Posted by: Northwest Eye in General on January 14, 2026
Introduction
Keratoconus is a progressive eye disease that can be quite challenging for those affected. It’s characterized by the thinning and bulging of the cornea, which can lead to a cone-like shape. This change distorts light, resulting in blurred vision that can significantly impact daily activities and overall quality of life.
We understand that facing such a condition can be overwhelming, especially as it becomes more prevalent among young adults. The financial burden associated with treatment is also rising, making it crucial to understand the causes, symptoms, and available interventions.
What steps can you take to recognize this condition early? It’s important to be aware of the signs and seek help promptly. Navigating the complexities of effective management can feel daunting, but you’re not alone in this journey. We are here to help you through this process.
Define Keratoconus: Understanding the Condition
is a progressive disorder of the eye that can be quite concerning. It’s characterized by the thinning and bulging of the cornea, which creates a cone-like shape that distorts how light enters the eye. This distortion often leads to recognizing its potential impact on your quality of life, making daily activities more challenging.
We understand that experiencing keratoconus can be distressing. In addition, the financial burden of treating corneal diseases is significant; this blurriness is a direct result of the changes in the cornea, which sets it apart from other vision issues like nearsightedness or astigmatism. Typically, this condition appears during adolescence or early adulthood and can progress over time, affecting one or both eyes.
Recent studies show that keratoconus affects about 289.1 individuals per 100,000 globally, with a noticeable rise in cases among young adults aged 20 to 29. It’s important to recognize that the financial burden of treating keratoconus has also increased significantly. In 2019, the average lifetime cost of treatment was estimated at $28,766.69, adjusted for inflation.
Awareness is crucial for recognizing its potential impact. Many individuals face difficulties with activities like reading, driving, and participating in sports. As one eye specialist noted, managing this condition can be both costly and time-consuming. This highlights the importance of early detection and intervention.
Real-world examples illustrate how keratoconus can disrupt daily routines, making awareness and education about it essential for those affected. If you’re experiencing keratoconus or other symptoms, we encourage you to seek professional medical help right away. Remember, you’re not alone in this journey; we are here to help you through the process.
Explore Causes: What Triggers Keratoconus?
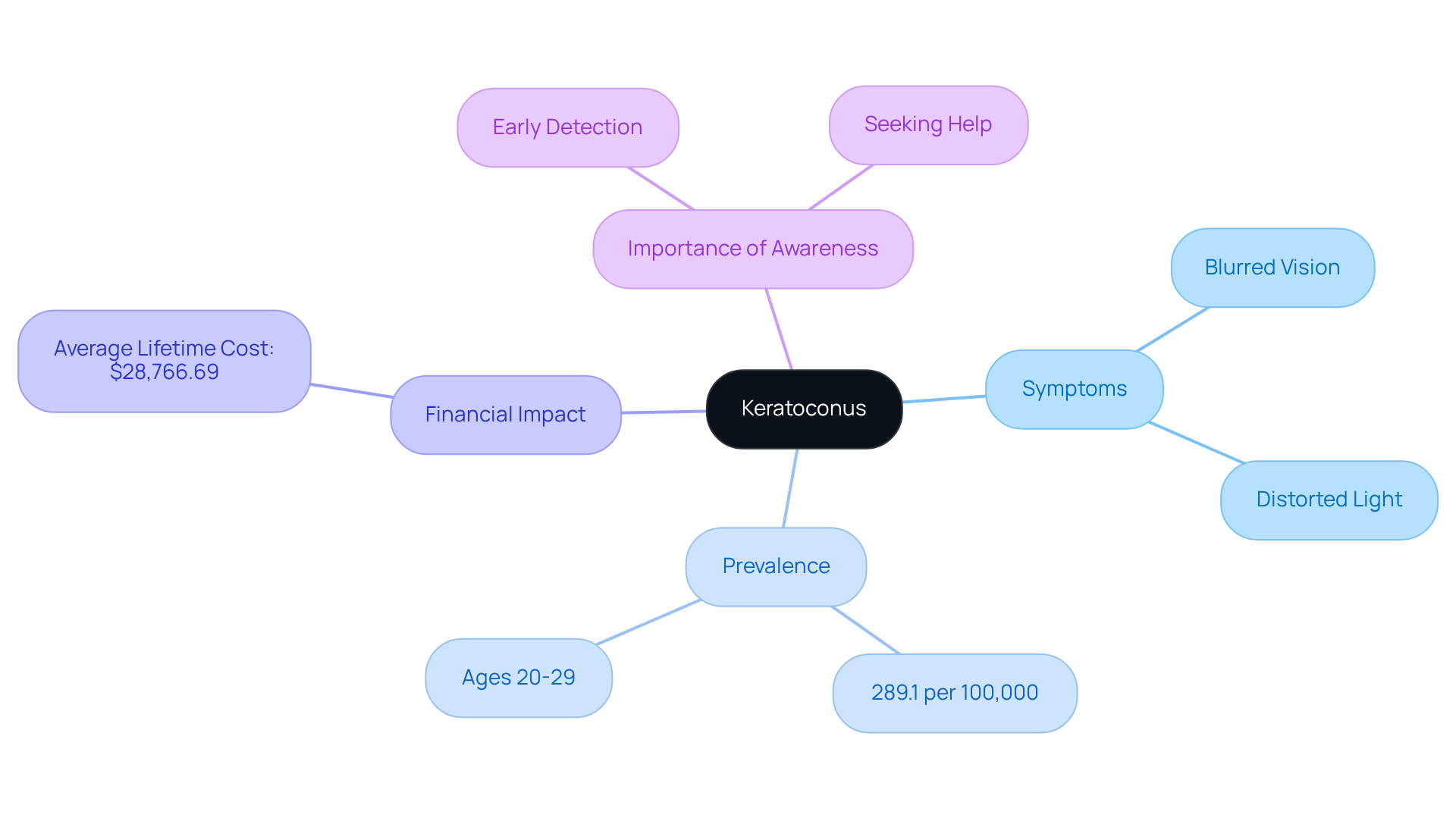
We understand that the exact cause of this eye condition can be confusing and concerning. While it’s not fully understood, it’s believed to stem from a mix of genetic and environmental factors. Many patients, about 10 to 15 percent, report a family history of the ailment, suggesting a hereditary component. For instance, a familial case study showed that three family members had both keratoconus and granular corneal dystrophy, hinting at a possible genetic link. Additionally, around 6-8% of individuals with this condition also have a positive family history, reinforcing the hereditary aspect.
Environmental triggers are also important to consider. Frequent eye rubbing is a common risk factor, with research showing that 87.4% of individuals with the condition engage in this behavior. Allergies and connective tissue disorders, like Marfan syndrome and Ehlers-Danlos syndrome, have been associated with the condition as well. Moreover, exposure to over 8 hours of sunlight each week is recognized as a risk factor. Understanding these environmental factors is crucial for those at risk, as taking proactive steps can help reduce the chances of developing the condition. Regular eye exams and early intervention are vital, especially for those with a family history, as timely diagnosis can significantly improve treatment outcomes.
The main symptoms of this condition include blurry or double vision, difficulty seeing at a distance, and light sensitivity. At Northwest Eye, your doctor may recommend specially fitted contact lenses to help with the corneal distortion caused by keratoconus. For more severe cases, a procedure called Corneal Collagen Cross-Linking might be suggested to stop the progression of the condition. As Khosrow Jadidi, an Associate Professor of Ophthalmology, notes, ‘The coexistence of corneal ectasia and granular dystrophy raises the possibility of a genetic connection between the conditions.’
We are here to help you through this process, and we encourage you to reach out if you have any questions or concerns.
Identify Symptoms: Recognizing Keratoconus Signs
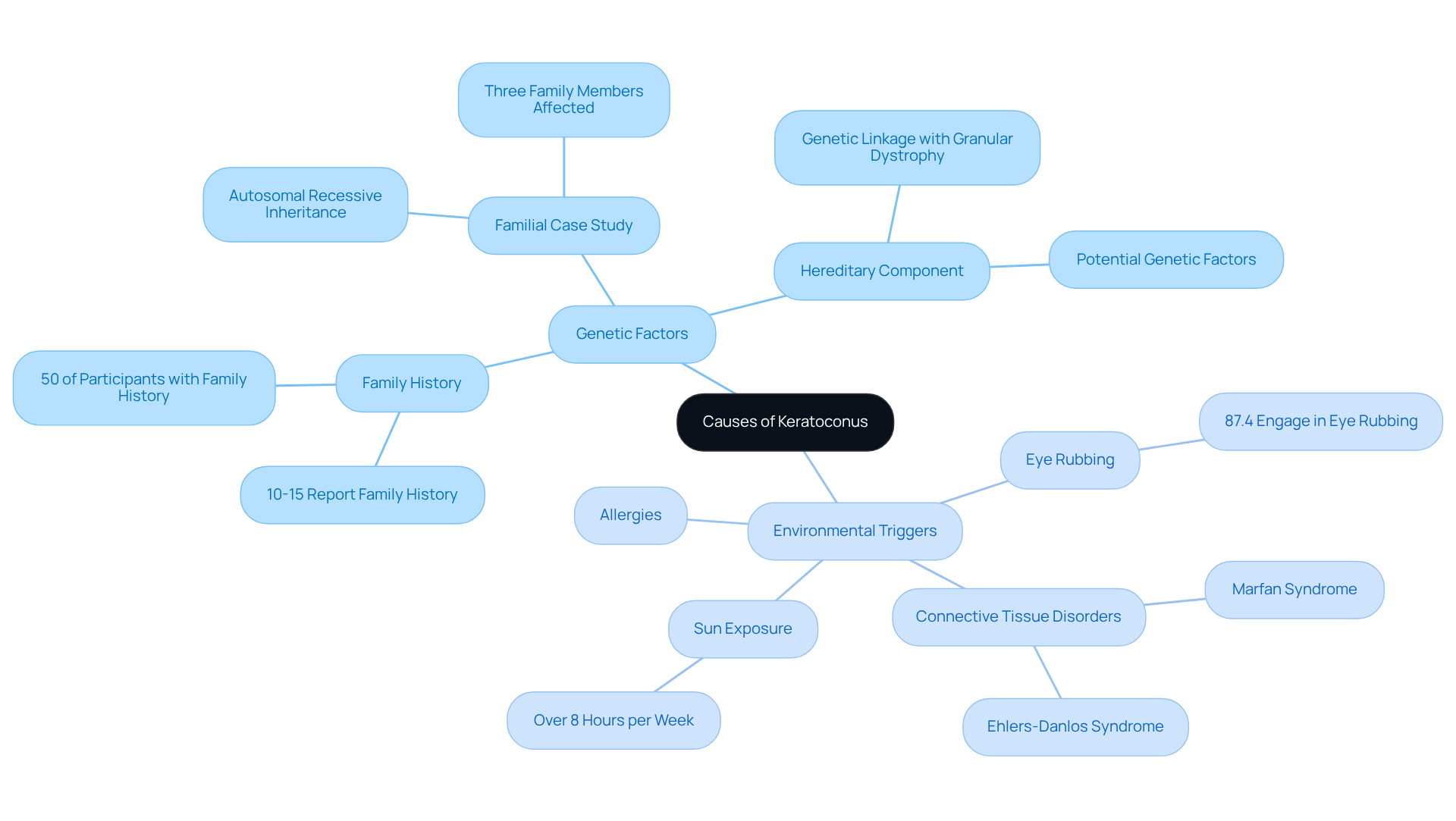
Symptoms of keratoconus often emerge gradually, and we understand how they can significantly impact your daily life. Here are some key indicators to watch for:
- vision that standard glasses can’t correct.
- Increased sensitivity, making bright environments uncomfortable.
- perception of halos or ghosting around lights as your sight may fluctuate unpredictably.
- Difficulties with frequent changes in eyeglass prescriptions, which can lead to challenges in low-light conditions.
- The sensitivity to light and glare, especially noticeable when driving at night.
Early recognition of symptoms related to keratoconus is crucial. They may signal the need for a diagnosis and potential treatment options. Research indicates that many individuals with keratoconus experience blurred vision, highlighting the importance of prompt intervention.
Eye care professionals are trained to identify these signs during routine exams. We are here to help you through this process, ensuring that you receive the care as soon as possible.
Understand Diagnosis: How Keratoconus Is Confirmed
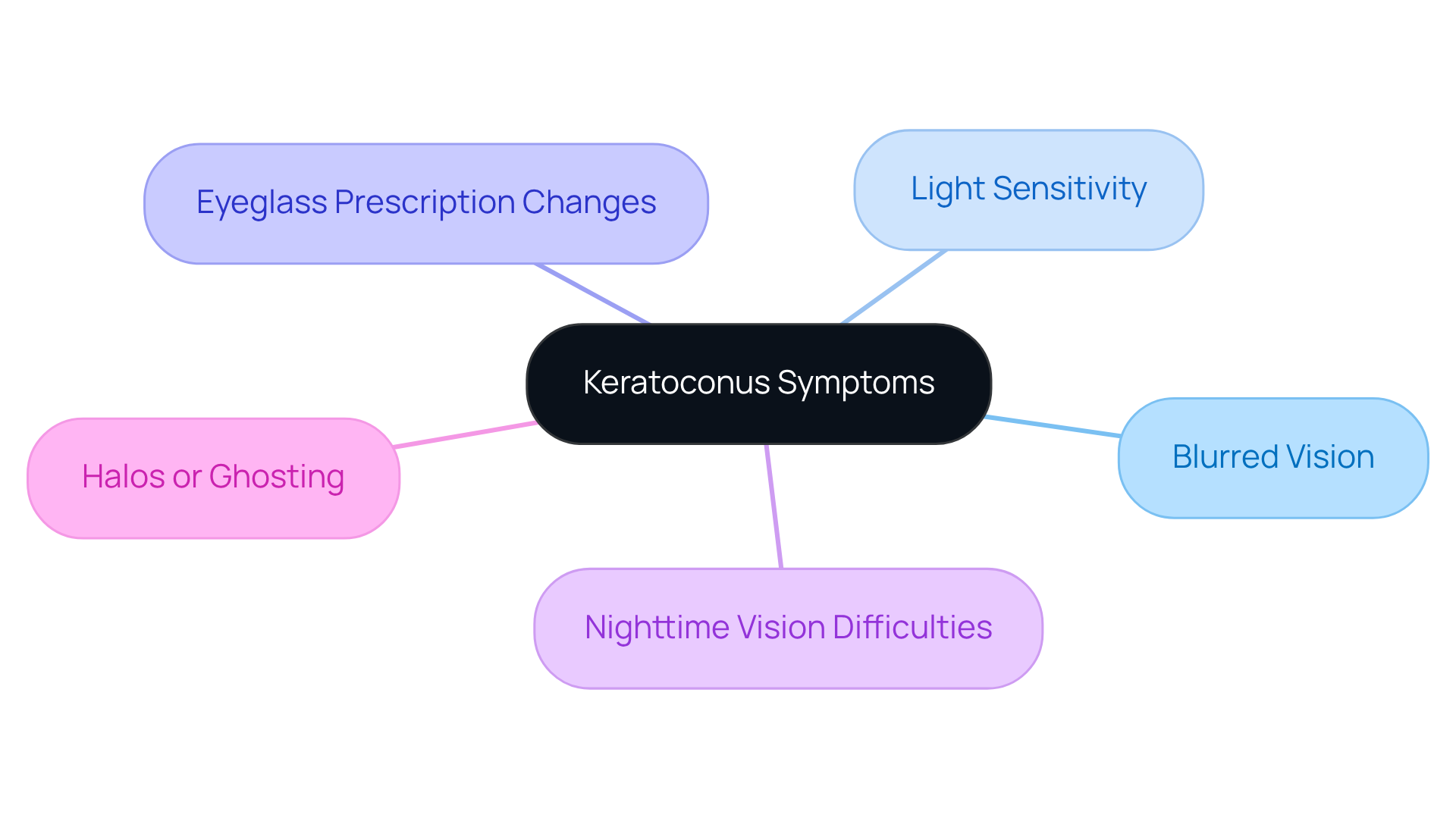
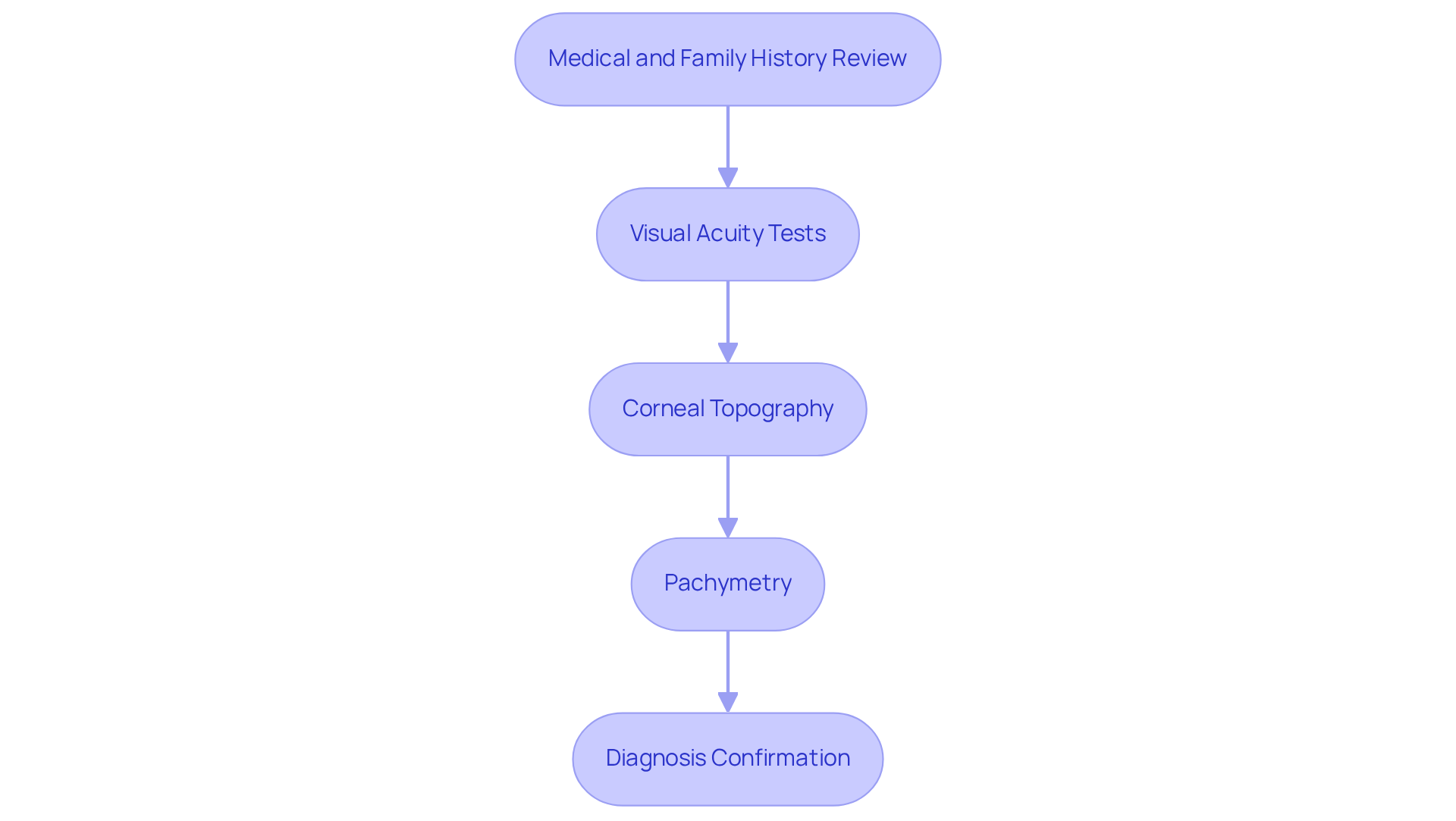
Diagnosing keratoconus can feel overwhelming, but we’re here to guide you through it. A thorough eye examination is essential, and it includes several important steps that help us understand your unique situation:
- around 13.3 cases of keratoconus per 100,000 people We start by discussing your medical background and any family history of eye conditions. This helps us identify potential risk factors, such as atopic diseases, that may be relevant to your diagnosis.
- importance of early detection and intervention These tests measure how sharp your vision is. Understanding how keratoconus affects your sight can help us address any challenges you face in your daily life.
- Medical and Family History Review This advanced technique maps the curvature of your cornea, revealing any irregularities that are characteristic of keratoconus thickness of your cornea. It’s particularly effective in detecting the condition early, even in cases that might have been previously overlooked. The health of your cornea is crucial, as it directly impacts the accuracy of this diagnostic method.
- Pachymetry: This measurement assesses the keratoconus eye disease, providing vital information about the severity of the disease. Variations in corneal thickness can significantly influence both diagnosis and treatment options.
Together, these diagnostic tools empower our ophthalmologists to confirm the presence of keratoconus and evaluate its severity. This is essential for tailoring the right treatment plan for you. Each year, we identify new cases, highlighting the visual acuity tests.
We understand that navigating this process can be daunting, but rest assured that these techniques not only help verify the condition but also play a crucial role in managing it effectively. Remember, we are here to help you through this journey.
Review Treatment Options: Managing Keratoconus Effectively
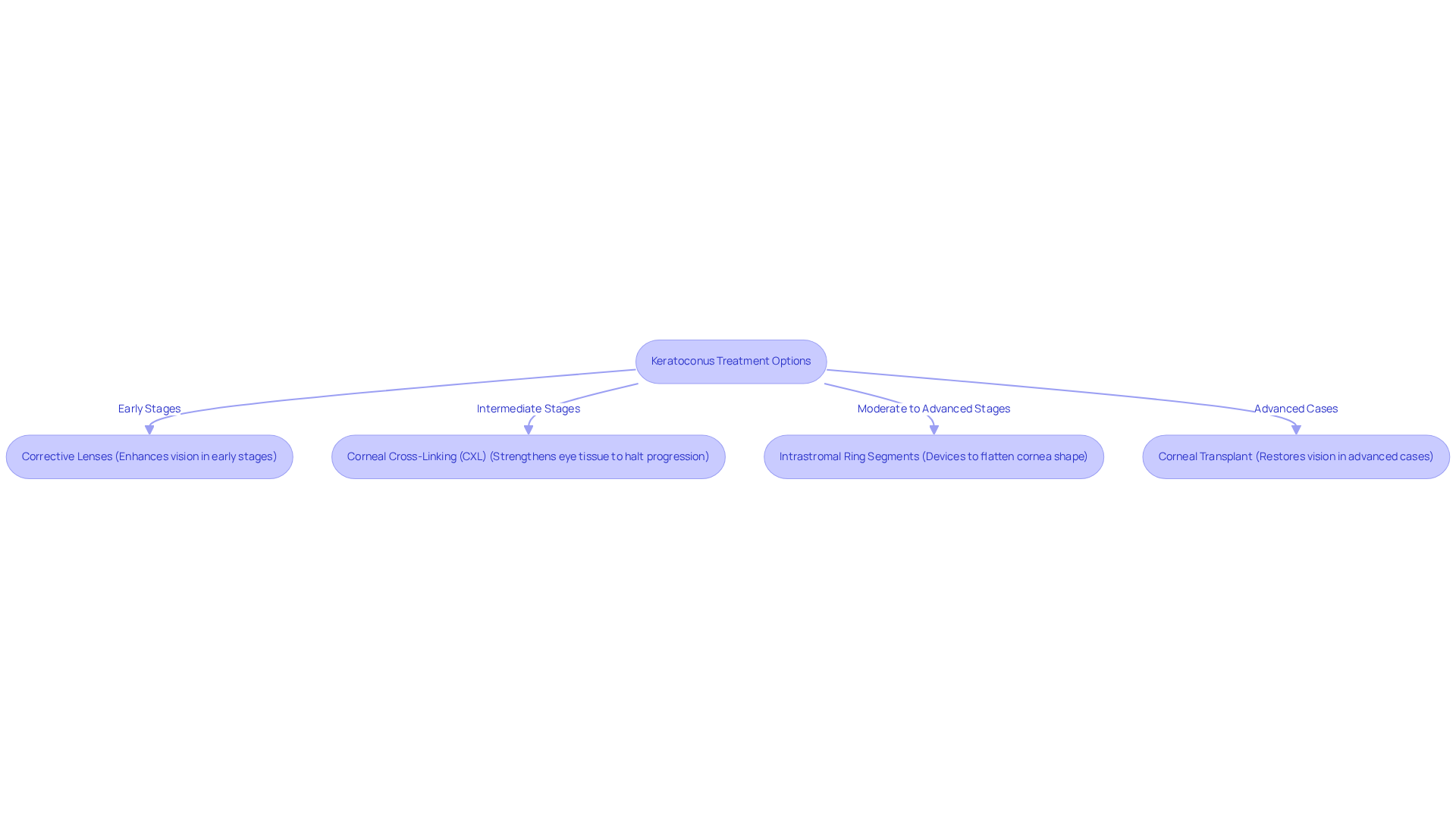
We understand that dealing with keratoconus can be challenging, and it’s important to know that resources are available to help you. Here’s a look at some of the approaches that may be recommended based on the severity of your condition:
- Glasses can halt the progression of keratoconus. In the early stages, glasses or contact lenses can significantly enhance your vision, providing a clearer view of the world around you.
- Corneal cross-linking (CXL): This procedure is designed to strengthen the eye tissue, helping to stabilize the condition. A personalized approach is essential for effective treatment. Many patients find reassurance in knowing that this option can stabilize their condition.
- Intrastromal ring segments are available. These are small devices inserted into the cornea to flatten its shape, which can improve your sight. It’s a minimally invasive option that many have found beneficial.
- In more advanced cases, a corneal transplant may be necessary to restore vision. While this may sound daunting, it can be a life-changing procedure for those who need it.
Each treatment option comes with its own benefits and risks, and we believe that a comprehensive plan is essential for achieving the best outcomes. Remember, you’re not alone in this journey; we are here to help you through the process and support you every step of the way.
Conclusion
Keratoconus is a complex eye condition that truly deserves our attention and understanding. As a progressive disorder, it involves the thinning and bulging of the cornea, which can lead to significant vision impairment. We understand that early detection and intervention are crucial for managing symptoms and improving the quality of life for those affected. Awareness of keratoconus, its causes, and treatment options is vital for individuals at risk and their families.
This article highlights several key aspects of keratoconus, including:
- Potential genetic and environmental triggers
- Common symptoms that signal its onset
- The critical diagnostic processes that can confirm its presence
From corrective lenses to advanced procedures like corneal cross-linking and transplants, various treatment options are available, each tailored to the severity of the condition. Understanding these elements empowers individuals to seek timely medical advice and interventions.
Ultimately, the significance of awareness and education about keratoconus cannot be overstated. By recognizing symptoms early and understanding the available treatment options, individuals can take proactive steps towards maintaining their vision and overall well-being. If you notice any signs of keratoconus, consulting with an eye care professional is essential for effective management and support. Remember, we are here to help you through this process.
Frequently Asked Questions
What is keratoconus?
Keratoconus is a progressive eye disorder characterized by the thinning and bulging of the cornea, causing a cone-like shape that distorts how light enters the eye, leading to blurred and altered vision.
At what age does keratoconus typically appear?
Keratoconus usually appears during adolescence or early adulthood and can progress over time, affecting one or both eyes.
How common is keratoconus?
Keratoconus affects approximately 289.1 individuals per 100,000 globally, with a notable increase in cases among young adults aged 20 to 29.
What are the financial implications of treating keratoconus?
The average lifetime cost of treating keratoconus was estimated at $28,766.69 in 2019, adjusted for inflation, indicating a significant financial burden for those affected.
What are the main symptoms of keratoconus?
The main symptoms include blurry or double vision, difficulty seeing at a distance, and light sensitivity.
What causes keratoconus?
The exact cause of keratoconus is not fully understood, but it is believed to result from a combination of genetic and environmental factors, such as frequent eye rubbing and certain connective tissue disorders.
Is there a hereditary component to keratoconus?
Yes, about 10 to 15 percent of patients report a family history of keratoconus, suggesting a genetic link.
What environmental factors are associated with keratoconus?
Environmental triggers include frequent eye rubbing, allergies, connective tissue disorders, and exposure to over 8 hours of sunlight each week.
How can keratoconus be treated?
Treatment options may include specially fitted contact lenses to address corneal distortion, and for more severe cases, a procedure called Corneal Collagen Cross-Linking may be recommended to halt the progression of the condition.
What should I do if I experience symptoms of keratoconus?
If you are experiencing blurred vision or other symptoms, it is important to seek professional medical help right away for proper diagnosis and intervention.
List of Sources
- Define Keratoconus: Understanding the Condition
- Checking your browser – reCAPTCHA (https://pubmed.ncbi.nlm.nih.gov/40833011)
- Prevalence of Keratoconus is 10x Higher Than Previously Thought (https://modernod.com/editorial-series/significant-findings/prevalence-of-keratoconus-is-10x-higher-than-previously-thought/37745)
- Keratoconus Global Burden More Than Doubled Since Analysis Published in 2020 (https://optometryadvisor.com/news/keratoconus-global-burden-more-than-doubled-since-analysis-published-in-2020)
- Keratoconus: U.S. Prevalence and Economic Burden (https://aao.org/eyenet/article/keratoconus-prevalence-economic-burden)
- Incidence and Prevalence of Keratoconus Rises Globally (https://reviewofoptometry.com/news/article/incidence-and-prevalence-of-keratoconus-rises-globally)
- Explore Causes: What Triggers Keratoconus?
- Longdom Publishing SL | Open Access Journals (https://longdom.org/open-access/familial-case-of-keratoconus-with-corneal-granular-dystrophy-in-a-family-of-iranian-origin-49835.html)
- Is Keratoconus Genetic? Understanding the Role of Family History (https://myclarityeyecare.com/is-keratoconus-genetic-understanding-the-role-of-family-history.html)
- Incidence and Prevalence of Keratoconus Rises Globally (https://reviewofoptometry.com/news/article/incidence-and-prevalence-of-keratoconus-rises-globally)
- Hereditary Predisposition Raises Keratoconus Risk (https://ophthalmologyadvisor.com/news/study-finds-data-accenting-genetics-in-corneal-disease-origin)
- Prevalence of Keratoconus and Associated Risk Factors Among High School Students in Couva, Trinidad: A Cross-Sectional Study | MDPI (https://mdpi.com/2411-5150/9/4/89)
- Identify Symptoms: Recognizing Keratoconus Signs
- Keratoconus Global Burden More Than Doubled Since Analysis Published in 2020 (https://optometryadvisor.com/news/keratoconus-global-burden-more-than-doubled-since-analysis-published-in-2020)
- Prevalence of Keratoconus is 10x Higher Than Previously Thought (https://modernod.com/editorial-series/significant-findings/prevalence-of-keratoconus-is-10x-higher-than-previously-thought/37745)
- Keratoconus: U.S. Prevalence and Economic Burden (https://aao.org/eyenet/article/keratoconus-prevalence-economic-burden)
- Cornea Research Foundation of America – Keratoconus (https://cornea.org/learning-center/conditions-research-areas/keratoconus.aspx)
- mayoclinic.org (https://mayoclinic.org/diseases-conditions/keratoconus/symptoms-causes/syc-20351352)
- Understand Diagnosis: How Keratoconus Is Confirmed
- Cornea Research Foundation of America – Keratoconus (https://cornea.org/learning-center/conditions-research-areas/keratoconus.aspx)
- Keratoconus Global Burden More Than Doubled Since Analysis Published in 2020 (https://optometryadvisor.com/news/keratoconus-global-burden-more-than-doubled-since-analysis-published-in-2020)
- Keratoconus: U.S. Prevalence and Economic Burden (https://aao.org/eyenet/article/keratoconus-prevalence-economic-burden)
- Age-specific Incidence and Prevalence of Keratoconus: A Nationwide Registration Study – PubMed (https://pubmed.ncbi.nlm.nih.gov/28039037)
- Incidence and Prevalence of Keratoconus Rises Globally (https://reviewofoptometry.com/news/article/incidence-and-prevalence-of-keratoconus-rises-globally)
- Review Treatment Options: Managing Keratoconus Effectively
- Corneal Cross-Linking Guide: Everything You Need to Know (https://nvisioncenters.com/corneal-cross-linking)
- What is the success rate of corneal cross-linking? (https://oculase.com/treatments/keratoconus-treatment/answerpack/keratoconus/keratoconus-faqs/what-is-the-success-rate-of-corneal-cross-linking)
- Promising New Procedure for Keratoconus (https://modernod.com/editorial-series/significant-findings/a-less-risky-procedure-for-patients-with-keratoconus/37760)
- CXL for Corneal Ectasia: Reshaping the Future of Treatment (https://aao.org/eyenet/article/cxl-corneal-ectasia-reshaping-future-of-treatment-2)
- Repeat corneal collagen cross-linking after failure of primary cross-linking in keratoconus (https://bjo.bmj.com/content/108/5/662)






