Posted by: Northwest Eye in General on January 10, 2026
Introduction
Understanding eye edema is crucial for anyone concerned about their vision and overall eye health. We understand that noticing swelling in your eyes can be alarming, and it’s important to address these feelings. This condition, characterized by the swelling of eye tissues due to fluid accumulation, can manifest in various forms, each with unique causes and symptoms.
By exploring the types of eye edema, their underlying factors, and effective treatment options, you can gain valuable insights to manage your eye health proactively. It’s common to feel overwhelmed by medical information, but we’re here to help you through this process. However, the journey to understanding eye edema raises an important question: how can one differentiate between the types and effectively address the symptoms before they lead to more serious complications?
Let’s take this step together, ensuring you feel supported and informed every step of the way.
Define Eye Edema and Its Types
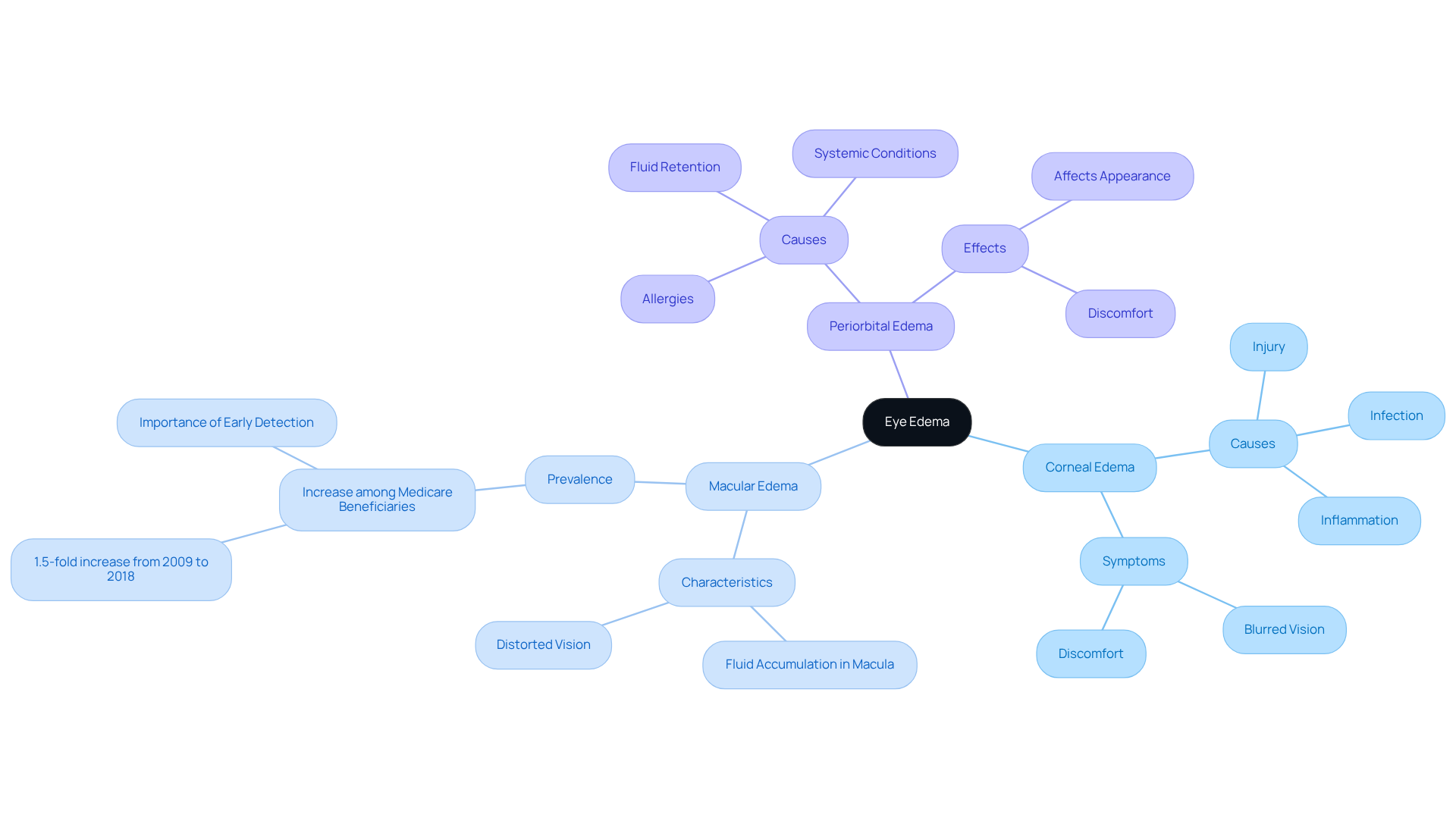
is characterized by the swelling of eye tissues as a result of fluid accumulation, and it can present itself in various forms. We understand that experiencing eye problems can be concerning, and it’s important to know what you’re dealing with.
- diabetic macular edema (DME) This condition involves swelling of the cornea, often resulting from injury, infection, or inflammation. It can lead to blurred vision and discomfort, which can be quite distressing.
- timely intervention Characterized by fluid accumulation in the macula, this type can distort vision and potentially lead to significant vision loss if not addressed promptly. Recent studies show that the prevalence of diabetic macular edema among Medicare beneficiaries has increased significantly, highlighting the importance of early detection and management.
- Periorbital Edema This type involves swelling around the eyes, commonly caused by allergies, infections, or other systemic conditions. It can affect your appearance and may come with discomfort, which is understandably frustrating.
Comprehending these types of eye edema is essential for identifying symptoms and pursuing treatment. We want you to know that timely intervention can prevent complications and preserve your vision. Awareness of these conditions is crucial for maintaining your eye health, and we are here to help you through this process.
Identify Causes of Eye Edema
Eye edema can arise from a variety of causes, each requiring careful consideration for effective management and treatment:
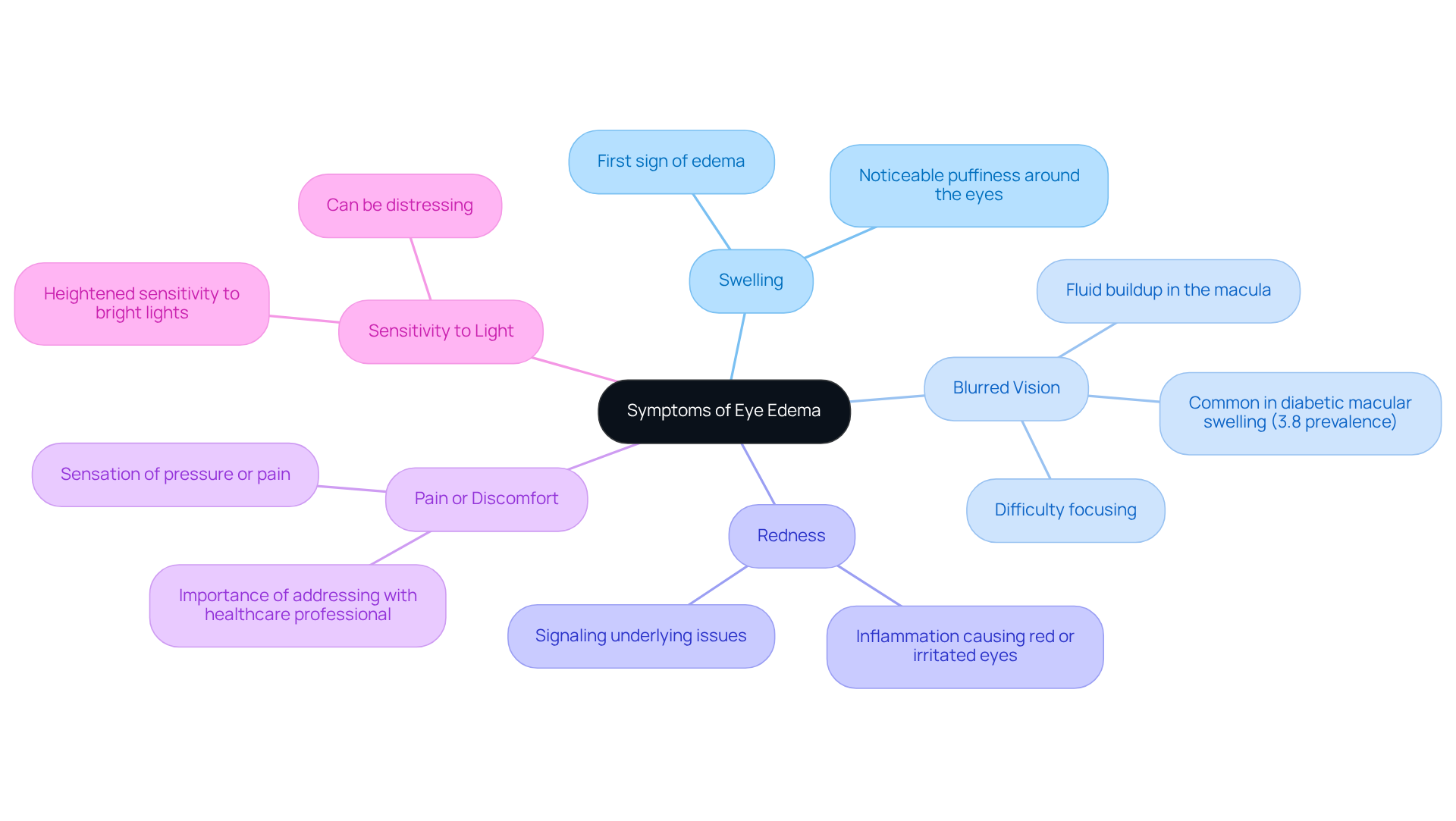
- Allergic Reactions: Common allergens such as pollen, dust, and pet dander can trigger significant swelling around the eyes. Approximately 40% of North Americans experience some form of allergic eye disease, which can lead to noticeable periorbital edema. Antihistamines and cold compresses may help alleviate symptoms.
- Infections: Both bacterial and viral infections are known to cause inflammation and edema. For instance, conjunctivitis, often referred to as “pink eye,” can lead to puffy and red eyelids due to the inflammation that makes blood vessels more visible. This condition can be highly contagious, emphasizing the importance of proper infection control practices. The prevalence of infectious eye diseases is significant, particularly among children and working-age individuals, highlighting the need for awareness and preventive measures. Symptoms that persist beyond 48 hours should prompt a medical evaluation.
- Injury: Trauma to the eye, whether from a direct blow or a foreign object, can result in localized swelling. Immediate evaluation is crucial to assess potential damage and determine appropriate treatment.
- Surgical Procedures: Post-operative inflammation is a common occurrence, especially following cataract surgery, where the incidence of eye swelling has been recorded at around 9.17%. Understanding this risk can help patients prepare for recovery.
- Medical Conditions: Systemic health issues, such as diabetes and thyroid disorders, can contribute to fluid retention around the eyes. Conditions like Graves’ disease may lead to periorbital edema, emphasizing the importance of managing underlying health problems. Additionally, certain medications, including blood pressure medications and corticosteroids, can cause eyelid swelling as a side effect.
- Lifestyle Factors: Factors such as excessive salt consumption and lack of sleep can exacerbate persistent eye swelling. Maintaining a balanced diet and ensuring adequate rest can help mitigate these effects.
Recognizing these causes is essential for timely intervention and effective treatment strategies.
Understand Diagnostic Procedures for Eye Edema
Diagnosing eye edema can feel overwhelming, but understanding the process can help ease your concerns. It involves a series of important procedures designed to ensure accurate identification and effective treatment planning. Here are some key diagnostic methods:
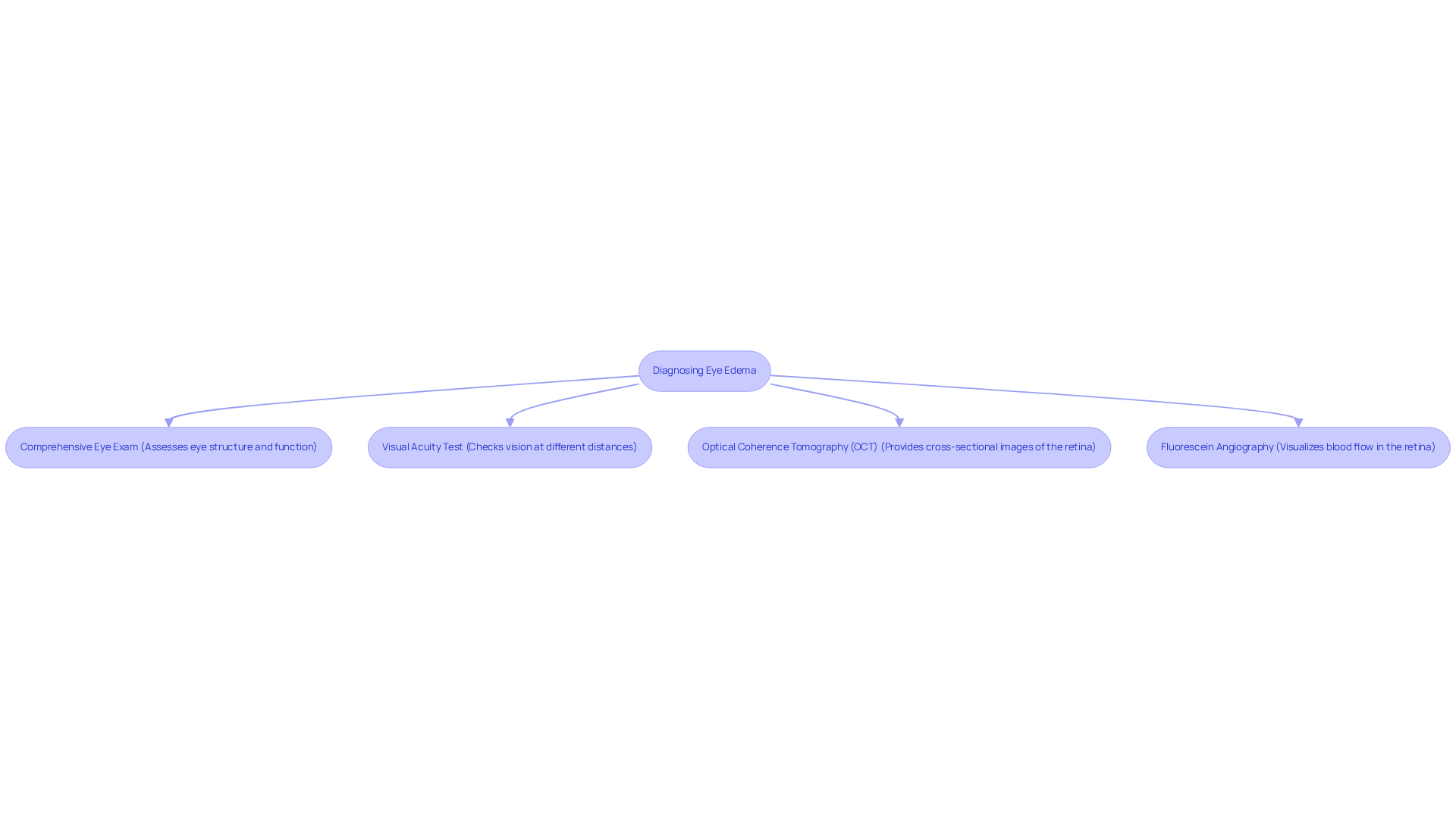
- Optical Coherence Tomography (OCT) This thorough examination assesses the eye’s structure and function, helping to identify any underlying conditions that may contribute to swelling.
- Visual Acuity Test This test checks how well you can see at different distances, providing crucial insights into how swelling might be affecting your vision.
- Fluorescein Angiography As a non-invasive imaging method, OCT gives cross-sectional images of the retina. It’s essential for diagnosing eye edema, as it reveals the degree of fluid buildup and the presence of cysts, which are vital for deciding on care options.
- Comprehensive Eye Exam This procedure involves injecting a special dye to visualize blood flow in the retina, helping to identify leaks associated with swelling. It’s particularly useful for assessing the severity of the condition and guiding further interventions.
These diagnostic tools are crucial for developing a lasting treatment plan. Research shows that OCT can effectively identify issues, allowing for prompt action that can prevent irreversible damage to the macula. Eye edema can lead to vision loss if not addressed, underscoring the importance of Visual Acuity Test. Additionally, diagnostic procedures play a vital role in identifying co-morbidities that may complicate treatment, ensuring you receive holistic care.
As noted by William C Lloyd III, “Eye edema can lead to temporary vision changes and improve over time, but in certain instances, it can be quite severe.” We understand that this can be a lot to take in, but rest assured that the incorporation of these advanced diagnostic methods reflects the latest progress in eye care, enhancing our ability to manage eye swelling effectively. We are here to help you through this process.
Explore Treatment Options for Eye Edema
If you’re dealing with eye edema and consulting with an ophthalmologist, it’s entirely understandable to feel concerned. Treatment can vary based on the underlying cause, and we want to help you navigate this journey with care. Here are some common approaches:
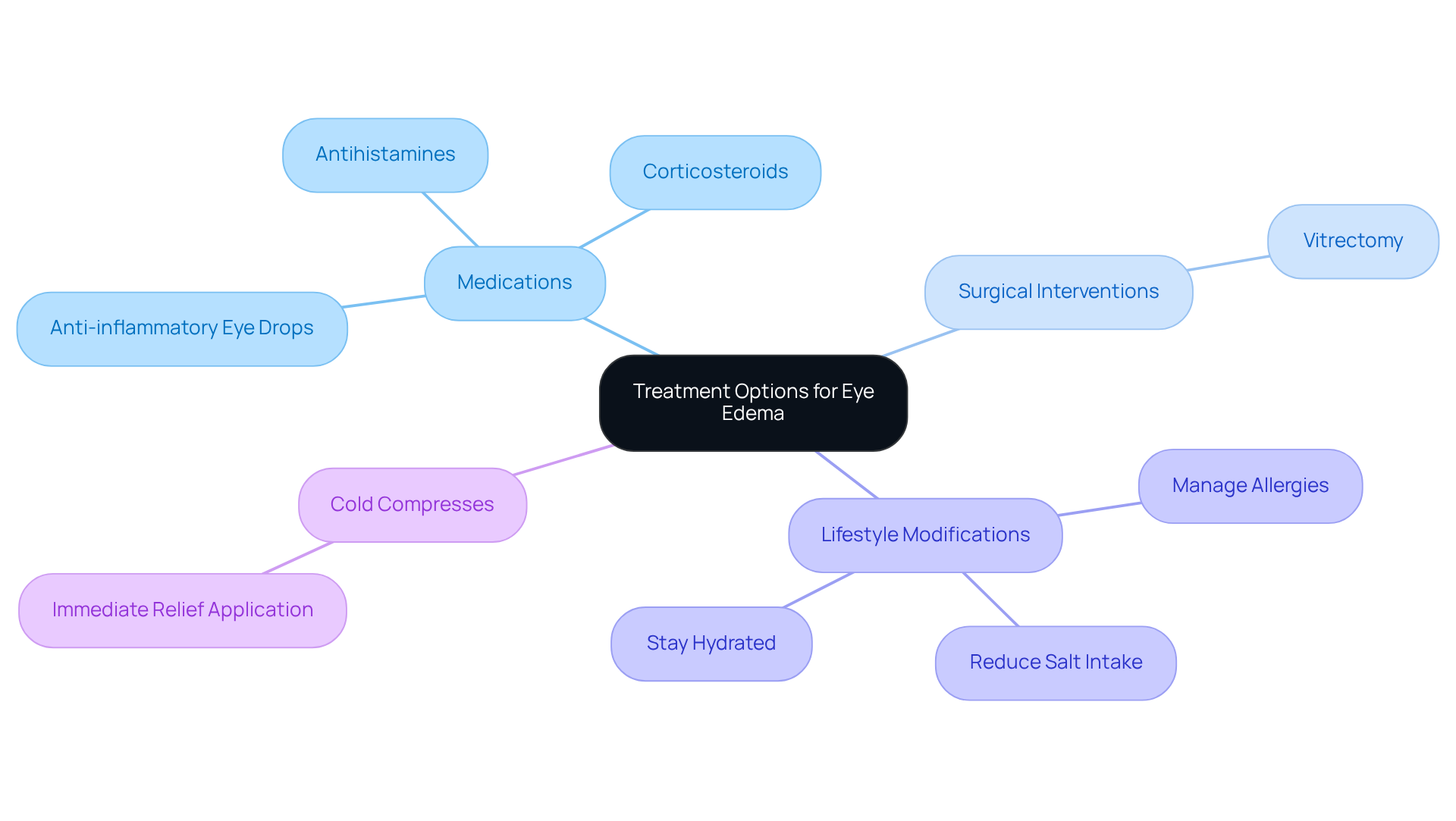
- Medications: corticosteroids or antihistamines can help reduce swelling and inflammation.
- Anti-inflammatory eye drops: In more severe cases, procedures like vitrectomy may be necessary to address eye issues.
- Lifestyle modifications: Simple changes, such as reducing salt intake, staying hydrated, and managing allergies, can make a significant difference in treatment outcomes.
- Preventing swelling: Applying a cold compress can provide immediate relief from macular swelling, offering you some comfort.
We understand that seeking treatment can feel overwhelming, but follow-up care is crucial for determining the most suitable care plan for you. Remember, you’re not alone in this – we are here to help you through this process.
Implement Follow-Up Care and Monitoring
Follow-up care is critical in managing eye edema effectively. Key components include:
- Regular Eye Exams: Schedule follow-up appointments with your Northwest Eye specialist to monitor progress and adjust treatment as necessary. This is especially important for cataract patients who may experience changes in vision.
- Symptom Tracking: Keep a log of any changes in symptoms, such as blurred vision, which can be associated with conditions like cataracts, diabetic retinopathy, or macular degeneration. Discuss these changes with your ophthalmologist to aid in diagnosing underlying conditions.
- Adherence to Treatment Plans: Follow prescribed medications and lifestyle recommendations to optimize recovery. Being informed about your treatment options, including innovative solutions like the Light Adjustable Lens, can empower your health decisions.
- Patient Education: Stay informed about your condition and treatment options to make informed health choices. Northwest Eye encourages you to learn about common eye symptoms and their associations with various conditions, as this knowledge can significantly impact your eye health.
Consistent follow-up care can significantly improve outcomes and prevent complications.






