Posted by: Northwest Eye in General on February 12, 2026
Introduction
After undergoing retinal detachment surgery, we understand that you may find yourself navigating a complex and emotional recovery journey. It’s common to feel overwhelmed by the recovery timeline and the importance of following post-operative care instructions. These factors can significantly impact your healing process and visual outcomes.
You might have questions about managing discomfort, maintaining proper positioning, and the necessity of follow-up appointments. How can you ensure a smooth recovery while addressing these concerns? This guide is here to help you through this process, delving into essential steps and strategies to facilitate optimal healing and restore your vision effectively.
Understand the Recovery Timeline After Retinal Detachment Surgery
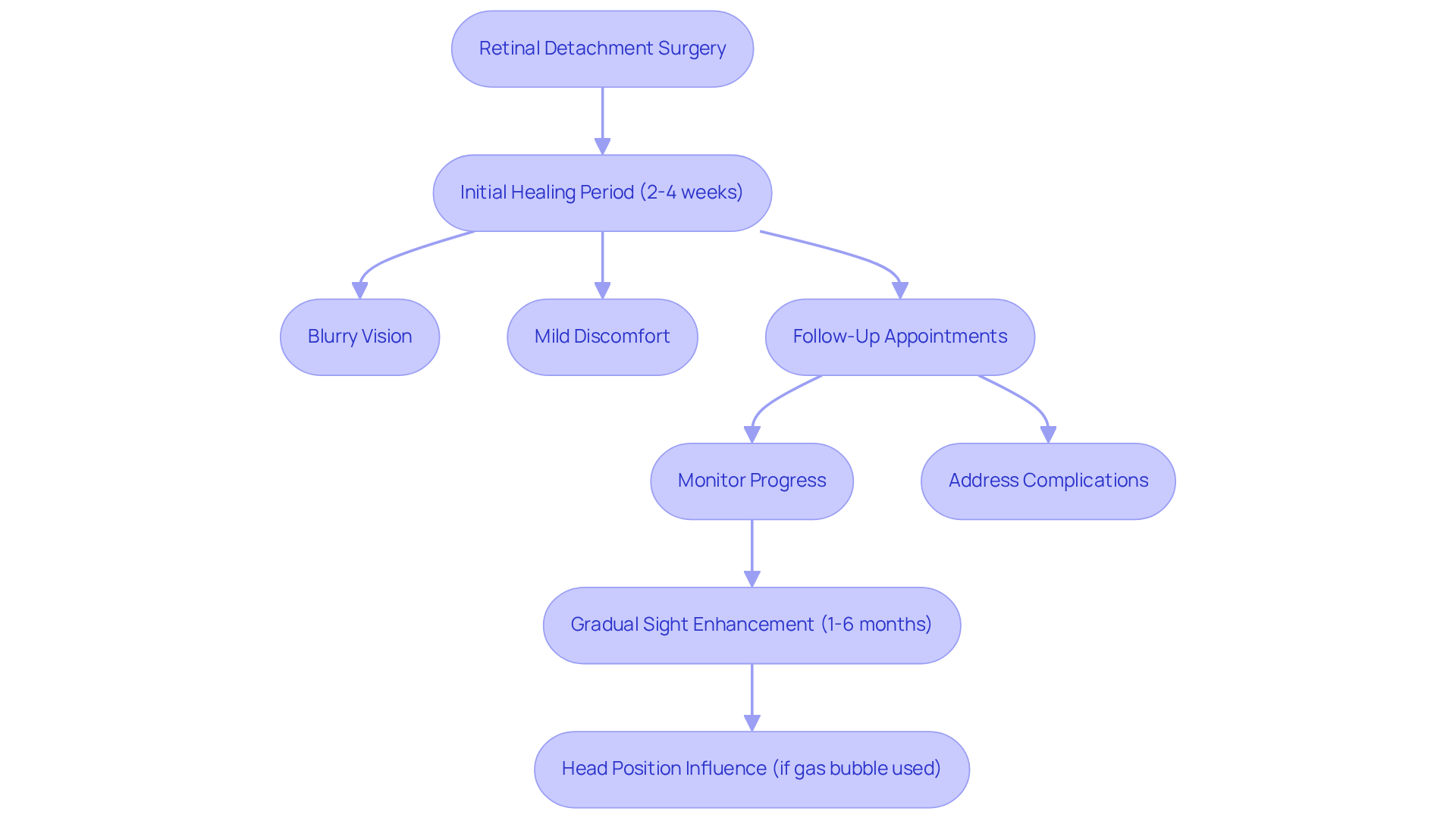
After regular [follow-up appointments](https://nweyeclinic.com/?p=7880) with your ophthalmologist, we understand that you may be feeling a mix of emotions. It’s common to experience an improvement during gradual sight enhancement over 1 to 6 months, during which blurry vision and discomfort can arise. These symptoms might stem from various conditions, including:
- nearsightedness
- farsightedness
As your eye begins to heal, some people notice improvements in their eyesight within just a few weeks. However, the process of recovery can take several months, depending on the severity of the detachment and the surgical technique used.
If a gas bubble was utilized during your procedure, it’s essential to maintain a specific position for optimal healing. This can influence your overall timeline. Follow-up appointments are crucial. They help monitor your progress, like infection or inflammation, and adjust your care as needed.
We want to reassure you that recovery experiences can vary. For instance, patients who undergo vitrectomy often see different results, depending on their unique situations. Understanding these timelines and adhering to post-operative care guidelines is vital for optimal recovery. If you notice any drastic changes or ongoing vision problems, please don’t hesitate to reach out. Your ophthalmologist can significantly improve your outcomes.
Follow Post-Operative Care Instructions Carefully
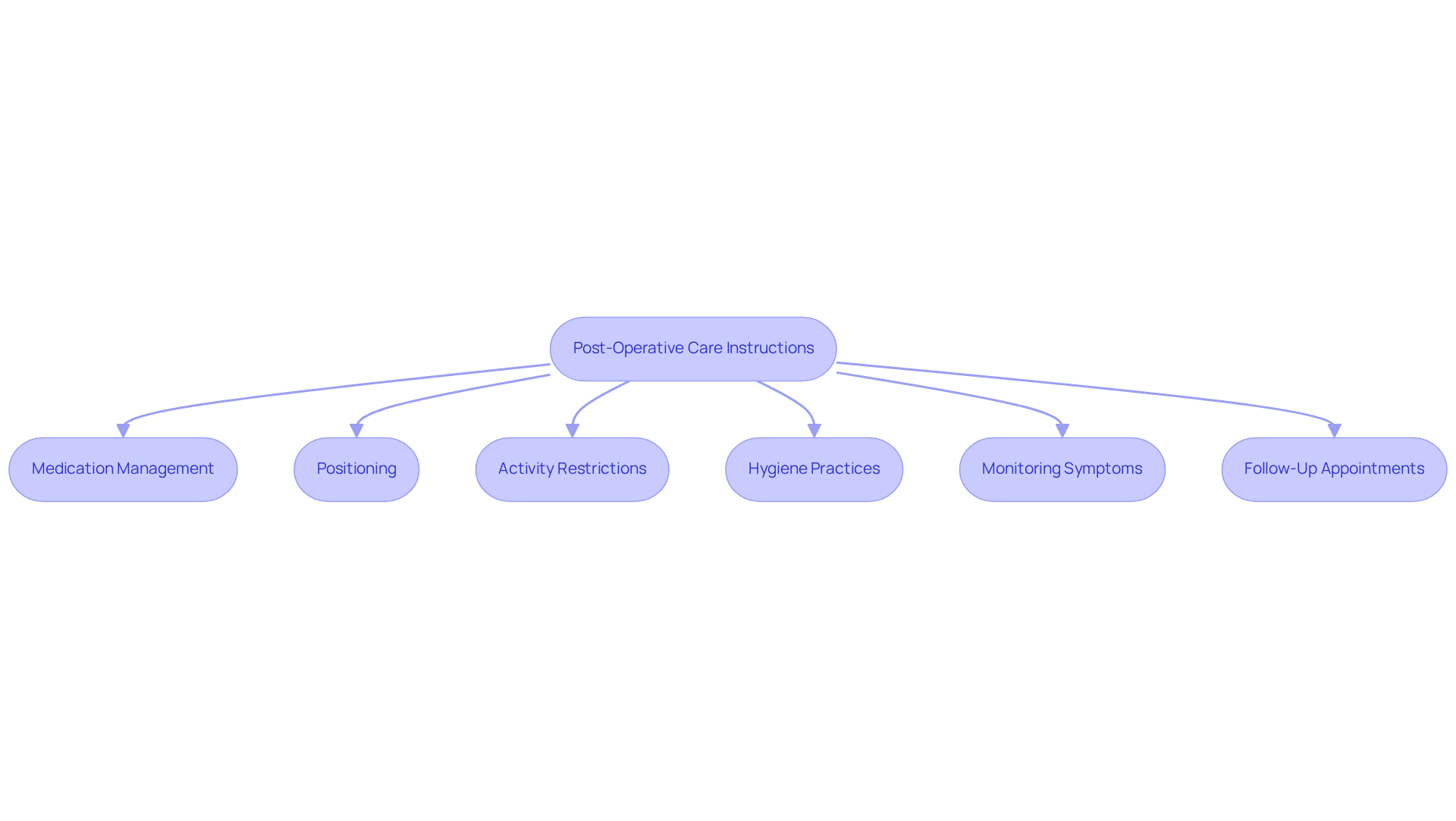
To ensure a smooth recovery after retinal detachment surgery, it’s crucial to follow your ophthalmologist’s post-operative care guidelines closely. We understand that this can be a challenging time, and we’re here to help you through it. Here are some key strategies to keep in mind:
- Medication Management: It’s important to stick to the prescribed regimen for antibiotics and anti-inflammatory eye drops. This helps prevent infection and reduces swelling. Remember to wait 5-10 minutes between different eye drops for the best results. Following these guidelines is vital, as modern surgical techniques have lowered infection risks to less than 1% when adhered to properly.
- Positioning: Maintaining the recommended head position, like face-down, is especially important if a gas bubble was used during your procedure. Incorrect positioning can lead to complications, such as the gas bubble shifting away from the treatment area, which is essential for optimal healing.
- Activity Restrictions: It’s common to feel eager to return to your normal routine, but please refrain from strenuous activities, heavy lifting, and bending over for at least two weeks after surgery. These restrictions are in place to avoid unnecessary strain on your eye, which can jeopardize your recovery.
- Hygiene Practices: Keeping the eye area clean is vital. Avoid exposing it to water for the first few days. Frequent hand washing with antiseptic soap or gel is crucial during the first week after surgery to prevent infection. If needed, use a clean, damp cloth to gently clean around your eye, ensuring hygiene is maintained.
- Monitoring Symptoms: Stay alert for any signs of complications, such as increased pain, redness, or changes in your vision. Severe pain that isn’t relieved by medication, especially when accompanied by nausea, requires immediate evaluation. It’s important to report these symptoms to your doctor right away, as early intervention can prevent serious issues and protect your vision.
- Follow-Up Appointments: Regular Follow-Up Appointments with a retina specialist are essential for monitoring your progress, adjusting treatment plans, and addressing any questions you may have.
By adhering to these guidelines, you not only facilitate a smoother healing process but also significantly increase your chances of a successful outcome during your retinal detachment surgery recovery. Remember, we’re here to support you every step of the way.
Manage Discomfort and Address Common Concerns
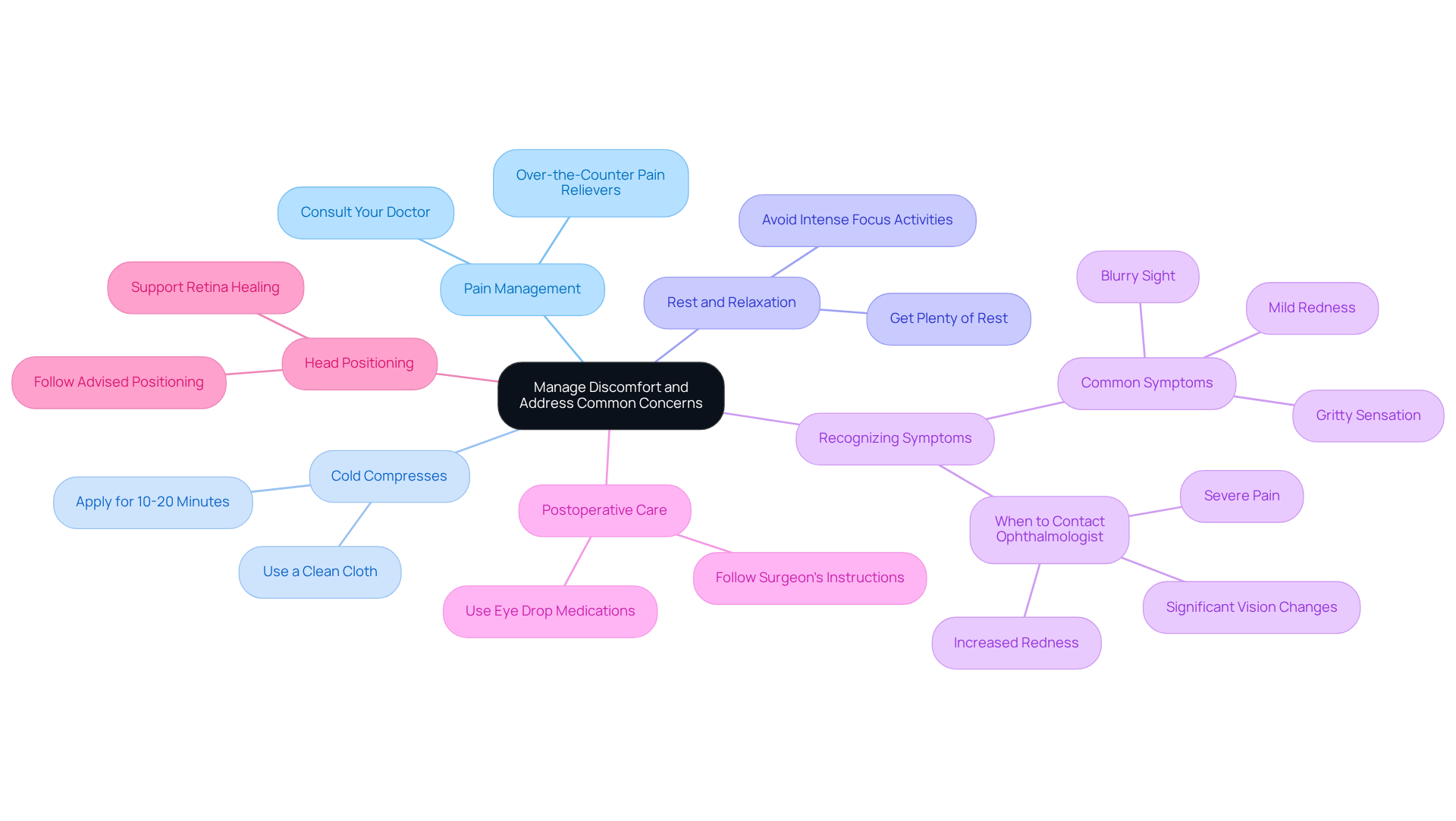
Post-operative discomfort is a normal part of the recovery process. We understand that this can be a challenging time, and we’re here to help you through it. Here are some strategies to manage discomfort and address common concerns:
- Over-the-counter pain relievers like acetaminophen or ibuprofen can help alleviate mild discomfort. Always consult your doctor before taking any medication to ensure safety and appropriateness.
- Applying a cold compress to the eye area can reduce swelling and provide relief from discomfort. Use a clean cloth and apply it for 10-20 minutes at a time.
- It’s important to get plenty of rest, as fatigue can make discomfort feel worse. Try to avoid activities that require intense focus, such as reading or using screens, especially in the first few days.
- It’s common to experience mild redness, or a gritty sensation in the eye. However, if you notice severe pain, vision loss, or increased redness, please contact your ophthalmologist immediately for guidance. Timely attention can prevent complications and ensure a smoother healing process.
- Following your surgeon’s instructions regarding eye drop medications is crucial. These drops help control inflammation and reduce the risk of infection during the first week after surgery.
- Following the advised head positioning after surgery is essential for healing. This positioning supports the retina as it heals, particularly if gas or silicone oil bubbles were used during the procedure.
Incorporating these strategies can significantly improve your healing experience during recovery and help manage discomfort effectively. Remember, we are here to support you every step of the way.
Schedule and Attend Follow-Up Appointments
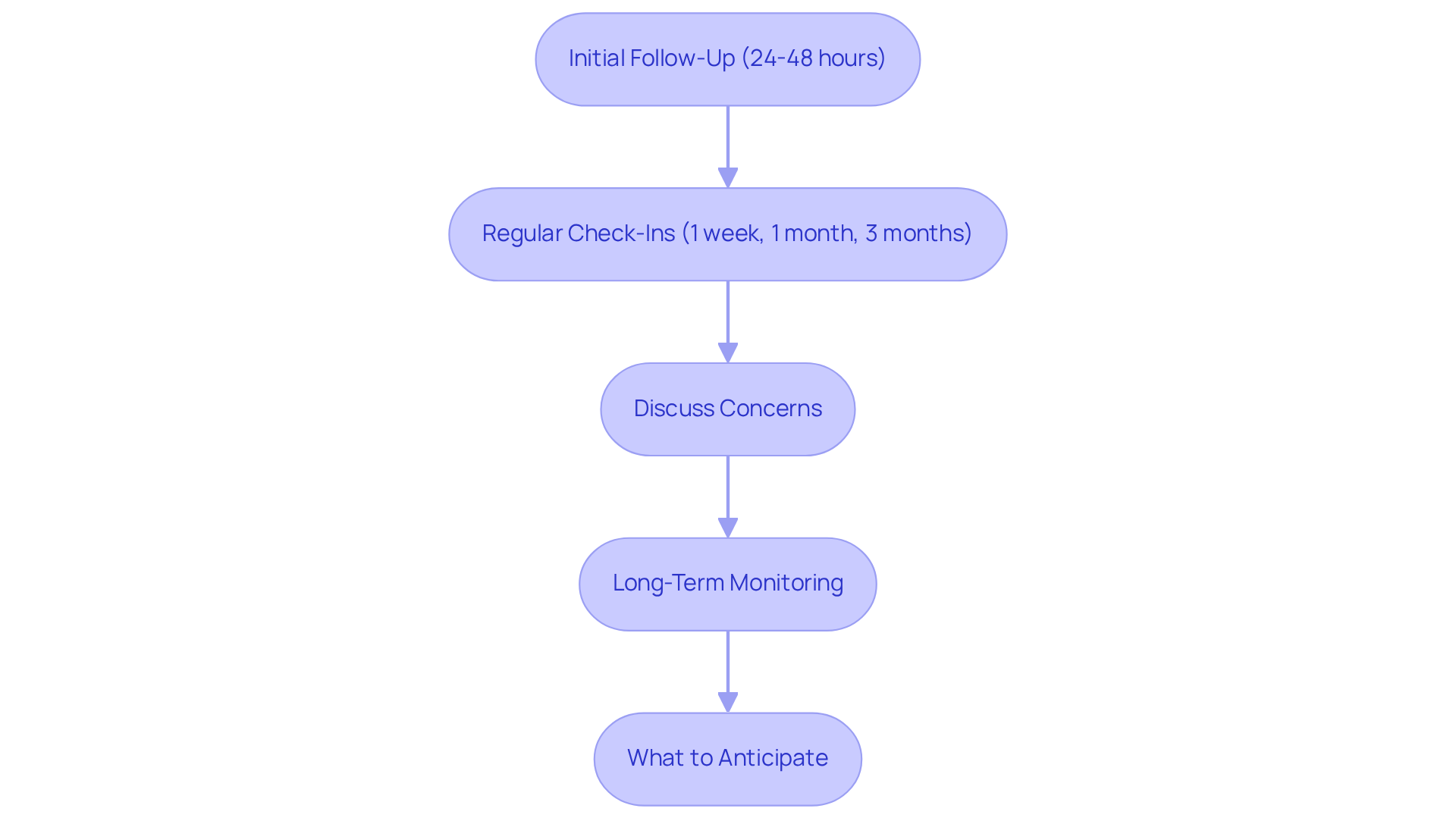
are essential for a successful recovery process. We understand that this can be a challenging time, and here’s what you should know:
- Initial Follow-Up: Schedule your first follow-up appointment within 24 to 48 hours post-surgery. This early visit allows your ophthalmologist to evaluate your healing progress and adjust your care plan as needed. It’s common to feel anxious during this time, but rest assured, this step is crucial for your recovery.
- Regular Check-Ins: Anticipate follow-up visits at one week, one month, and three months following the procedure. These appointments are vital for monitoring your condition and confirming that your retina remains securely attached throughout your retinal reattachment process, as noted in recent evaluations of 401 uncomplicated primary retinal detachment surgeries carried out in 2023. Research suggests that successful retinal detachment surgery recovery is associated with a 100% reattachment rate. Understanding this can provide some reassurance as you navigate your recovery; regular follow-up can greatly improve results.
- Discuss Concerns: Use these visits to voice any concerns or symptoms you may be experiencing. It’s important to have open dialogue with your physician, as this encourages comfort and offers direction on effectively handling your healing process. Remember, your feelings and questions are valid.
- Long-Term Monitoring: Ongoing follow-up care is essential, as some patients may need further treatments or interventions. Regular check-ins with your ophthalmologist not only safeguard your eyesight but also improve the chances of successfully monitoring your progress. As indicated by specialists, prioritizing these appointments is essential for a robust recovery. We are here to help you through this process.
- What to Anticipate: During long-term vision health management, expect to undergo evaluations and discussions about your healing process. Your doctor will monitor for any complications, such as infections or inflammation, and ensure that your treatment plan remains effective. This proactive approach is crucial for maintaining your vision, especially during follow-up appointments. Additionally, be sure to adhere to any prescribed medication instructions, including the use of eye drops, to support your recovery. Taking these steps can make a significant difference in your healing journey.
Conclusion
After undergoing retinal detachment surgery, we understand that the journey to recovery can feel overwhelming. It’s crucial to pay careful attention to various aspects of post-operative care. Knowing the recovery timeline and following the prescribed guidelines can significantly influence your healing process. By prioritizing follow-up appointments and adhering to recommended practices, you can enhance your chances of a successful outcome.
Key strategies for a smooth recovery include:
- Managing discomfort through medication and rest.
- Maintaining proper head positioning.
- Closely monitoring symptoms for any complications.
Regular communication with your healthcare providers during follow-up visits is essential. This allows for timely adjustments to treatment plans and addresses any concerns that may arise. We want you to feel reassured, and this proactive approach plays a vital role in safeguarding your vision health.
Ultimately, the path to recovery after retinal detachment surgery is a collaborative effort between you and your healthcare team. Emphasizing the importance of post-operative care and follow-up appointments empowers you to take charge of your healing journey. By embracing these essential steps, you can look forward to restoring your vision and returning to your daily activities with confidence.
Frequently Asked Questions
What is the typical initial healing period after retinal detachment surgery?
The initial healing period after retinal detachment surgery typically lasts 2 to 4 weeks.
What symptoms might I experience during the recovery period?
During the recovery period, you may experience blurry vision and mild discomfort, which can arise from conditions such as nearsightedness, farsightedness, cataracts, or diabetic retinopathy.
How long does the overall recovery process take?
The overall recovery process can take several months, depending on the severity of the detachment and the surgical technique used.
What should I do if a gas bubble was used during my surgery?
If a gas bubble was used during your procedure, it is essential to maintain a specific head position for optimal healing.
Why are follow-up appointments with my ophthalmologist important?
Regular follow-up appointments are crucial to monitor your progress, address any complications like infection or inflammation, and adjust your care as needed.
How does recovery vary among patients?
Recovery experiences can vary; for instance, patients who undergo vitrectomy may see gradual sight enhancement over 1 to 6 months, depending on their unique situations.
What should I do if I notice drastic changes or ongoing vision problems during my recovery?
If you notice any drastic changes or ongoing vision problems, it is important to reach out to your ophthalmologist, as proactive communication can significantly improve your outcomes.
List of Sources
- Understand the Recovery Timeline After Retinal Detachment Surgery
- Retinal Detachment Surgery Recovery Timeline (https://everett-hurite.com/blog/how-long-does-recovery-take-after-retinal-detachment-surgery-in-pittsburgh-pa)
- Retinal Detachment Surgery Recovery, Retina Surgery Recovery (https://midatlanticretina.com/2023/07/10/retinal-detachment-surgery-recovery)
- Surgery for Retinal Detachment: What to Expect at Home | Kaiser Permanente (https://healthy.kaiserpermanente.org/health-wellness/health-encyclopedia/he.surgery-for-retinal-detachment-what-to-expect-at-home.abp2623)
- Follow Post-Operative Care Instructions Carefully
- Face Down Recovery After Retinal Surgery – DC Retina (https://dcretina.com/article/recovery-after-retina-surgery-face-down-recovery)
- Retinal Surgery Recovery: What to Expect and How to Prepare (https://retinaconsultantsofamerica.com/blog/retinal-surgery-recovery-what-to-expect-and-how-to-prepare)
- Retinal Detachment Surgery Recovery, Retina Surgery Recovery (https://midatlanticretina.com/2023/07/10/retinal-detachment-surgery-recovery)
- Dr Donaldson – Retinal Surgery Post-Op Instructions – Terrace Eye Centre (https://terraceeyecentre.com.au/surgery-information/dr-donaldson-instructions/dr-donaldson-retinal-surgery-post-op-instructions)
- Manage Discomfort and Address Common Concerns
- Retinal Surgery Recovery: What to Expect and How to Prepare (https://retinaconsultantsofamerica.com/blog/retinal-surgery-recovery-what-to-expect-and-how-to-prepare)
- Patient Perspective: Retinal Detachment (https://hopkinsmedicine.org/news/articles/2022/04/patient-perspective-retinal-detachment)
- virginiaeyeconsultants.com (https://virginiaeyeconsultants.com/retinal-detachment-eyelid-surgery-patient-story)
- Retinal Detachment Surgery Recovery, Retina Surgery Recovery (https://midatlanticretina.com/2023/07/10/retinal-detachment-surgery-recovery)
- Schedule and Attend Follow-Up Appointments
- Patient Perspective: Retinal Detachment (https://hopkinsmedicine.org/news/articles/2022/04/patient-perspective-retinal-detachment)
- The Importance Of Follow-Up Care After Eye Surgery | Retina Associates of Orange County (https://retinaorangecounty.com/2025/09/13/the-importance-of-follow-up-care-after-eye-surgery)
- Surgery for Retinal Detachment: What to Expect at Home | Kaiser Permanente (https://healthy.kaiserpermanente.org/health-wellness/health-encyclopedia/he.surgery-for-retinal-detachment-what-to-expect-at-home.abp2623)
- Retina Surgery Outcomes | Mass Eye and Ear (https://masseyeandear.org/ophthalmology-outcomes/retina-surgery)






