Posted by: Northwest Eye in General on January 10, 2026
Introduction
Facing retinal detachment surgery can be overwhelming, and it’s completely normal to feel anxious about it. The thought of potential vision loss can weigh heavily on anyone. That’s why understanding the surgical process is so important. Timely intervention and knowledge can truly make a difference in your outcomes.
As you navigate through the complexities of diagnosis, surgical options, and post-operative care, you might have many questions. What steps can you take to ensure a successful recovery? How can you achieve the best visual results? We understand that these concerns are significant, and we’re here to help you through this process.
This guide will explore the essential aspects of retinal detachment surgery, offering clarity and support as you embark on this challenging journey. Remember, you’re not alone in this; many have walked this path and found their way to recovery. Let’s take this journey together.
Define Retinal Detachment and Its Implications
When the thin tissue at the back of your eye pulls away from its usual spot, it can lead to a condition known as retinal detachment. We understand that this can be alarming, and it’s important to know that if not treated promptly, it can result in permanent vision loss. Common causes include:
- Aging
- Trauma
- Certain eye diseases
It’s common to feel anxious when experiencing these signs, but timely intervention is crucial. Understanding their implications through retinal detachment surgery can significantly improve outcomes and help preserve your vision.
We are here to help you through this process. Remember, you’re not alone in this journey, and seeking care as soon as possible can make a world of difference.
Explore Diagnostic Techniques for Retinal Detachment
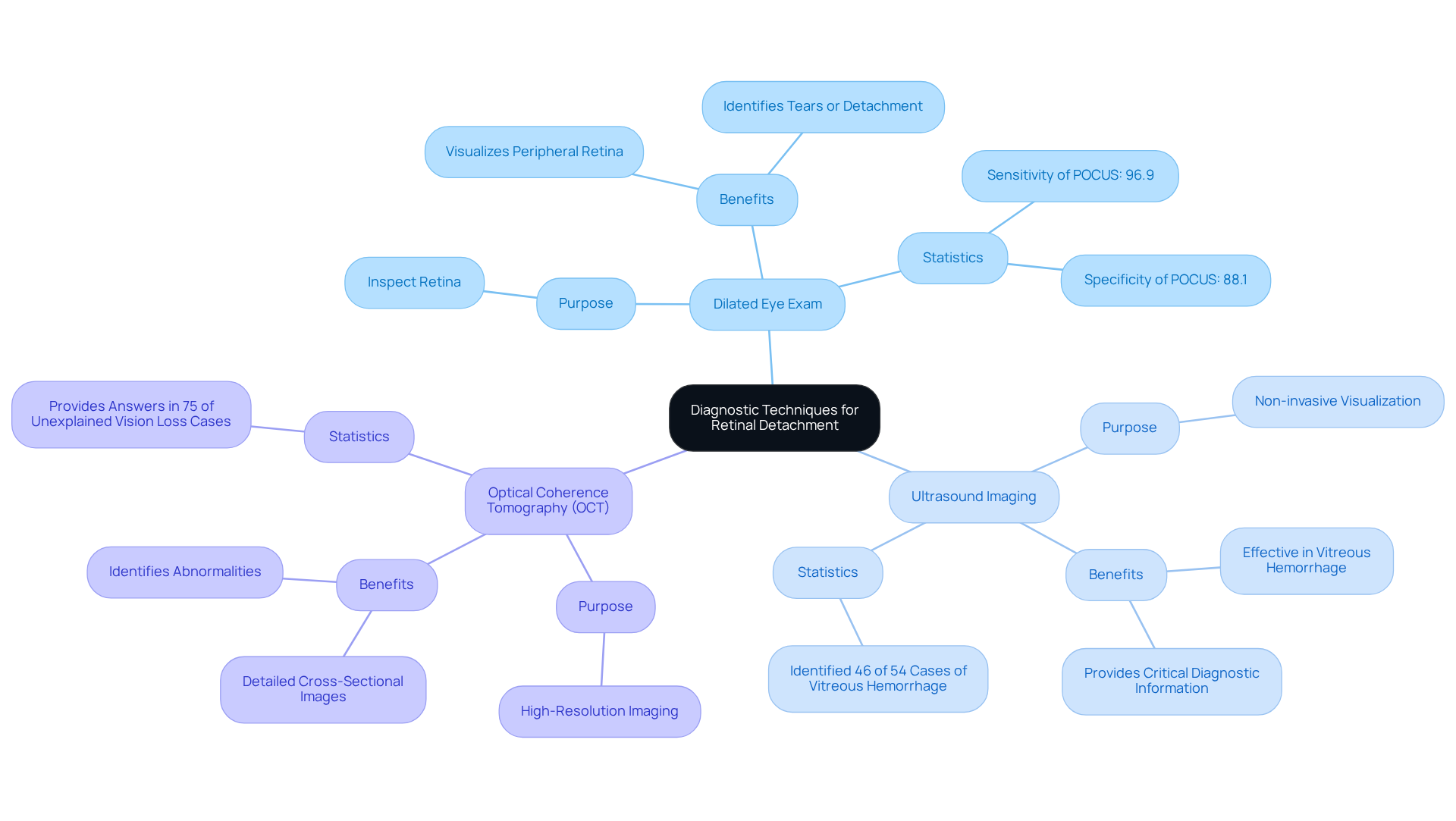
can feel overwhelming, but we’re here to help you through this process. A thorough eye examination using diagnostic tools is essential for understanding your condition and ensuring the best care.
- visualizing the peripheral part of your eye We understand that the thought of eye drops can be daunting. However, these drops widen your pupil, allowing ophthalmologists to closely inspect your retina for any signs of tears or detachment. This method is crucial for early detection and timely intervention, where many detachments occur.
- Optical Coherence Tomography (OCT) If direct inspection of your eye’s interior is challenging, such as in cases of vitreous hemorrhage, OCT is a non-invasive option. It effectively visualizes eye structures, providing critical information for diagnosis and peace of mind.
- advanced techniques This high-resolution imaging technique offers detailed cross-sectional images of your eye’s interior. It allows for precise evaluation of layers and any abnormalities. With its unparalleled sensitivity, OCT has become a standard in Ultrasound Imaging, with studies showing it can provide answers in unexplained vision loss cases 75% of the time.
These diagnostic tools are vital for a [[Dilated Eye Exam](https://nweyeclinic.com/eye-exam)](https://nweyeclinic.com/eye-exam), significantly reducing the risk of permanent vision loss. It’s common to feel anxious about these procedures, but current statistics indicate that point-of-care ultrasonography (POCUS) has a sensitivity of 96.9% for identifying eye separation. This underscores its effectiveness in emergency settings.
By integrating these techniques into clinical practice, we enhance overall diagnostic accuracy and improve patient outcomes. Remember, we are here to support you every step of the way.
Detail Surgical Procedures for Retinal Detachment
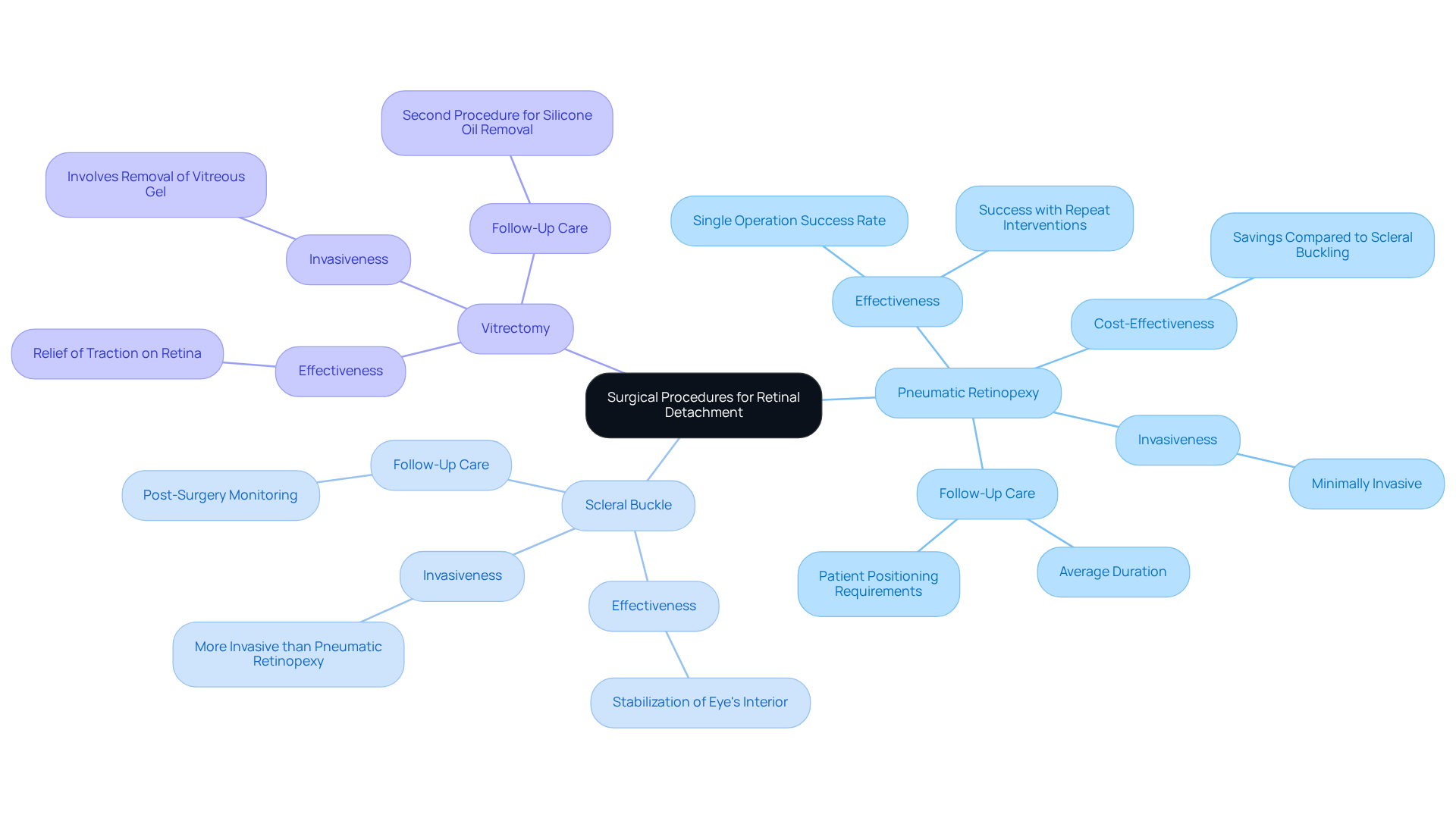
When it comes to average duration of 15 months, several surgical techniques are available, each designed with your specific needs in mind. We understand that facing such a condition can be daunting, and we’re here to guide you through your options.
- [[Pneumatic Retinopexy](https://retinatoday.com/articles/2010-jan-feb/happy-25th-pneumatic-retinopexy)](https://retinatoday.com/articles/2010-jan-feb/happy-25th-pneumatic-retinopexy): This minimally invasive procedure involves injecting a gas bubble into your eye. This bubble gently floats to the detached area, pressing the retina back into place. It’s particularly effective for smaller detachments, boasting a remarkable single-operation success rate of nearly 97%. In fact, studies show that 54% of cases succeed with just one pneumatic retinopexy, while 66% achieve success with repeat interventions. Importantly, if this procedure doesn’t work the first time, it doesn’t diminish your eye’s potential for good vision, making it a great first-line treatment. Plus, it can save you nearly 75% in treatment costs compared to scleral buckling, which is a significant advantage.
- Scleral Buckle: In this method, a silicone band is placed around your eye to gently push the wall toward the light-sensitive tissue, effectively closing the tear. This technique has been shown to stabilize the eye’s interior and is often used alongside gas injection to ensure everything is positioned just right. While the outcomes for scleral buckle surgery are generally positive, it is more invasive than pneumatic retinopexy.
- Vitrectomy: This procedure involves removing the vitreous gel to relieve traction on the retina, followed by reattachment using various techniques. While vitrectomy can be effective, it may require a second procedure to remove silicone oil used during the surgery. The decision regarding retina detachment surgery is made after a thorough evaluation, considering factors like the severity of the separation and the number of breaks in the retina.
Each surgical option, such as pneumatic retinopexy, has its own unique advantages and considerations. The decision is made collaboratively between you and your ophthalmologist, ensuring that the chosen approach aligns with your specific needs and circumstances. Follow-up care is crucial, with an average duration of 15 months reported for patients. This highlights the importance of monitoring your outcomes post-surgery. Remember, we are here to help you through this process, and we’ll support you every step of the way.
Outline Post-Operative Care and Recovery Expectations
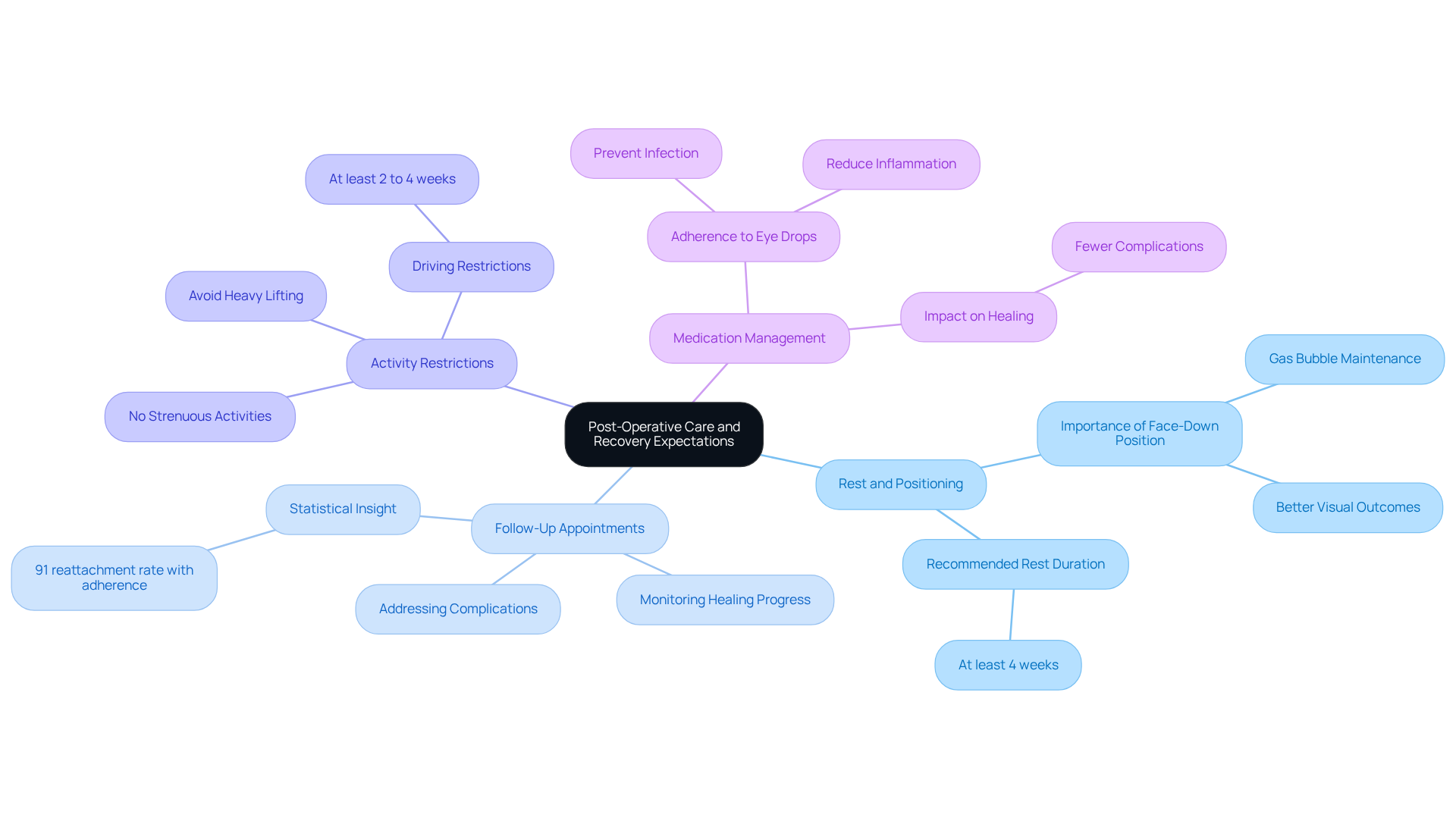
Post-operative care is vital for a successful recovery following retina detachment surgery. We understand that this can be a challenging time, and we’re here to support you through it. Key components of your recovery include:
- Rest and Positioning: Maintaining a specific head position, often face down, is crucial for ensuring that any gas bubble injected during surgery remains in place. This helps facilitate the reattachment of the retina. Research shows that patients who adhere to this positioning experience better visual outcomes and fewer complications. With a success rate for retina detachment surgery of around 90%, it is essential to follow these guidelines for your recovery.
- Follow-Up Appointments: Regular check-ups are essential for monitoring your healing progress and addressing any complications. It’s common to feel anxious about your recovery, but studies indicate that nearly 35.3% of patients in the face-down group experienced retinal displacement at six months. This highlights the necessity for ongoing evaluations. Moreover, patients who diligently follow post-operative care instructions have a 91% reattachment rate, reinforcing the importance of sticking to your care protocols.
- [[[Activity Restrictions](https://midatlanticretina.com/2023/07/10/retinal-detachment-surgery-recovery)](https://midatlanticretina.com/2023/07/10/retinal-detachment-surgery-recovery)](https://midatlanticretina.com/2023/07/10/retinal-detachment-surgery-recovery): We recommend refraining from heavy lifting, strenuous activities, and driving for at least 2 to 4 weeks post-surgery. This precaution helps prevent strain on your eye and supports the healing process.
- Medication Management: Adhering to prescribed eye drops and medications is critical for preventing infection and reducing inflammation. Patients who follow their medication regimen tend to heal better and face fewer complications. It’s important to be aware of potential complications during recovery, such as infection and inflammation, which can impact your healing.
Understanding these guidelines is essential for optimizing your recovery and achieving the best possible visual outcomes. Many patients notice improvements in vision within two to four weeks, but the average recovery time for retina detachment surgery typically ranges from 3 to 8 weeks. Remember, patience and adherence to care protocols are key to your healing journey.
Conclusion
Understanding retinal detachment and the surgical interventions available can significantly influence outcomes and preserve vision. We know that facing such a condition can be overwhelming, but this article has explored the critical aspects of retinal detachment, from its definition and implications to the diagnostic techniques, surgical procedures, and post-operative care necessary for recovery. Recognizing the urgency of this condition and the steps involved in treatment empowers you to seek timely care and make informed decisions about your health.
Key insights discussed include:
- The importance of early diagnosis through advanced imaging techniques like OCT and ultrasound, which enhance the accuracy of detecting retinal detachment.
- It’s common to feel anxious about the unknown, but understanding these options can help ease your concerns.
- Various surgical options, such as pneumatic retinopexy, scleral buckle, and vitrectomy, each offering unique benefits tailored to individual needs.
- Post-operative care, including positioning, follow-up appointments, and medication management, is crucial for ensuring successful recovery and optimal visual outcomes.
Ultimately, understanding the process of retinal detachment surgery and adhering to post-operative guidelines can lead to a smoother recovery and better long-term vision. We encourage you to remain proactive in recognizing symptoms and seeking medical advice promptly. By doing so, you can take charge of your eye health and work towards preventing the potentially devastating effects of retinal detachment. Remember, we are here to help you through this process.
Frequently Asked Questions
What is retinal detachment?
Retinal detachment is a condition that occurs when the thin tissue at the back of the eye pulls away from its usual position.
What are the implications of retinal detachment?
If not treated promptly, retinal detachment can lead to permanent vision loss.
What are common causes of retinal detachment?
Common causes include aging, trauma, and certain eye diseases.
What symptoms might indicate retinal detachment?
Symptoms include sudden flashes of light, floaters, and a shadow over your visual field.
What should I do if I experience symptoms of retinal detachment?
It is crucial to seek care as soon as possible, as timely intervention through retina detachment surgery can significantly improve outcomes and help preserve vision.
List of Sources
- Define Retinal Detachment and Its Implications
- Retinal Detachment Can Steal Your Sight—Here’s How to Catch It Early (https://yalemedicine.org/news/retinal-detachment-can-steal-your-sight-heres-how-to-catch-it-early)
- Retinal Detachment – Symptoms, Causes & Treatment | Lions Eye Institute (https://lei.org.au/services/eye-health-information/retinal-detachment)
- Demographics and Seasonality of Retinal Detachment, Retinal Breaks, and Posterior Vitreous Detachment from the Intelligent Research in Sight Registry – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9559074)
- mayoclinic.org (https://mayoclinic.org/diseases-conditions/retinal-detachment/symptoms-causes/syc-20351344)
- nei.nih.gov (https://nei.nih.gov/eye-health-information/eye-conditions-and-diseases/retinal-detachment)
- Explore Diagnostic Techniques for Retinal Detachment
- Optical Coherence Tomography in Retinal Detachment: Prognostic Biomarkers, Surgical Planning, and Postoperative Monitoring – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11988441)
- Retina experts reflect on how OCT transformed patient care | Ophthalmology Times – Clinical Insights for Eye Specialists (https://ophthalmologytimes.com/view/retina-experts-reflect-on-how-oct-transformed-patient-care)
- Point-of-Care Ultrasonography in Ophthalmologic Diagnosis in the Emergency Department (https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2730478)
- Retinal detachment – Diagnosis and treatment – Mayo Clinic (https://mayoclinic.org/diseases-conditions/retinal-detachment/diagnosis-treatment/drc-20351348)
- Recent Optical Coherence Tomography (OCT) Innovations for Increased Accessibility and Remote Surveillance – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12108957)
- Detail Surgical Procedures for Retinal Detachment
- Happy 25th, Pneumatic Retinopexy – Retina Today (https://retinatoday.com/articles/2010-jan-feb/happy-25th-pneumatic-retinopexy)
- Pneumatic Retinopexy: Failure, 360º Laser, Pseudophakes (https://retinalphysician.com/issues/2014/september/pneumatic-retinopexy-failure-360186-laser-pseudophakes)
- Pneumatic retinopexy: success rate and complications – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC1857020)
- Learning About Retinal Detachment Surgery | Kaiser Permanente (https://healthy.kaiserpermanente.org/health-wellness/health-encyclopedia/he.learning-about-retinal-detachment-surgery.abp2669)
- Outline Post-Operative Care and Recovery Expectations
- prasadnetralaya.com (https://prasadnetralaya.com/care-your-eyes-after-retinal-detachment-surgery)
- Positioning After Retinal Surgery (https://aao.org/eye-health/treatments/face-down-recovery-after-retinal-surgery)
- 5 Essential Steps for Detached Retina Recovery Success | Northwest Eye (https://nweyeclinic.com/5-essential-steps-for-detached-retina-recovery-success)
- Retinal Detachment Surgery Recovery, Retina Surgery Recovery (https://midatlanticretina.com/2023/07/10/retinal-detachment-surgery-recovery)
- dmei.org (https://dmei.org/blog/life-after-retinal-detachment-surgery)






