Posted by: Northwest Eye in Vision Correction on March 25, 2026
Introduction
A keratoprosthesis shines as a beacon of hope for those grappling with severe corneal disease, especially when traditional corneal transplants haven’t worked. This innovative surgical procedure replaces damaged ocular surfaces with artificial lenses, offering the possibility of restored vision for individuals who have run out of options.
We understand that the journey through keratoprosthesis can feel overwhelming. It encompasses the intricacies of surgery, the nuances of recovery, and the risks involved. These aspects raise important questions about its effectiveness and safety.
What can you expect as you navigate this complex landscape of vision restoration? It’s common to feel anxious about the unknown, but rest assured, we are here to help you through this process. Your concerns are valid, and understanding what lies ahead can make a significant difference in your journey.
Define Keratoprosthesis: Understanding the Basics
A keratoprosthesis (KPro) is a surgical procedure that involves replacing a diseased or damaged cornea with an artificial cornea. We understand that facing such a procedure can be daunting, and it’s important to grasp what it entails. The cornea is a clear, dome-shaped layer at the front of the eye, covering the pupil and the colored iris. This transparent part plays a vital role in eye health, helping to maintain a balance of fluid movement in and out of the eye.
When the cornea is damaged, especially in cases of severe disease, a keratoprosthesis can provide a hopeful solution for regaining sight. This option is particularly beneficial for individuals who have struggled with vision loss or who may not be suitable candidates for traditional procedures. One of the most commonly used types is the Boston artificial cornea. It features a central optic held within a cylindrical frame, allowing light to pass through while providing essential structural support to the eye.
We are here to help you through this process, ensuring you feel informed and supported every step of the way.
Outline the Procedure: Steps Involved in Keratoprosthesis Surgery
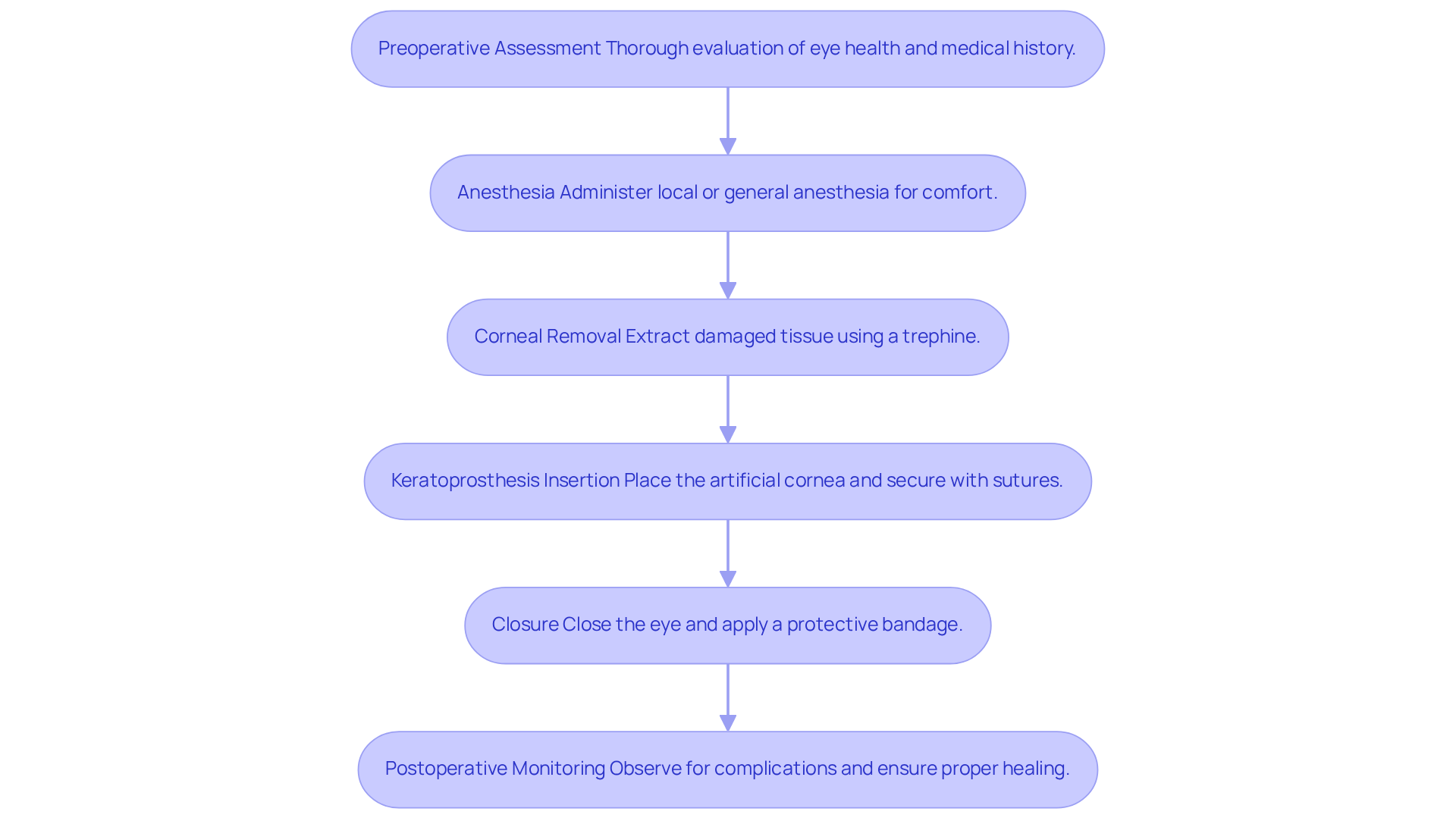
Keratoprosthesis surgery is a complex procedure aimed at restoring vision for those facing severe corneal disease. We understand that this can be a daunting experience, and we’re here to guide you through each step of the process:
- Preoperative Assessment: A thorough evaluation of your eye health and medical history is essential. This helps us determine your suitability for the keratoprosthesis procedure, identify any potential risks, and customize the surgical approach to meet your needs.
- Anesthesia: To ensure your comfort during surgery, we administer either local or general anesthesia. The choice depends on your specific case and preference, allowing for a pain-free experience.
- Corneal Removal: The surgeon carefully extracts the damaged tissue using a trephine, creating a precise circular opening in the eye. This step is crucial for preparing your eye for the keratoprosthesis surgery.
- Keratoprosthesis Insertion: The artificial cornea, known as a corneal prosthesis, is then placed into your eye. It’s secured with sutures to the surrounding tissue, ensuring stability and proper alignment.
- Closure: After the artificial cornea is in place, your eye is closed, and a protective bandage is applied. This bandage aids in the healing process and protects your eye from external factors.
- Postoperative Monitoring: Following surgery, we closely observe you for any immediate complications and to ensure proper healing. This monitoring is vital for addressing any issues that may arise and for assessing the success of the procedure.
Overall, the keratoprosthesis surgery is meticulously coordinated and requires skilled ophthalmologists along with comprehensive postoperative care to enhance your outcomes. Research shows that the retention rate for individuals without autoimmune disease is approximately 95.9% after one year, highlighting the procedure’s effectiveness. As Sharon Fekrat from the Department of Ophthalmology at Duke University mentions, “Primary keratoprosthesis implantation may be recommended in cases that have an anticipated unfavorable prognosis following initial penetrating keratoplasty, such as cases with limbal stem cell deficiency (LSCD).”
It’s important to be aware that issues like retroprosthetic membrane formation can occur in about 30% of individuals, which underscores the significance of understanding potential risks. Remember, we are here to help you through this process.
Detail Recovery: Post-Operative Care and Expectations
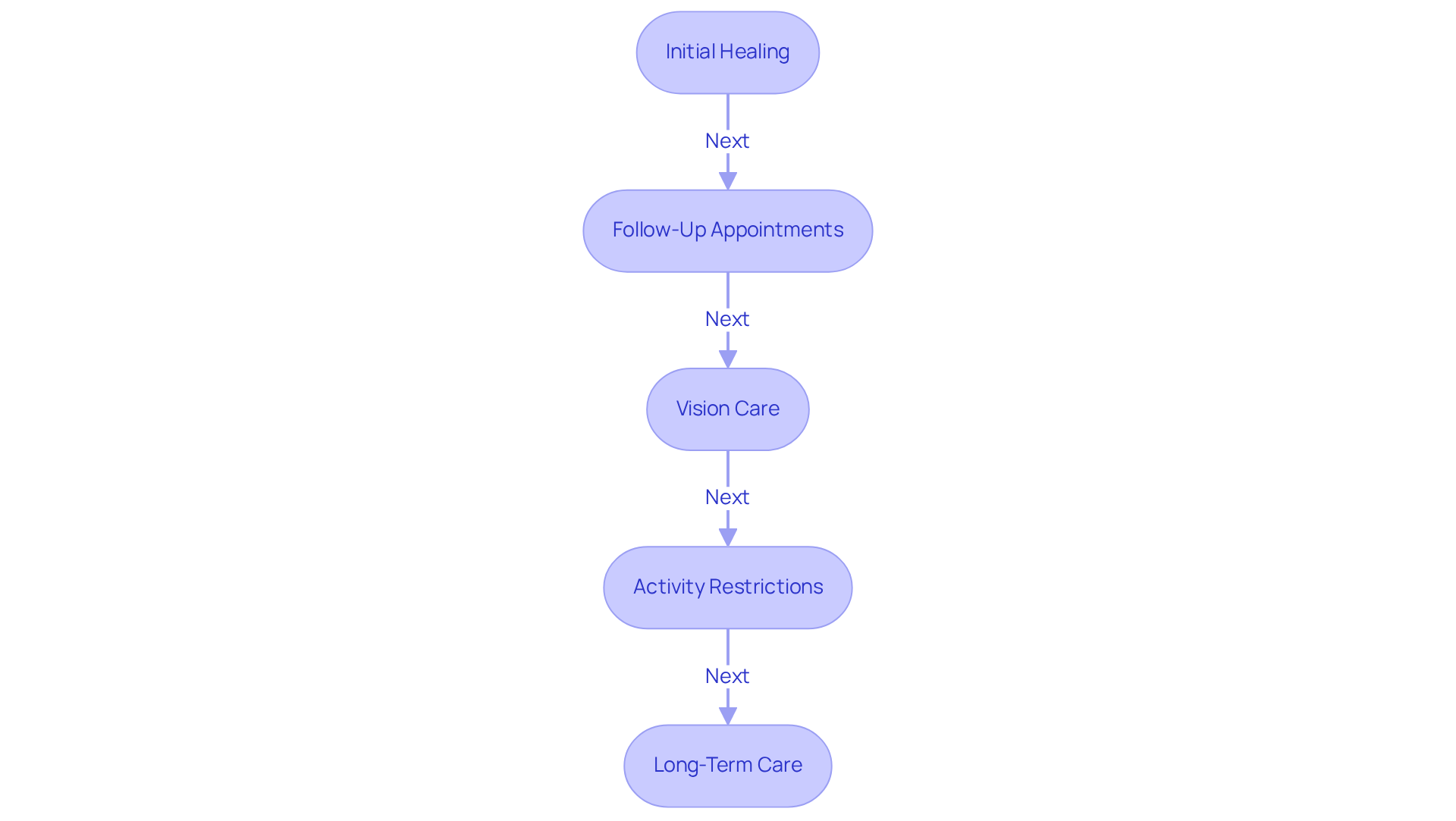
Recovery from keratoprosthesis surgery involves several critical components that we want you to be aware of:
- adhering to post-operative care instructions It’s common to feel discomfort and swelling during the first few days after surgery. We understand that this can be concerning, but rest assured, your recovery will be facilitated through prescribed medications to ensure your comfort.
- significant improvements in vision Regular follow-up visits are crucial for monitoring your healing and identifying any complications early. These appointments typically occur within the first week and continue at regular intervals thereafter. We’re here to support you every step of the way.
- post-operative complications It’s important to refrain from rubbing your eyes and to closely follow the guidance regarding drops and medications. This helps prevent infection and promotes optimal healing. Remember, you’re not alone in this; many patients have successfully navigated this process.
- Follow-Up Appointments We advise you to avoid strenuous activities and heavy lifting for several weeks to support your recovery. It’s normal to feel a bit restless, but taking it easy will help you heal better.
- Activity Restrictions Ongoing care may involve using a bandage contact lens and regular assessments to manage potential complications, such as glaucoma or retroprosthetic membranes. We’re committed to ensuring your long-term health.
Statistics show that approximately 49.7% of patients experience complications, which highlights the importance of diligent follow-up and care. However, many patients report positive outcomes following recovery from keratoprosthesis surgery, with 70% of eyes achieving visual acuity of 20/200 or better within the first year post-surgery. Eye care professionals emphasize the necessity of follow-up visits to maximize your recovery outcomes.
We are here to help you through this process, and we encourage you to reach out with any questions or concerns.
Discuss Risks: Understanding Potential Complications of Keratoprosthesis
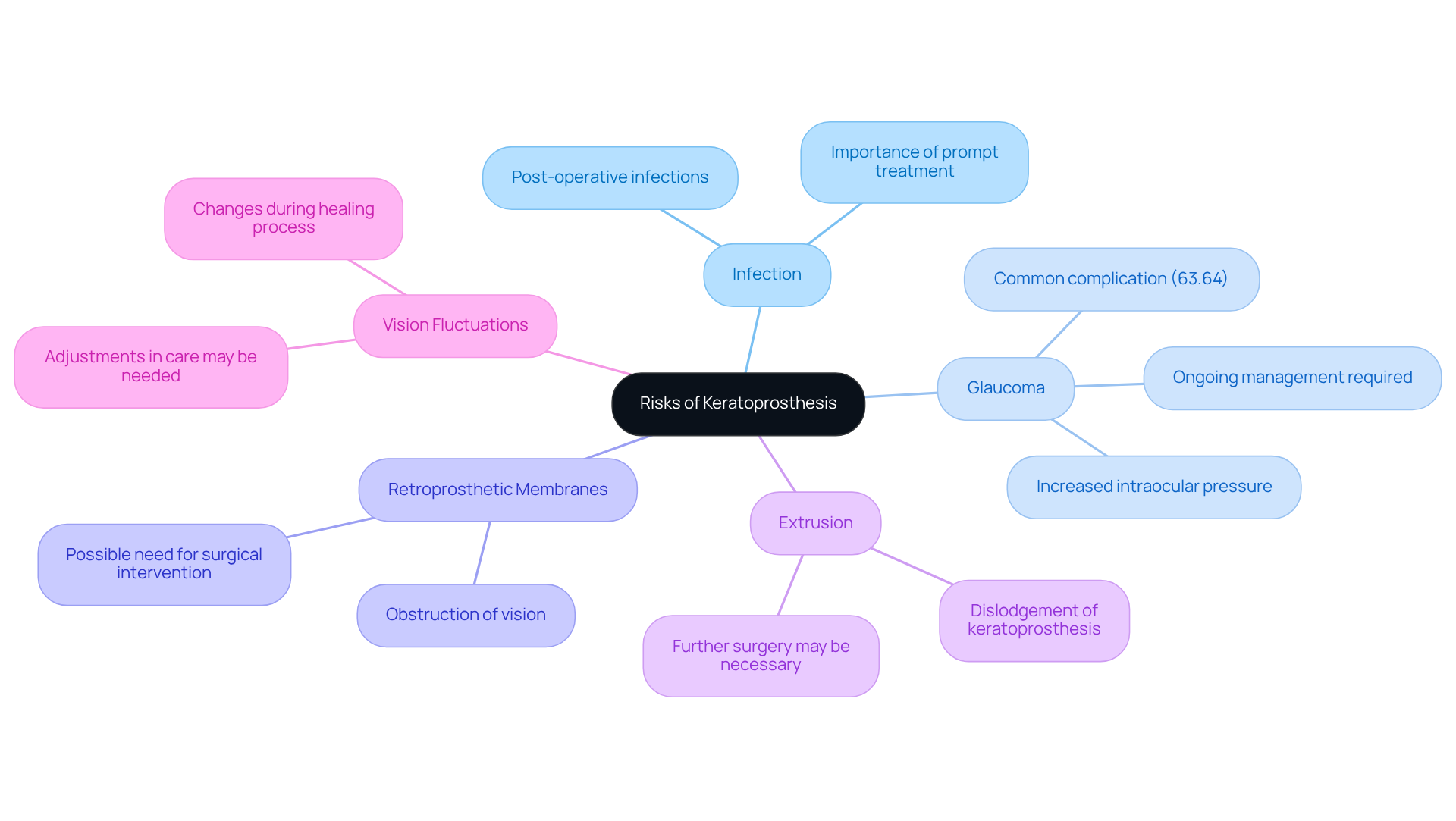
While the use of keratoprosthesis can significantly improve vision, we understand that it’s important to be aware of the potential risks involved. Here are some key considerations:
- Infection: Post-operative infections can occur, and it’s crucial to seek prompt treatment to prevent any risk of vision loss.
- Glaucoma: Increased intraocular pressure is a common complication that may require ongoing management. It’s common to feel concerned about this, but rest assured, your healthcare team will guide you through it.
- Retroprosthetic Membranes: These can develop behind the artificial cornea, potentially obstructing vision. If this happens, surgical intervention may be necessary, but we’re here to support you every step of the way.
- Extrusion: In some cases, the keratoprosthesis may become dislodged or may experience extrusion from the eye, which would necessitate further surgery. We know this can be worrying, but your care team will be prepared to address any issues.
- Vision Fluctuations: As your eye heals, you may experience changes in vision. While these fluctuations can stabilize over time, they may require adjustments in your care. Remember, it’s perfectly normal to have questions during this process.
We are here to help you through this journey, ensuring you have the support and information you need.
Conclusion
Keratoprosthesis offers a beacon of hope for those grappling with severe corneal disease, especially when traditional corneal transplants haven’t worked. This innovative surgical procedure replaces a damaged cornea with an artificial lens, paving the way for improved vision and a better quality of life for those facing corneal blindness.
We understand that considering such a procedure can be daunting. Throughout this article, we explored key aspects of keratoprosthesis, including:
- The surgical procedure
- The importance of postoperative care
- The potential risks involved
From the preoperative assessment to the careful steps of insertion and recovery, each phase is crucial for achieving the best possible outcomes. It’s common to feel concerned about risks like infection, glaucoma, and vision fluctuations, which is why diligent follow-up care and open communication with healthcare providers are so important.
Ultimately, the journey through keratoprosthesis surgery is one of resilience and hope. For those contemplating this option, staying informed and proactive in managing both the procedure and recovery is essential. Embracing this opportunity could lead to significant improvements in vision and overall well-being. Remember, with the right support and resources, regaining sight is not just a dream-it’s a possibility. We are here to help you through this process.
Frequently Asked Questions
What is a keratoprosthesis (KPro)?
A keratoprosthesis (KPro) is a surgical procedure that replaces a diseased or damaged ocular surface with an artificial lens.
Why is the cornea important?
The cornea is a clear, dome-shaped layer at the front of the eye that covers the pupil and iris, playing a vital role in eye health by maintaining fluid balance in and out of the eye.
Who can benefit from a keratoprosthesis?
Individuals with severe corneal blindness, especially those who have struggled with conventional corneal transplants or are not suitable candidates for those procedures, can benefit from a keratoprosthesis.
What is the Boston artificial cornea?
The Boston artificial cornea is one of the most commonly used types of keratoprosthesis, featuring a central optic held within a cylindrical frame that allows light to pass through while providing structural support to the eye.
How can patients feel supported during the keratoprosthesis process?
Patients are encouraged to stay informed and supported throughout the keratoprosthesis process, with assistance provided to help them understand each step.
List of Sources
- Outline the Procedure: Steps Involved in Keratoprosthesis Surgery
- Retention Of The Boston Keratoprosthesis Type 1: Multicenter Study Results – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC3674188)
- Visual outcomes of primary keratoprosthesis implantation in transplant-naïve eyes – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11449357)
- Outcomes of Boston Keratoprosthesis Type I Implantation in Poland: A Retrospective Study on 118 Patients (https://mdpi.com/2077-0383/13/4/975)
- Long-term outcomes of the Boston keratoprosthesis: a 15-year follow-up (https://canadianjournalofophthalmology.ca/article/S0008-4182(25)00362-X/fulltext)
- The Boston Keratoprosthesis (https://crstoday.com/articles/2009-sep/crst0909_16-php)
- Detail Recovery: Post-Operative Care and Expectations
- missourieye.com (https://missourieye.com/blog/considering-vision-correction-these-6-patient-quotes-may-surprise-you)
- Clinical Outcomes and Early Postoperative Complications in Boston Type I Keratoprosthesis Implantation: A Retrospective Study – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11595152)
- Ten-Year Outcome of Boston Type I Keratoprosthesis Surgery at a Tertiary Care Center – PubMed (https://pubmed.ncbi.nlm.nih.gov/38305331)
- Longer-Term Vision Outcomes and Complications with the Boston Type 1 Keratoprosthesis at the University of California, Davis (https://sciencedirect.com/science/article/abs/pii/S0161642010013850)
- Post-operative outcomes associated with Boston type 1 keratoprosthesis implantation in Northeast China – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC6307462)
- Discuss Risks: Understanding Potential Complications of Keratoprosthesis
- Glaucoma Risk Factors and Outcomes Following Boston Keratoprosthesis Type 1 Surgery – PubMed (https://pubmed.ncbi.nlm.nih.gov/33493469)
- Endophthalmitis After Keratoprosthesis (https://jamanetwork.com/journals/jamaophthalmology/fullarticle/265908)
- Glaucoma Outcomes Following Boston Keratoprosthesis Type 1 Surgery | IOVS | ARVO Journals (https://iovs.arvojournals.org/article.aspx?articleid=2768132)
- Long-term outcomes of the Boston keratoprosthesis: a 15-year follow-up (https://canadianjournalofophthalmology.ca/article/S0008-4182(25)00362-X/fulltext)
- Long-term Outcomes of Boston Type I Keratoprosthesis, and Efficacy of Amphotericin B and Povidone-Iodine in Infection Prophylaxis (https://sciencedirect.com/science/article/pii/S0002939421003159)






