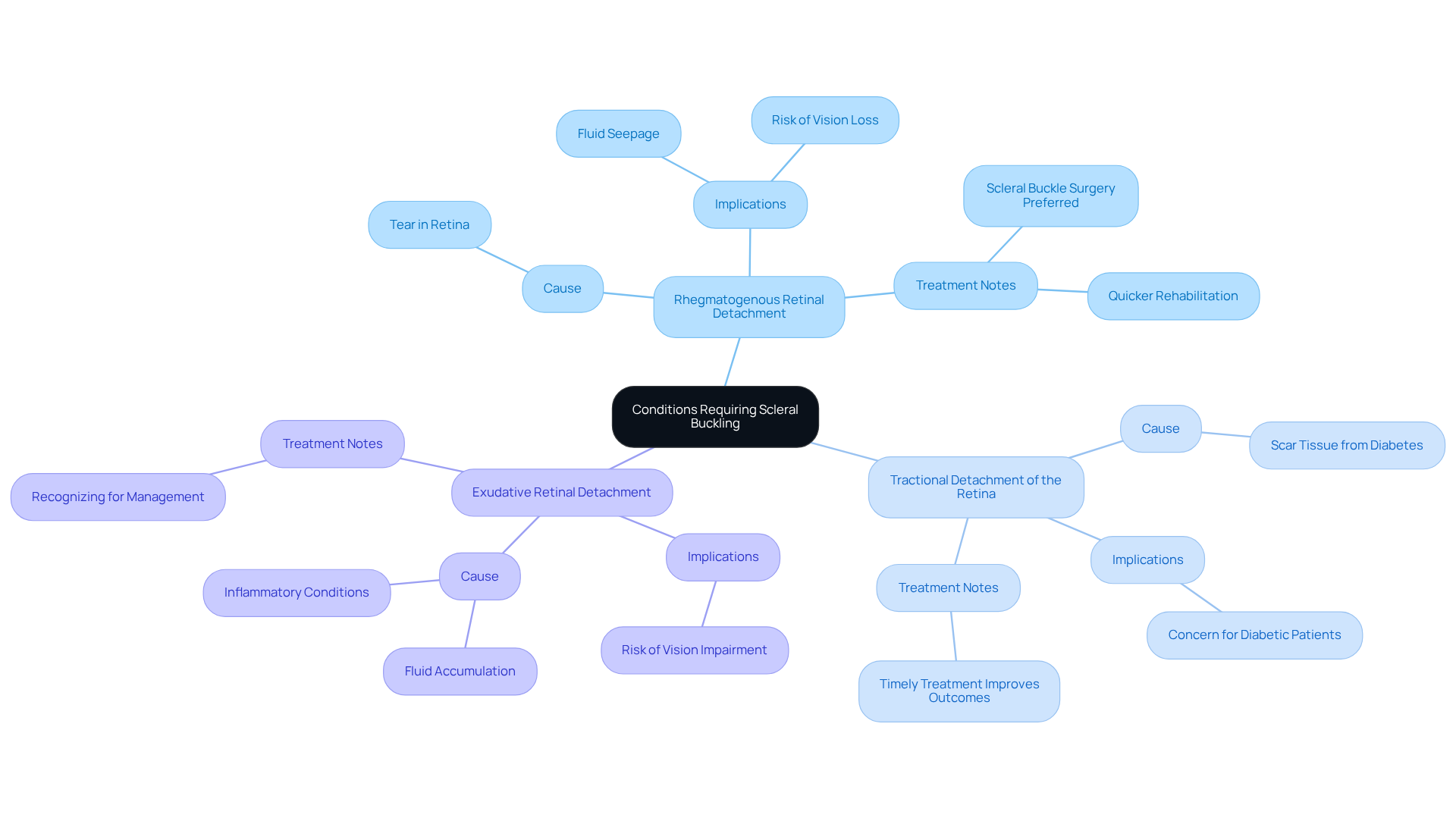
Scleral buckling is primarily indicated for several critical retinal conditions:
- Rhegmatogenous detachment: This condition arises when a tear in the retina allows fluid to seep underneath, leading to detachment. We understand that this can be alarming, and prompt recognition and treatment are essential to prevent irreversible vision loss. Surgery is often favored in uncomplicated cases, especially in eyes with formed vitreous. It can achieve reattachment of the tissue with reduced risk and quicker rehabilitation compared to other methods.
- Tractional detachment of the retina: Commonly associated with diabetes, this type occurs when scar tissue pulls on the retina, detaching it from the back of the eye. It’s common to feel concerned about the connection between diabetes and eye detachment, but understanding this link is crucial for early intervention. Recent studies show that treatment can significantly improve outcomes.
- Rhegmatogenous retinal detachment: This form occurs due to fluid accumulation beneath the eye’s light-sensitive layer without any associated tear, often linked to inflammatory conditions. Recognizing this type is vital for appropriate management, as untreated cases can lead to significant vision loss.
Recognizing these conditions is paramount, as untreated conditions can lead to permanent vision impairment. Scleral buckling can greatly enhance patient outcomes and preserve vision. As Dr. Mahesh P Shanmugam notes, ‘Scleral buckling has been around for over 60 years and is more of an art than a technique,’ underscoring its established role in modern ophthalmic practice. We are here to help you through this process.
Explain the Scleral Buckle Procedure Steps
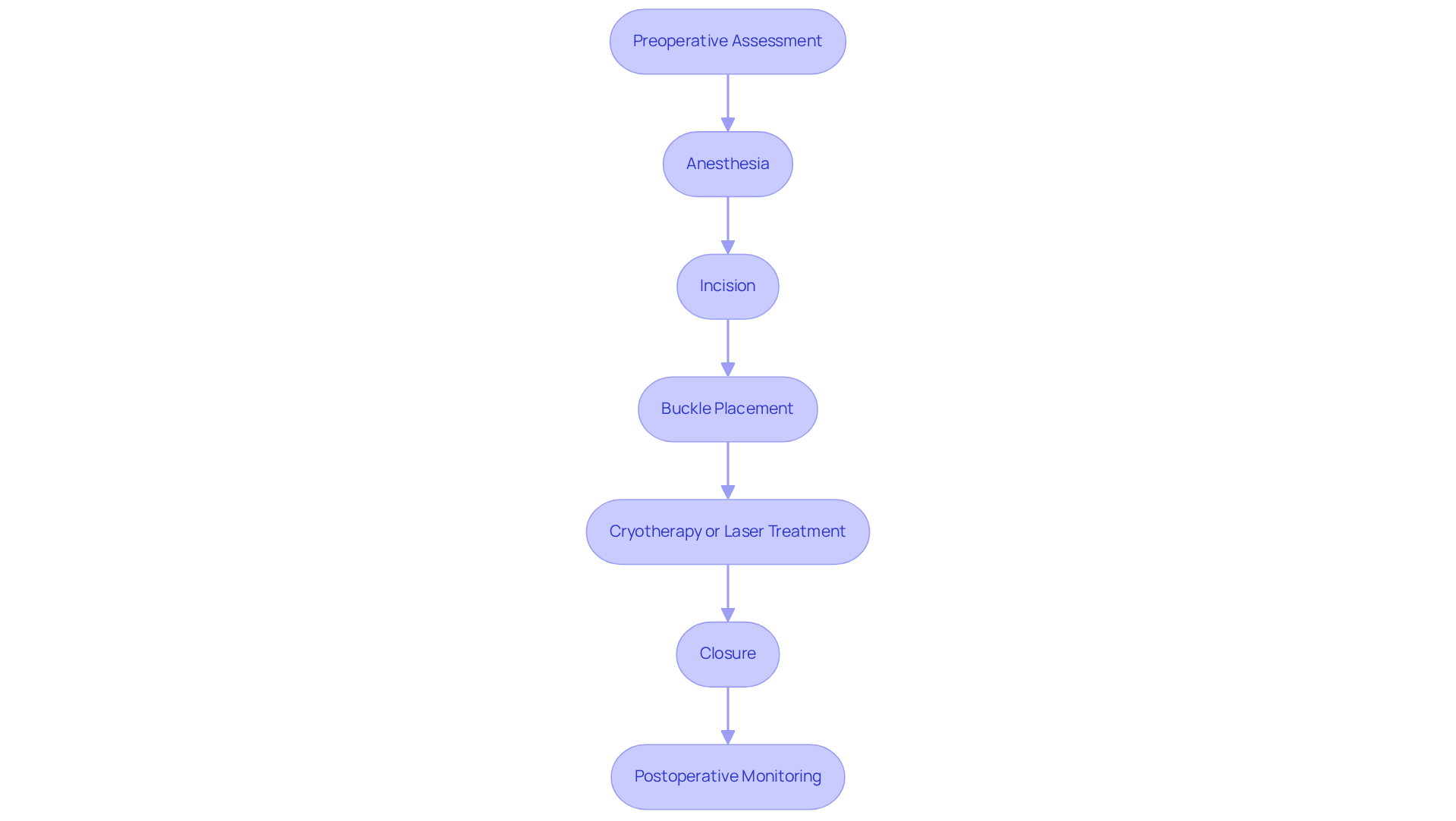
The surgery can feel daunting, but it can help ease your concerns. Here’s a gentle overview of the steps involved:
- Preoperative Assessment: First, a thorough eye evaluation is conducted to assess the extent of the detachment. This helps in planning the best approach for your procedure.
- Anesthesia: To ensure your comfort, local anesthesia is administered to numb the eye, and sedation may be offered to help you relax.
- Incision: A small incision is made in the conjunctiva, the membrane covering your eye, allowing access to the sclera.
- Buckle Placement: A silicone band is carefully placed around the eye. This band indents the sclera, gently pushing the retina back into its proper position.
- Cryotherapy or Laser Treatment: These techniques may be utilized to seal any retinal tears, preventing further detachment.
- Closure: Finally, the conjunctiva is sutured back in place, completing the procedure.
- Postoperative Monitoring: Afterward, you’ll be monitored for any immediate complications before being discharged, ensuring your safety.
Typically, the surgery lasts about 60 to 90 minutes and boasts a high success rate in reattaching the retina. This minimally invasive approach allows many patients to return home the same day, which can lead to quicker recovery times and a smooth return to daily activities. We understand that the thought of surgery can be overwhelming, but surgeons emphasize the importance of proper technique to minimize complications and enhance your outcomes. Remember, we are here to help you through this process.
Prepare for Scleral Buckle Surgery
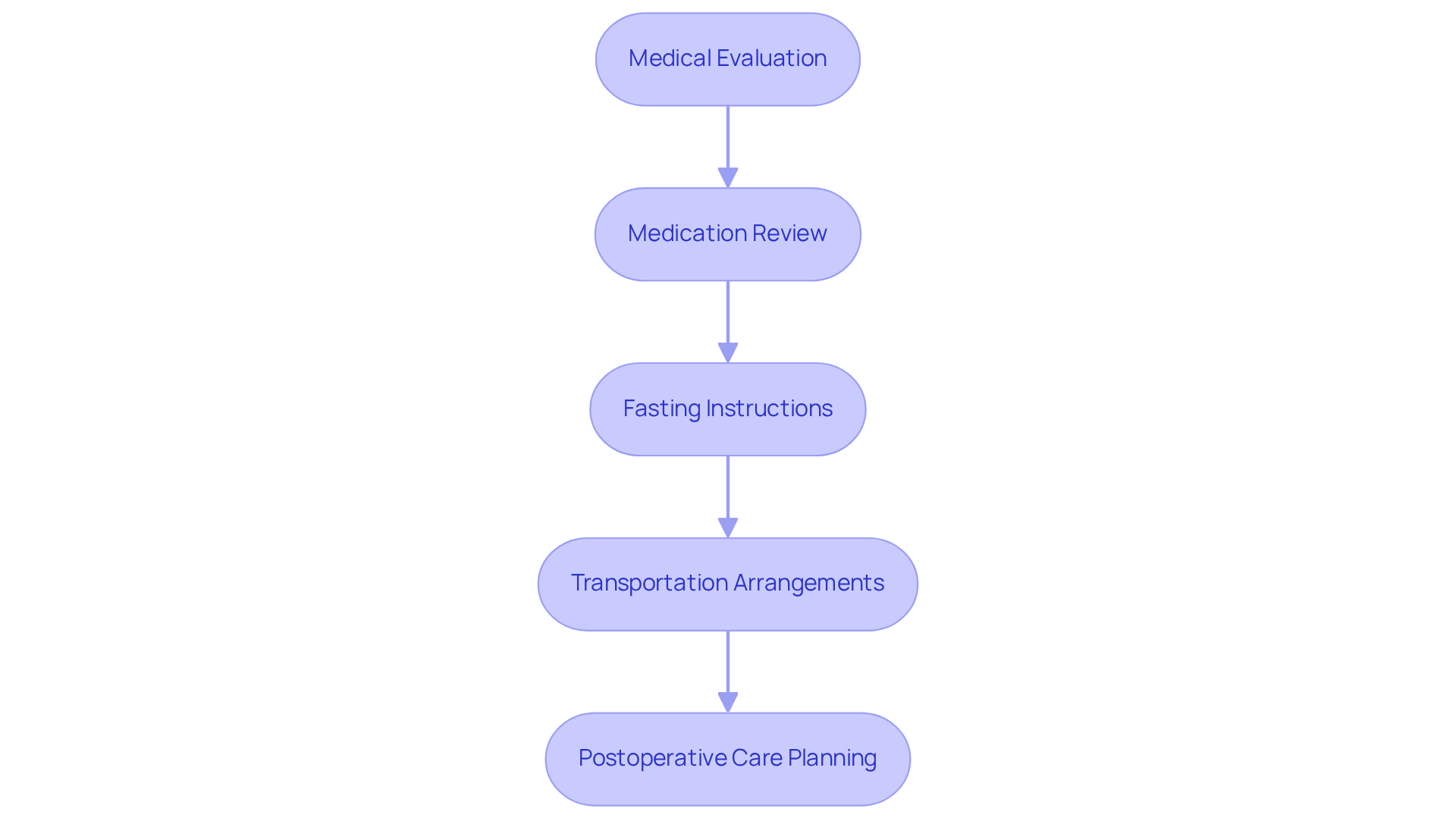
Preparation for scleral buckle surgery involves several essential steps to ensure a smooth experience and optimal recovery:
- Medical Evaluation: A thorough medical evaluation is crucial to identify any underlying health conditions that could impact the surgery. Ophthalmologists have successfully performed scleral buckle surgery for over 50 years, underscoring its importance in eye care.
- Medication Review: Patients must discuss all medications with their ophthalmologist, particularly blood thinners, which may need to be temporarily discontinued to minimize surgical risks.
- Fasting Instructions: It is standard practice for patients to refrain from eating or drinking for a specified period before the procedure to prepare for anesthesia.
- Transportation Arrangements: Given that anesthesia will be administered, it is vital to arrange for a responsible adult to drive the patient home after the surgery.
- Postoperative Care Planning: Patients should plan for their recovery by securing assistance at home, particularly during the first few days post-surgery, as you will need to arrange for someone to help you during this time.
These preparations are not only recommended but are critical for enhancing the likelihood of a successful outcome. As Sonia Kelley, OD, MS, states, “A scleral buckle is a surgery that places a permanent silicone band around the eye to help return the retina into position after a retinal detachment.” Proper planning can significantly impact recovery and overall satisfaction with the surgical experience, as inadequate preparation may lead to complications or dissatisfaction with the outcome.
Outline Post-Operative Care and Recovery
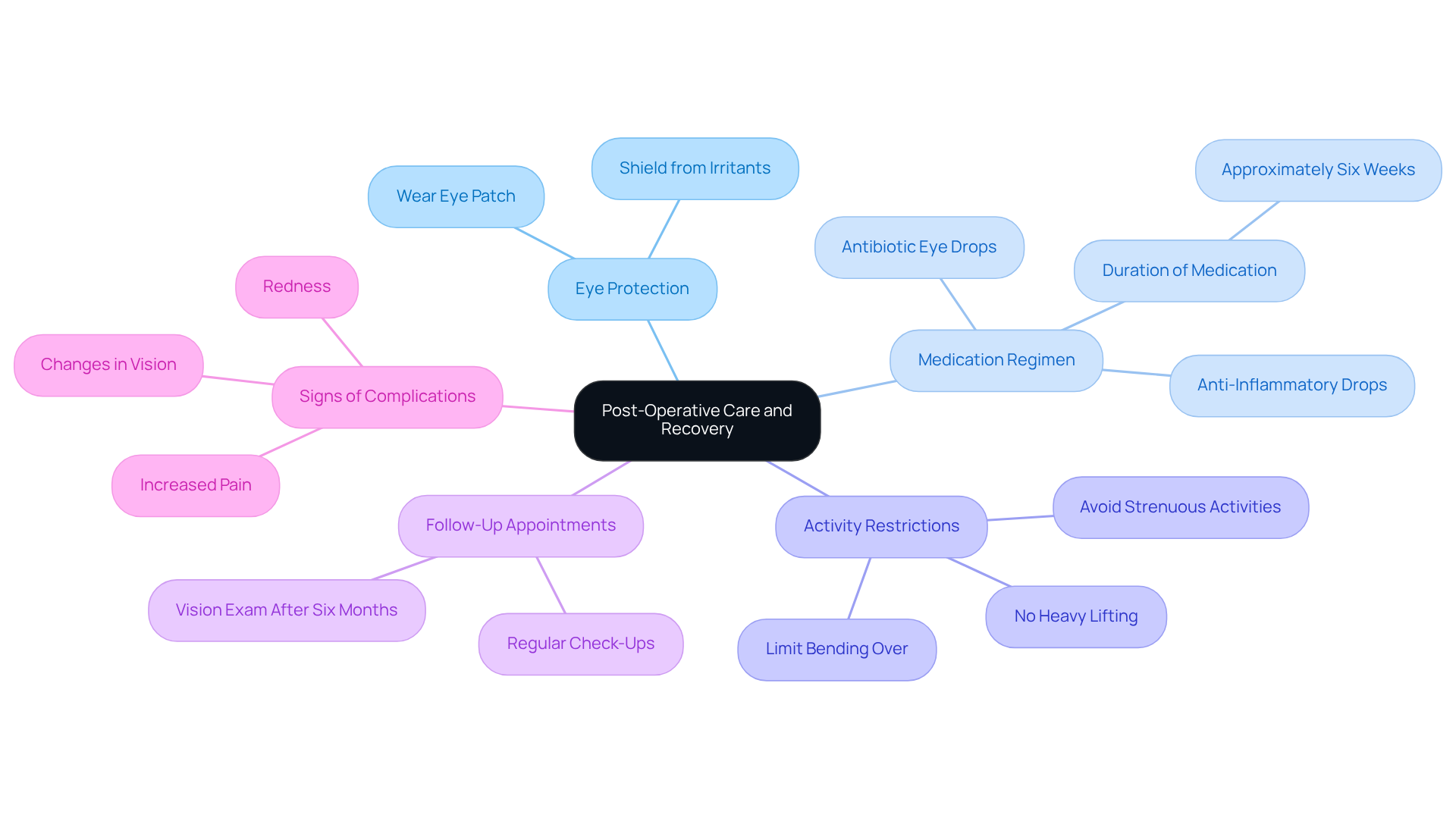
Post-operative care after scleral buckle surgery is crucial for a successful recovery, and we recognize that this can be a challenging time for you. Here are several key components to keep in mind:
- Eye Protection: It’s common to feel concerned about your eye after surgery. Patients are often advised to wear an eye patch for a brief period to shield the eye from potential irritants and to promote healing.
- Medication Regimen: To help prevent infection and reduce inflammation, your ophthalmologist will typically prescribe antibiotic and anti-inflammatory eye drops. These medications are crucial for a smooth recovery, and we want you to feel reassured that they’re there to support you.
- Activity Restrictions: We know it can be frustrating, but it’s important to avoid strenuous activities, heavy lifting, and bending over for several weeks. These restrictions help minimize strain on your eye and support proper healing.
- Follow-Up Appointments: Regular follow-up visits are vital to monitor your healing process. These appointments allow your surgeon to assess your recovery and address any concerns that may arise, ensuring you feel supported every step of the way.
- Signs of Complications: Please remain vigilant for signs of complications, such as increased pain, redness, or changes in vision. If you notice any of these symptoms, prompt communication with your surgeon is essential.
Statistics show that the success rate of scleral buckle surgery for reattaching the retina exceeds 90%. Around 90% of individuals achieve complete restoration of their retina after just one operation. However, it’s normal to experience some discomfort or pain for a few days post-surgery, and your eye may remain red, swollen, and tender for several weeks. Vision may vary for several months due to changes in the eye’s shape caused by the buckle.
Real-life examples show that effective pain management, including the use of cold packs and prescribed medications, contributes significantly to a more comfortable recovery process. Following these guidelines can help ensure a successful outcome and enhance your overall eye health. Remember, we are here to help you through this process.
Discuss Risks and Complications of Scleral Buckle Surgery
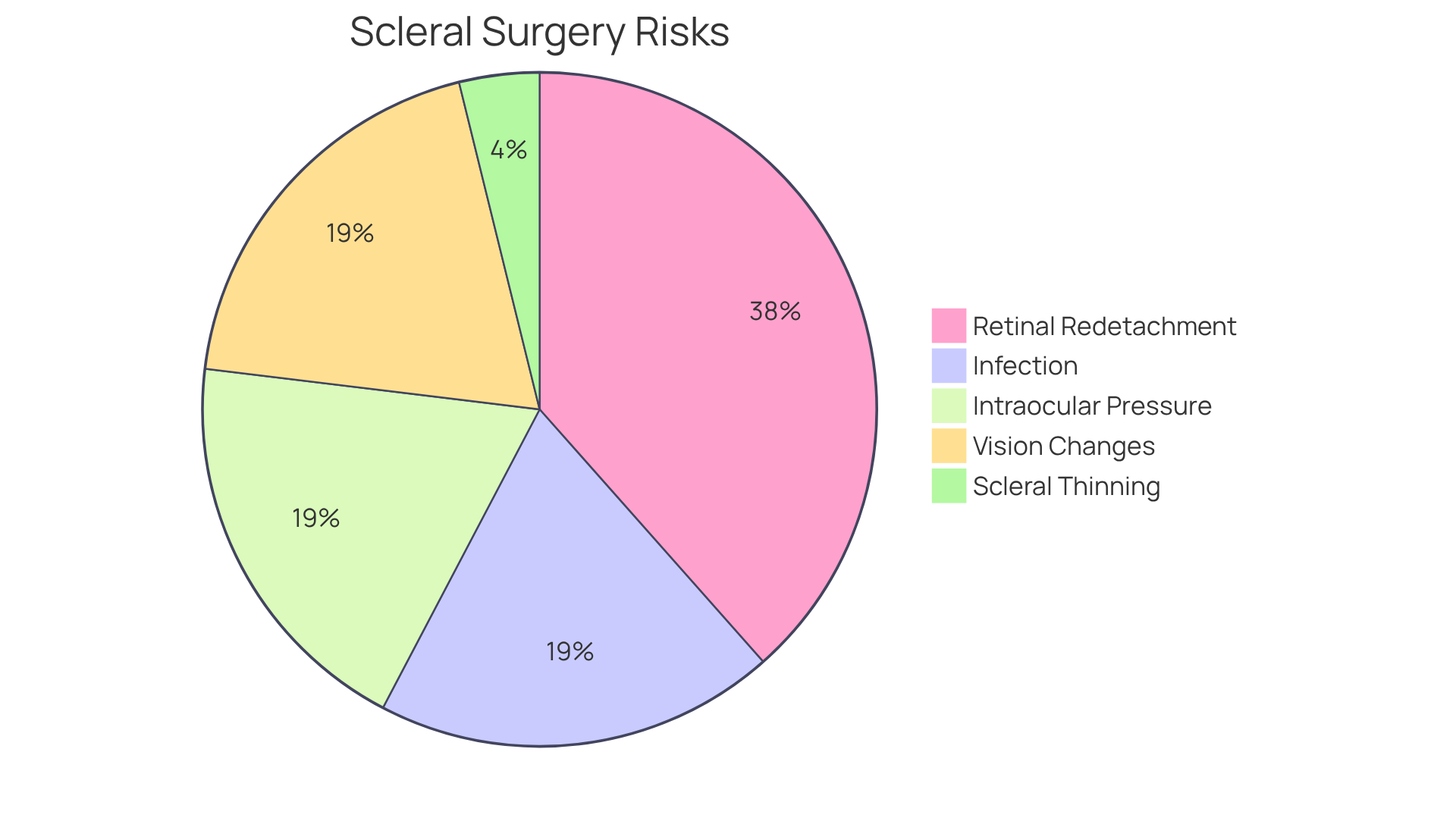
The scleral buckle procedure is generally considered safe, but we understand that you may have concerns about potential risks and complications. One of the most significant worries is retinal detachment, which can happen in about 10% of patients. In such cases, a second procedure might be necessary to fully reattach the retina. However, it’s reassuring to know that scleral buckle surgery successfully reattaches the retina in around 90% of patients, highlighting its effectiveness despite these risks.
Infection is another risk associated with any surgical procedure. While the overall rates of infection are low, it’s crucial to stay vigilant to prevent complications at the surgical site. Additionally, the position of the buckle can lead to increased intraocular pressure, which may pose challenges for those with pre-existing glaucoma. You might also experience vision changes, such as double vision or blurred vision, after the surgery, so careful monitoring during recovery is essential.
In rare cases, scleral thinning can occur due to the device’s positioning, potentially jeopardizing the integrity of the eye. To aid in your recovery and prevent infection, you will need to take prescribed eye drops for about six weeks following the procedure. Understanding these risks is vital as you weigh the benefits of scleral buckle surgery. Retinal specialists emphasize the importance of timely intervention for retinal detachment, as untreated cases can lead to severe vision loss.
Regular follow-up appointments are crucial to monitor your eye’s condition and ensure the procedure’s effectiveness. This allows for prompt action should any complications arise. As one eye care provider shared, “You will need close follow-up care with your surgeon to see if the procedure was effective.” It’s also important to note that the scleral buckle is designed to remain in place permanently, providing long-term support to the weakened or detached retina. We are here to help you through this process, ensuring you feel supported every step of the way.
Conclusion
Scleral buckle surgery is a vital step in managing retinal detachment, focusing on restoring vision and preventing further complications. This minimally invasive procedure uses a silicone band to support the retina and has shown impressive success rates, with studies indicating reattachment rates over 90%. We understand that learning about the procedure, preparation, and post-operative care can ease concerns and improve patient outcomes.
Key insights include the various conditions that may require scleral buckling, such as rhegmatogenous and tractional retinal detachments. The detailed overview of the surgery, along with essential pre-operative and post-operative care instructions, highlights the importance of thorough preparation and attentive recovery practices. While we acknowledge the risks associated with the surgery, like retinal redetachment and infection, the overall benefits of timely intervention are clear, reaffirming the procedure’s crucial role in ophthalmic care.
Ultimately, the experience of scleral buckle surgery goes beyond the technical details; it’s about empowering patients who may be facing potential vision loss. By fostering awareness and understanding of this procedure, individuals can approach their treatment with greater confidence and security. If you’re experiencing symptoms of retinal detachment, seeking timely medical advice and considering scleral buckle surgery could be pivotal in preserving your vision and enhancing your quality of life.
Frequently Asked Questions
What is scleral buckle surgery and what is its purpose?
Scleral buckle surgery is a specialized eye procedure designed to treat retinal detachment, where the retina separates from the underlying tissue. The surgery involves placing a silicone band around the eye to indent the sclera, relieving tension on the retina, helping to reconnect it, restore vision, and prevent further complications.
How effective is scleral buckle surgery?
Scleral buckle surgery has a high success rate, with a reattachment rate of about 90.9% for a single procedure. For primary rhegmatogenous retinal detachment (RRD), the reattachment rate is even higher at 95.01%. When combined with pars plana vitrectomy, the success rate can reach 98.6%.
What conditions require scleral buckling?
Scleral buckling is primarily indicated for rhegmatogenous retinal detachment, tractional detachment of the retina (often associated with diabetes), and exudative retinal detachment (due to fluid accumulation without a tear).
What are the advantages of scleral buckle surgery?
The key advantages of scleral buckle surgery include its minimally invasive nature, the ability to restore vision, and significant improvements in quality of life for many patients.
What is the typical duration and anesthesia used for the surgery?
Scleral buckle surgery is typically performed as an outpatient procedure lasting between 60 to 90 minutes and can be done under local or general anesthesia.
What should patients expect after the surgery?
After scleral buckle surgery, patients are usually prescribed eye drops to prevent infection and are encouraged to attend regular follow-up exams to monitor their healing progress.
Can you provide an example of a patient experience with scleral buckle surgery?
An example is Michael, a 55-year-old patient who regained significant vision after undergoing a scleral support procedure combined with vitrectomy, showcasing the positive impact of this treatment.
Why is timely intervention important for retinal detachment?
Timely intervention for retinal detachment is crucial because untreated cases can lead to permanent vision impairment. Recognizing and treating conditions like rhegmatogenous, tractional, and exudative retinal detachments can greatly enhance patient outcomes and preserve vision.
List of Sources
- Define Scleral Buckle Surgery and Its Purpose
- Surgeon Experience, Detachment Type Can Influence Scleral Buckle Success (https://ophthalmologyadvisor.com/news/scleral-buckle-experience-retinal-detachment)
- What is Scleral Buckle Surgery? – Texas Retina Associates (https://texasretina.com/2022/08/02/what-is-scleral-buckle-surgery)
- Retina Surgery Outcomes | Mass Eye and Ear (https://masseyeandear.org/ophthalmology-outcomes/retina-surgery)
- An Old Technique Made New: Scleral Buckling – Retina Today (https://retinatoday.com/articles/2025-jan-feb/an-old-technique-made-new-scleral-buckling)
- Scleral Buckle: Understanding Its Role in Retinal Detachment Treatment | Northwest Eye (https://nweyeclinic.com/scleral-buckle-understanding-its-role-in-retinal-detachment-treatment)
- Identify Conditions Requiring Scleral Buckling
- Case Study: Rhegmatogenous Retinal Detachment (https://optos.com/blog/2015/feb/case-study-rhegmatogenous-retinal-detachment)
- Why scleral buckling is still relevant – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11168543)
- Explain the Scleral Buckle Procedure Steps
- Scleral Buckle Surgery: Everything You Need to Know (https://allaboutvision.com/treatments-and-surgery/vision-surgery/other/scleral-buckle-surgery)
- Scleral Buckle: Understanding Its Role in Retinal Detachment Treatment | Northwest Eye (https://nweyeclinic.com/scleral-buckle-understanding-its-role-in-retinal-detachment-treatment)
- Scleral Buckle for Retinal Detachment: Three Surgical Approaches (https://eyesoneyecare.com/resources/scleral-buckle-retinal-detachment-three-surgical-approaches)
- Prepare for Scleral Buckle Surgery
- Scleral Buckle Surgery: Everything You Need to Know (https://allaboutvision.com/treatments-and-surgery/vision-surgery/other/scleral-buckle-surgery)
- Outline Post-Operative Care and Recovery
- Scleral Buckle Surgery: Everything You Need to Know (https://allaboutvision.com/treatments-and-surgery/vision-surgery/other/scleral-buckle-surgery)
- Scleral Buckle: Understanding Its Role in Retinal Detachment Treatment | Northwest Eye (https://nweyeclinic.com/scleral-buckle-understanding-its-role-in-retinal-detachment-treatment)
- Scleral Buckling Surgery for Retinal Detachment | Kaiser Permanente (https://healthy.kaiserpermanente.org/health-wellness/health-encyclopedia/he.scleral-buckling-surgery-for-retinal-detachment.hw187645)
- Discuss Risks and Complications of Scleral Buckle Surgery
- Scleral Buckling (https://hopkinsmedicine.org/health/wellness-and-prevention/scleral-buckling)
- Scleral Buckle Surgery: Everything You Need to Know (https://allaboutvision.com/treatments-and-surgery/vision-surgery/other/scleral-buckle-surgery)
- Scleral Buckle | Southeastern Retina Associates (https://southeasternretina.com/retina-treatments/scleral-buckle)






